Model relies on analysis of peri-ictal scalp EEG data, promising wide applicability
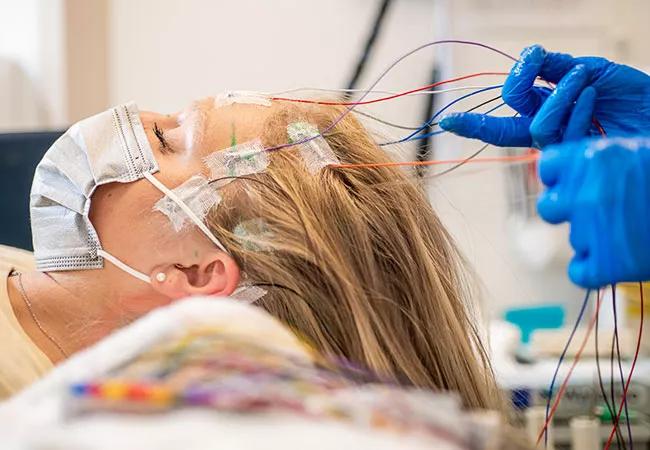
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/da80a827-f26e-4ca7-aab5-1490e00d929c/22-NEU-3183518-CQD-Hero-650x450-1_jpg)
scalp EEG electrodes on a woman's head
A machine learning algorithm combining clinical variables and peri-ictal scalp EEG recordings shows promise for predicting seizure outcomes following brain resection with high accuracy, report Cleveland Clinic researchers in a new study in Nature Scientific Reports.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“We found that application of our predictive model could reduce unsuccessful brain resections by 20% in patients with drug-resistant epilepsy [DRE],” says senior author Lara Jehi, MD, an epilepsy specialist who also serves as Cleveland Clinic’s Chief Research and Information Officer and Director of the Center for Computational Life Sciences. “Moreover, this approach is highly clinically translatable, as scalp EEG is noninvasive, inexpensive and acquired for epilepsy surgery patients all over the world.”
More than 20 million people worldwide suffer from uncontrolled seizures caused by DRE. Resective epilepsy surgery — most commonly temporal lobe resection — is the gold standard therapy to permanently stop seizures, but only half of surgical patients achieve long-term seizure freedom. Researchers around the world have tried to identify the factors most predictive of which patients will experience sustained freedom from seizures after surgery.
In 2015, Cleveland Clinic Epilepsy Center staff created an evidence-based risk prediction model to predict epilepsy surgery outcomes. The publicly available nomograms, spearheaded by Dr. Jehi, use simple clinical variables that are a standard part of presurgical care and can accurately predict surgical outcome (success or failure in achieving seizure freedom) in about 70% of cases. These online risk calculators are currently used around the world for presurgical decision-making and patient counseling.
However, efforts to build more accurate predictive frameworks have continued by incorporating more granular patient-specific data, a task that may be suited to novel artificial intelligence methods. Success in prediction has been challenging, as accuracy has generally hovered around 80% even with the best frameworks, save for rare models that use data obtained through complex imaging or invasive brain recordings, which limits these models’ potential to be translated to mainstream clinical practice.
Advertisement
“Brain surgery for epilepsy is the last option for many patients who suffer from debilitating seizures, so it’s critical to be as informed as possible before the procedure itself,” says co-investigator Carl Saab, PhD, of the Department of Biomedical Engineering in Cleveland Clinic Lerner Research Institute. “It can be devastating for these patients to face a 50% chance of recurring seizures after they go through all the risks, time and costs of surgery.”
As technology evolves, researchers are updating their risk prediction strategies. Shehryar Sheikh, MD, the study’s first author and a neurosurgery resident physician, had an idea for a risk prediction model using machine learning and scalp EEG. He collaborated with colleagues in Cleveland Clinic’s Epilepsy Center and Lerner Research Institute to determine and refine which data to use.
“The exciting thing about our model is that scalp EEGs are universal,” Dr. Sheikh explains. “Every patient who undergoes surgery, no matter where they are, undergoes a scalp EEG. This means there will be no extra burden to providers, and this model can be easily implemented to help ensure the right patients are selected for surgery.”
The researchers retrospectively analyzed a dataset of 294 patients who underwent temporal lobe resection for DRE at Cleveland Clinic over a recent 10-year period. EEG data had been captured through video EEGs taken in the epilepsy monitoring unit. Many patients experienced multiple seizures while under observation, so the team randomly selected one seizure from each patient for analysis.
Advertisement
After removing artifacts from the EEGs using a machine learning algorithm and completing additional pre-processing steps, the team ran multiple predictive models to identify which biomarkers from the EEG data were the best indicators of resection success or failure.
Results showed that EEG data taken during a five-minute peri-ictal window could reliably predict post-surgery outcomes. Using data collected two minutes before (pre-ictal) to three minutes after (post-ical) a seizure, the machine learning model was able to predict surgical outcome (success or failure) with accuracy of over 90%. Additional clinical variables did not impact the accuracy of the predictions.
When the researchers applied the innovative statistical approach known as decision curve analysis to quantify the clinical usefulness of EEG-augmented model, it showed that the model could reduce the rate of unsuccessful brain resections by 20% compared with prevalent nomograms based solely on clinical variables. “This is the first known application of decision curve analysis in the epilepsy field,” Dr. Jehi notes.
She says these findings offer promising news for patients. “This model’s accuracy surpasses by far the existing artificial intelligence models that have aimed to predict surgical outcomes,” she says, “including those that use much more complex inputs from much more expensive or invasive presurgical tests, such as functional MRI or stereoelectroencephalography. In contrast, this model uses universally available data.”
Advertisement
The investigators plan to continue their research by validating their results in external datasets and other patient populations.
Advertisement
Advertisement
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Early identification of temporal encephaloceles can improve surgical decision-making
Insights from one of the first studies of invasive monitoring in the rare form of focal cortical dysplasia
Novel Cleveland Clinic project is fueled by a $1 million NIH grant
Patients with epilepsy should be screened for sleep issues
Sustained remission of seizures and neurocognitive dysfunction subsequently maintained with cannabidiol monotherapy
Investigational gene approaches offer hope for a therapeutically challenging condition
Study combines intracranial electrophysiology and SPECT to elucidate the role of hypoperfusion