We now have an expanded toolbox to extend survival and lessen treatment toxicity
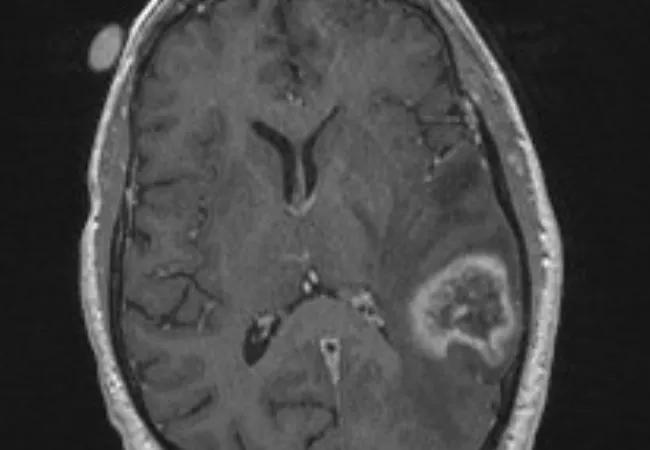
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f193bd96-a99d-45bf-af07-fabad1398600/22-NEU-2909543-brain-metastasis_650x450-1_jpg)
MRI of a patient with brain metastases
By Lilyana Angelov, MD; Samuel Chao, MD; and Marc Shapiro, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Nearly half of all brain metastases are associated with an underlying cancer diagnosis, and lung cancer is one of the most common of these. As improved cancer therapies are helping patients live longer, the safe and effective management of lung cancer brain metastases is coming to the fore. The goals we always keep in mind in these cases are to extend survival, prevent neurological dysfunction and improve quality of life. This article briefly reviews progress toward these goals made in recent years.
Surgery can be essential for making a diagnosis, maximizing resection of a solitary metastasis and improving survival. It offers many advantages over other management strategies: not only is the cancer locally removed, but the associated rapid resolution of mass effect and edema many times improves neurological issues and allows for faster tapering of corticosteroids used to treat symptomatic lesions.
Surgical risk can be reduced and neurological deficits minimized by using the following tools and strategies:
In most cases, adding whole brain radiation therapy (WBRT) or stereotactic radiosurgery to surgery has been essential to increase survival and reduce tumor recurrences.
Sometimes open surgery is not necessary; however, a biopsy may be required to confirm the tumor diagnosis and guide patient management.
Whole brain radiation therapy. For decades, WBRT was considered standard treatment for patients with brain metastases. While 70% to 90% of patients experience improved symptoms in one to three weeks, toxicity — including alopecia, fatigue, skin erythema, headache, otitis media, somnolence syndrome and leukoencephalopathy — is common.
Advertisement
Most importantly, WBRT is associated with neurocognitive decline, which becomes more evident as patients live longer than one year. This risk can be lowered by newer approaches such a medications (e.g., memantine) or modified radiation delivery such as hippocampal sparing during WBRT; however, delayed impact on cognition continues to be a factor.
This concern regarding delayed toxicity has reduced the role of WBRT in recent years. WBRT is still considered necessary for leptomeningeal disease and for cases involving numerous metastatic lesions, although the threshold is not well defined and is rising as other therapies prove effective for multiple metastases. WBRT is also traditionally standard for small cell lung cancer (SCLC) brain metastases, but evidence now indicates that stereotactic radiosurgery alone may be sufficient, if not favored, for up to 10 lesions.
Stereotactic radiosurgery. Stereotactic radiosurgery offers multiple advantages over many other therapies, including lower cost and, in most cases, avoidance of general anesthesia for surgery. It involves a minimally invasive or noninvasive outpatient procedure with no meaningful recovery time. Additionally, in contrast to some of the limitations encountered with open surgery, stereotactic radiosurgery can safely treat lesions that are small, deep or near critical areas.
Already the standard for limited small brain metastases, stereotactic radiosurgery has increasingly been used over the past few years as primary treatment for patients with up to 15 tumors and for large lesions. It also can be used as salvage treatment for recurrence of metastases following WBRT. Comparable to WBRT in terms of overall survival and local and distant control, it allows faster time to systemic therapy and causes fewer toxicities, including neurocognitive impairment.
