5% of flagged ECGs in real-world study were from patients with previously undiagnosed HCM
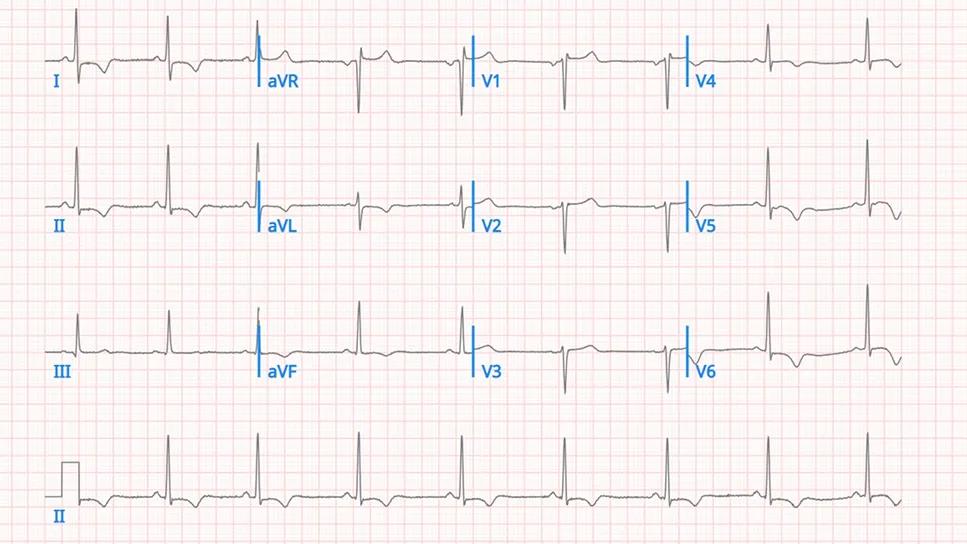
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/171de6f2-72e0-4821-ba2d-675316edeac8/ECG-suggesting-hypertrophic-cardiomyopathy)
electrocardiogram tracing
Use of artificial intelligence-enhanced 12-lead echocardiography (AI-ECG) was associated with a high degree of accuracy in detection of hypertrophic cardiomyopathy (HCM) in real-world clinical use, enabling identification of HCM in 5% of patients not previously diagnosed with HCM. So finds a prospective observational study reported by Cleveland Clinic researchers at the American College of Cardiology Scientific Session and published online in JACC Clinical Electrophysiology.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The findings of our real-world study suggest that clinical application of AI-ECG algorithms offers incremental diagnostic value in evaluating patients who might have HCM, enabling earlier disease detection and intervention, which improves the likelihood of successful treatment outcomes,” says principal investigator Milind Desai, MD, MBA, Director of Cleveland Clinic’s Hypertrophic Cardiomyopathy Center. “The algorithm we used performed well across patient subgroups differing by age, sex and whether or not patients had prior septal myectomy.”
HCM usually is diagnosed based on some combination of clinical evaluation, cardiac imaging methods such as echocardiography and cardiac magnetic resonance imaging (CMR), and genetic testing. Yet HCM patients can have no symptoms or nonspecific symptoms for considerable periods, and evidence indicates that nearly 85% of HCM cases are undiagnosed, underdiagnosed or misdiagnosed.
“In view of the considerable clinical implications of a delayed diagnosis or misdiagnosis of HCM for both patients and their at-risk family members, early and accurate diagnosis is a top priority,” Dr. Desai says.
More than 90% of patients with HCM have abnormal ECG findings, with the most common abnormalities being left ventricular hypertrophy, Q waves and repolarization abnormalities. Because these ECG findings are nonspecific and overlap with those of many other conditions, ECG screening alone has limited utility for detecting HCM, despite its low expense, noninvasive nature and wide availability.
Advertisement
To overcome the limits of standard ECG-based screening, convolutional neural networks have been used in recent years to develop AI-powered ECG algorithms for detecting HCM from 12-lead ECGs. Cleveland Clinic implemented one such algorithm (from Viz.ai, San Francisco) in February 2024 to assist in the diagnosis of HCM. “We undertook our study to evaluate the real-world clinical application of this algorithm in a large, undifferentiated patient population at our tertiary care center,” Dr. Desai notes.
