The device is a less invasive alternative for patients who are struggle with chronic pain
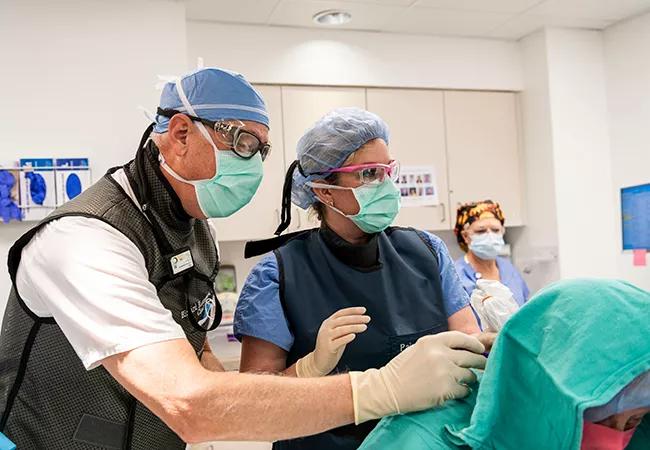
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/719d1a31-514e-4fd5-83fc-930f5b161cf5/21-PAI-2140696-CQD-650x450-1_jpg)
peripheral nerve stimulation device
A 44-year-old patient had right foot surgery and developed peripheral nerve injury. The patient experienced progressive pain and disability in terms of being able to walk, stand and perform other daily activities. She failed to get significant improvement with physical therapy (PT) and medical management alone. She was given nerve blocks and had some temporary improvements lasting about a month. This allowed her to increase her PT and incorporate water-based therapies into her treatment. The patient began to be able to do more things that she could do before, but it was still not at the level she wanted.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The patient consulted with Richard W. Rosenquist, MD, who suggested peripheral nerve stimulation. A stimulating needle was directed towards the patient’s deep peroneal nerve using ultrasound guidance. After it was located and stimulation was obtained, the stylet was removed, and Dr. Rosenquist threaded a percutaneous sleeve containing a micro lead through the needle and made sure that the patient was still receiving stimulation in the correct area. The needle was removed, and tiny remote control battery pack was attached to the patient’s leg. The patient had multiple programs to stimulate that nerve over the course of many weeks.
The patient had 90% to 100% relief of pain. She was able to participate in physical therapy, markedly increase her physical activity and come off of medications. The patient was very pleased with her response to the device and the overall improvement in function.
Dr. Rosenquist notes that peripheral nerve stimulation may be a good option for select patients who have struggled with chronic pain and have not found the relief they were looking for after other treatments. The device is relatively newer, and although the body of experience with peripheral nerve stimulation isn’t as extensive as it is for spinal cord stimulation, Dr. Rosenquist reports positive results for these patients.
“We’ve got many decades worth of experience with spinal cord stimulation and with the fully implanted devices,” says Dr. Rosenquist. “With these temporary peripheral nerve stimulators, it’s probably not even 10 years’ worth of experience. But they’re a nicer alternative because it’s not a permanent implant, so they’re a lot less invasive. If you can get something that somebody wears for two months—the approval for this particular device suggests stimulation for 60 days—and gets prolonged relief out of doing so, that’s wonderful. Plus, they’re being applied in a wide variety of areas of the body.”
Advertisement
While patients who are good candidates often find long-lasting relief, it can be difficult to identify those patients during the screening process. Dr. Rosenquist believes this is due to the smaller body of literature and experience with the device that means the patient selection criteria isn’t as fully developed yet. “I’ve had a couple people where we were never able to get great relief, and I’ve got others who have had tremendous relief. One of the drawbacks for something relatively new is you don’t have the patient selection criteria as finely tuned as you’re going to have when you’ve got much more experience and people have done more rigorous studies. So right now, some of it is a little bit of gestalt in the sense that I’ve done blocks, the patient got good temporary relief, but it wasn’t durable. So we end up trying something in between a block and a fully implanted system.”
Because these devices are temporary, they do not require the same full psychological evaluation required for a fully implanted device. But Dr. Rosenquist suggests that you still want people whose history, physical exam and any imaging studies all make sense and are concordant with the other pieces of information available.
Dr. Rosenquist often uses peripheral nerve stimulation as a tertiary option. Typically, patients will try medical management or a peripheral nerve blocks with local anesthetic and steroid first. If they get to the point where peripheral nerve blocks with local anesthetic and steroid provide good but only short-term relief, then the physician might think about doing something like peripheral nerve stimulation to see if the patient gets sustained relief through neuromodulation with electrical current.
Advertisement
For patients who are good peripheral nerve stimulation candidates, relief can be felt quite soon after implantation. Usually within a day or two, people are starting to notice significant relief,” says Dr. Rosenquist. “It’s not something where you have to wait a long time to see whether or not you’re getting a response to this particular device. The utility and applicability of these devices is something that is evolving. And, for some of these patients where the injury involves a small peripheral nerve, those things might not have been targeted in the past. Certainly for the nerve that we targeted with this patient, it would have probably been out of the scope of a traditional fully implanted device. But now, all we need to do is target this one specific peripheral nerve branch. This is a new device with new capabilities, and along with the use of ultrasound imaging to visualize nerves, we’re able to do some things that were not possible in the past.”
Advertisement
Advertisement
What the postoperative data show so far
Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies
Study participants also reported better sleep quality and reduced use of pain medications
Two-hour training helps patients expand skills that return a sense of control
Program enhances cooperation between traditional and non-pharmacologic care
National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
Pain specialists can play a role in identifying surgical candidates
Individual needs should be matched to technological features