Advertisement
For large brain metastases (≥ 2 cm), single-session radiosurgery does not consistently provide durable control. Instead, we recommend staged treatment — i.e., two stereotactic radiosurgery treatments performed one month apart — effectively boosting the target and achieving approximately 90% one-year local control. This strategy capitalizes on tumor volume shrinkage that is often observed between sessions, reducing the irradiated volume and possibly making the tumor more responsive to the next treatment. Systemic therapy is allowable between the two treatments. We have found this approach feasible, safe and effective, obviating the need for surgical intervention even for large brain metastasis in select cases.
Radiation necrosis (a delayed impact of radiation treatment seen in 5% to 10% of patients) remains a concern following both WBRT and stereotactic radiosurgery, especially as it can be clinically and radiologically difficult to distinguish from recurrent tumors. We closely monitor all patients with MRI after radiation therapy to detect suspicious lesions early, as well as for radionecrosis when it is more likely to be limited and even reversible if treated promptly.
In recent years, we have changed how we treat non-small cell lung cancer (NSCLC) tumors driven by epidermal growth factor receptor (EGFR) mutations or anaplastic lymphoma kinase (ALK) rearrangements, and this has had significant impact on control of lung cancer-related brain metastases.
Prior to 2015, the tyrosine kinase inhibitors (TKIs) used for targeted therapy of NSCLC offered very good systemic control but very little control of brain metastases. Since 2015, TKIs with CNS activity have become available and have quickly moved from second-line to frontline therapy. We now even have data supporting adjuvant use of one TKI, osimertinib, for EGFR-positive tumors. These developments have given us the welcome option of withholding WBRT in TKI-naïve patients.
Advertisement
How do we use these drugs? In cases of EGFR– or ALK-driven tumors with brain metastases, virtually all patients who are TKI-naïve receive TKI therapy plus stereotactic radiosurgery. The first-line TKI is osimertinib for those with EGFR-positive tumors and alectinib for those with ALK-positive tumors.
If disease progression occurs, for EGFR-positive tumors we will continue osimertinib if there are two or fewer lesions and extracranial control is being achieved. If there are multiple lesions and extracranial control is being lost, we continue with stereotactic radiosurgery alone and decide whether and when to add chemotherapy. For disease progression in patients with ALK-positive tumors, alectinib may be followed by the second-line TKI lorlatinib before considering switching to chemotherapy.
For patients with tumors with no driver mutations, immunotherapy with a checkpoint inhibitor — with or without chemotherapy — is used in addition to stereotactic radiosurgery.
Whether and when we can use systemic therapy alone is a key research question currently under study. Given the known benefits from local therapy, many oncologists are understandably reluctant to use systemic therapy alone, even though the appeal of systemic therapy is compelling, given its potential impact on controlling the disease throughout the body. However, there continue to be multiple unknowns regarding the timing and sequence of systemic therapy in relation to stereotactic radiosurgery or WBRT, as well as regarding the advisability of trying another TKI if CNS progression occurs.
Advertisement
Even as the field grapples with these questions, the progress of the past few years — particularly the advent of systemic therapies and improvements in the use of stereotactic radiosurgery — deserves recognition. These advances underscore the importance of multidisciplinary expertise in the management of lung cancer brain metastases. And with so much still unknown despite these advances, the need for a multidisciplinary team approach to optimize individual treatment strategies may be the greatest imperative of all.
Dr. Angelov is a neurosurgeon in Cleveland Clinic’s Rose Ella Burkhardt Brain Tumor and Neuro-Oncology Center and Director of Cleveland Clinic’s Gamma Knife Center. Dr. Chao is a radiation oncologist in the Burkhardt Brain Tumor and Neuro-Oncology Center and Associate Director of the Gamma Knife Center. Dr. Shapiro is a medical oncologist in the Department of Solid Tumor Oncology in Cleveland Clinic’s Taussig Cancer Institute.
Advertisement
Largest study to date comparing direct-acting oral anticoagulants to low-molecular-weight heparin
Research demonstrates improved overall survival for patients receiving comprehensive treatment for breast cancer in addition to radiation or surgical intervention for brain cancer
Improvements enable targeting of brain tumors with single-session, fractionated or neoadjuvant approaches
This approach led to local control for patients with brain metastases more than 2 cm in diameter
Study uses molecular and clinical stratification to help guide patient selection
Phase 3 STELLAR trial underscores role of molecular stratification in glioma care
Phase 2 trials investigate sitagliptin and methimazole as adjuvant therapies
Large retrospective study suggests DOACs are safe, effective alternative to low-molecular-weight heparin in complex patient population