ONS shown to be successful
Around 2 percent of the general population is affected by chronic migraine, the most disabling type of chronic headache. Migraine is among the top three reasons people miss work, after the flu and before back pain. It has a major impact on the economy and people’s overall quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
At Cleveland Clinic, Nagy Mekhail, MD, PhD, Director of Evidence-Based Medicine in the Department of Pain Management, has helped dozens of patients with chronic headache in recent years with peripheral nerve stimulation, specifically occipital nerve stimulation (ONS). ONS puts an electric field around the occipital nerve and stops the pain signal from firing.
For patients with chronic migraine who have failed aggressive pharmaceuticals and other treatment modalities, ONS is an emerging treatment modality.
“Neuromodulation for intractable migraine is very effective and cost-effective for properly selected patients,” says Dr. Mekhail. He and his team at the Pain Management Department at Cleveland Clinic recently conducted a study to gather evidence showing that ONS is an effective long-term treatment for chronic migraine.
At Cleveland Clinic, 20 patients were implanted with a neurostimulation system, randomized to an active or control group for 12 weeks. For an additional 40 weeks, they received open-label treatment and the team looked at outcomes, including number of headache days, pain intensity, Migraine Disability Assessment (MIDAS), Zung Pain and Distress (PAD), direct patient reports of headache pain relief, quality of life, satisfaction and adverse events.
This analysis compared the outcomes of a multicenter study of ONS to one site, in hopes of finding differences in outcomes and adverse events. Cleveland Clinic results showed that headache days per month were reduced by 8.51 (9.81) days (P < 0.0001). The proportion of patients who achieved a 30 percent and 50 percent reduction in headache days and/or pain intensity was 60 percent and 35 percent, respectively. MIDAS and Zung PAD were reduced for all patients.
Advertisement
Patient selection for this procedure is key to its success, Dr. Mekhail stresses. He notes that an advantage at Cleveland Clinic has been the teamwork between the Pain Management Department and the Headache Center. Physicians of the Cleveland Clinic Headache Center, who are very familiar with each patient case, can refer the proper patients for this procedure. From there, the experience of the implanting physician helps to ensure the success of the procedure.
He notes that further research is needed into both technology and implantation techniques. He is currently working with his team to put together a five center feasibility study. Currently they are working on the final protocol, with the goal of starting this year.
Advertisement
Advertisement

Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies

Study participants also reported better sleep quality and reduced use of pain medications

Two-hour training helps patients expand skills that return a sense of control
Program enhances cooperation between traditional and non-pharmacologic care

National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
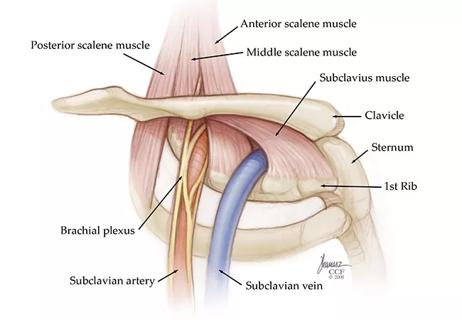
Pain specialists can play a role in identifying surgical candidates
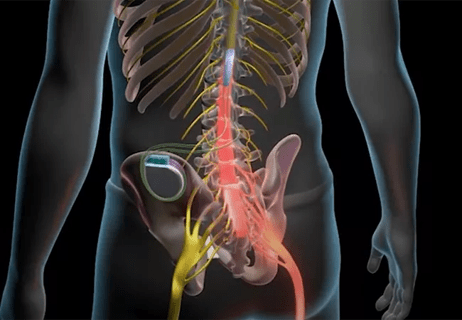
Individual needs should be matched to technological features
New technologies and tools offer hope for fuller understanding