Following implementation of the AI-ECG algorithm for routine clinical use, all ECGs performed in adult patients evaluated at Cleveland Clinic’s Main Campus underwent analysis by the algorithm in addition to standard ECG interpretation. The study included all first ECGs for the 45,873 consecutive adults evaluated during the first 8.5 months of the algorithm’s use. Other than exclusion of patients with pacemakers, there were no restrictions based on the presence or absence of a cardiovascular diagnosis.
The investigators assessed the AI-ECG algorithm’s diagnostic performance against clinical diagnoses using three different HCM probability thresholds: ≥0.95, ≥0.90 and ≥0.85 (within a range from 0 to 1).
Patients were divided into the following groups:
Advertisement
Clinical diagnoses were made by experienced cardiologists, whether for patients with a diagnosis of HCM (in both each of the first two groups above) or those with an alternative diagnosis excluding HCM.
Among the first ECGs analyzed for the study’s 45,873 patients, 1,265 (2.76%) were flagged by the algorithm for suspected HCM using the ≥0.85 probability threshold (i.e., the broadest threshold). The 1,265 patients with these flagged ECGs broke down as follows:
As expected, the algorithm’s accuracy varied by the chosen HCM probability threshold. Key observations included the following:
The algorithm performed similarly well in men and women, and it was more sensitive in patients under age 50 but more specific in those 50 or older. Among patients with previously diagnosed HCM, the algorithm performed similarly across all probability thresholds in patients regardless of whether or not they had undergone myectomy and whether or not they had received mavacamten therapy.
Advertisement
The 691 false-positive patients flagged for HCM had various alternate diagnoses, including aortic stenosis and hypertension. This suggests that concomitant secondary left ventricular hypertrophy can potentially confound the AI-ECG algorithm’s diagnosis of HCM, the researchers note.
“These findings suggest that AI-ECG can potentially offer a less costly and faster alternative to traditional screening tools like echocardiography and CMR in the initial evaluation for HCM,” Dr. Desai notes. He adds that the algorithm’s ability to flag 63 cases of undiagnosed HCM during this short study period — 5% of the total ECGs flagged — underscores its potential to improve patient outcomes through earlier HCM detection and treatment.
For example, Dr. Desai and colleagues recently reported the case of a patient who was diagnosed with obstructive HCM through the use of AI-ECG who has since been initiated on therapy with the novel agent mavacamten and has shown excellent clinical response (JACC Case Rep. 2025 Epub 26 Feb).
In their study report, the authors note that the ideal probability threshold to use when employing an AI-ECG algorithm may vary based on specific clinical context. For instance, a threshold of ≥0.95 has a high positive predictive value, suggesting particular utility when screening high-risk patients, such as those with a family history of HCM. In contrast, a threshold of ≥0.85-0.90 offers a low risk of missing actual HCM cases, but at the expense of excess false-positives. Such a threshold could be useful when screening a lower-risk population like young athletes, in whom HCM is the most common cause of sudden cardiac death.
Advertisement
“The symptoms of HCM can be nonspecific, and often other diagnoses — both cardiac and noncardiac — are entertained,” observes study co-author Maran Thamilarasan, MD, staff cardiologist in Cleveland Clinic’s Section of Cardiovascular Imaging. “If AI-enhanced ECG can alert to the possibility of this diagnosis, as this study suggests is the case, this can lead to earlier appropriate diagnostic testing and treatment.”
Dr. Desai is a consultant to and has research agreements with Viz.ai as well as several pharmaceutical companies. No external funding or industry support was used in the conduct of the study reported here, which was fully funded by philanthropic support for Dr. Desai’s research. Dr. Thamilarasan reported no potential conflicts of interest.
Image at top is reprinted from Desai et al., JACC: Case Reports (2025 Epub 26 Feb), under the Creative Commons CC-by-NC-ND license.
Advertisement
End-of-treatment VALOR-HCM analyses reassure on use in women, suggest disease-modifying potential
Cardiac imaging substudy is the latest paper originating from the VANISH trial
Vigilance for symptom emergence matters, a large 20-year analysis reveals
Phase 3 ODYSSEY-HCM trial of mavacamten leaves lingering questions about potential broader use
High composite score in myectomy specimens signals worse prognosis
Few patients report left ventricular dysfunction or heart failure after one year
Avoidance of septal reduction therapy continues while LVEF dysfunction remains infrequent
New risk score pools factors that may predict adverse outcomes in the uncommon phenotype