Study finds that inpatient mortality and serious complications are reduced
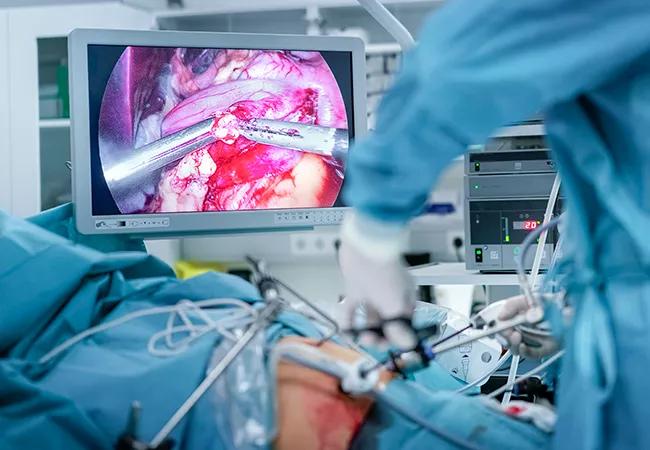
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/05bda2a5-8ff8-42eb-897f-1fc326737aad/22-DDI-2922384-CQD-650x450-1_jpg)
Doctor performing bariatric surgery in hospital
Heart attack is a leading cause of death in the United States, and obesity is a known risk factor for heart disease and mortality. A new study by Cleveland Clinic researchers shows that patients with obesity who underwent bariatric surgery and subsequently suffered a heart attack had lower rates of mortality and severe complications than patients with obesity and heart attack but no history of bariatric surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The study analyzed data from nearly 300,000 patients with obesity who were hospitalized for myocardial infarction (MI). The researchers found that patients with a history of bariatric surgery were almost three times less likely to die while hospitalized than patients who had not had the procedure. Rates of severe complications and hospital lengths of stay following MI also were lower in the bariatric surgery cohort.
“Obesity is a serious disease and treating it with bariatric surgery has very clear benefits,” says study coauthor Roberto Simons-Linares, MD, Director of Bariatric Endoscopy in Cleveland Clinic’s Digestive Disease & Surgery Institute. “You can reduce your risk of having a heart attack, or if you do have a heart attack and end up in the hospital, you reduce your risk of dying or having complications.”
The study’s results were presented at the 2022 Digestive Disease Week annual meeting.
The case-control study utilized data from the 2016 and 2017 National Inpatient Sample, using ICD10-CM codes to identify patients with obesity who were hospitalized with MI, including those with a history of bariatric surgery.
Due to the dataset’s limitations, it did not contain information on how much weight each patient had lost following bariatric surgery or the period of time that had elapsed between bariatric surgery and MI, Dr. Simons-Linares notes.
Primary outcomes were differences in mortality rates and differences in rates of inpatient outcomes and complications between the case group (patients with obesity and MI who had previously undergone bariatric surgery) and the control group (bariatric surgery-naïve patients).
Advertisement
Secondary outcomes were acute kidney injury (AKI), respiratory failure requiring mechanical ventilation, shock, sepsis and hospital length of stay (LOS).
The researchers created multivariate regression models to adjust for confounders and hospital characteristics.
Of 290,450 patients with obesity and MI included in the study, 3,805 had a history of bariatric surgery. This case group had an in-hospital mortality rate of 0.8%, compared with an in-hospital mortality rate of 2.3% among the control group of patients who had not had the procedure (p=0.001).
“Those may look like small numbers, but when we’re talking about the lives of patients, they are significant,” Dr. Simons-Linares says. “The survival rate for patients who had undergone bariatric surgery is almost three times better.”
Bariatric surgery patients also had lower rates of respiratory failure (2.2% compared with 4.2% for no-surgery patients, p=0.01) and AKI (13.7% compared with 21.2%, p<0.01).
They had shorter mean LOS (4.02 days compared with 4.8, p<0.01) and lower mean hospitalization costs ($86,412 in total charges compared with $100,471 for no-surgery patients, p<0.01).
“The message is that bariatric surgery works,” says Dr. Simons-Linares. “Currently, less than 1% of patients who qualify for bariatric surgery actually get the surgery. That means 99% of eligible patients are missing this benefit of living longer.”
In addition to adding to the medical literature on bariatric surgery, Dr. Simons-Linares says the study shows the importance of treating obesity as a disease.
Advertisement
The results should encourage clinicians to intervene sooner when treating patients with obesity who are at risk for heart disease.
“We need to approach obesity not as a cosmetic problem but as a serious chronic and relapsing disease,” he says. “For clinicians with patients whose body mass index is 30 and above, they should immediately try to decrease their patients’ risk by referring them to a specialist who treats obesity.”
While the present study focused on bariatric surgery, other options such as endoscopic interventions and drug therapy also have been shown to be safe and effective for patients with obesity. “It’s not one-size-fits-all,” Dr. Simons-Linares says.
Outcomes from the study and others like it should motivate insurance providers to cover obesity treatments including bariatric surgery, he says. “There are major benefits both in terms of patient care and resource utilization.”
Dr. Simons-Linares notes that bariatric surgery is not a quick fix, but rather one step in a weight-loss process that also includes major lifestyle changes.
“I tell all my patients, ‘These are tools for you to use,’” he says. “We have a multidisciplinary approach, with dieticians, nutritionists, psychologists and surgeons. We all work together to improve outcomes in patients suffering from obesity.”
Dr. Simons-Linares is planning a follow-up study utilizing a smaller database that should reveal more details about patients with obesity and a history of bariatric surgery and the impact of multiple weight-loss interventions on MI risk and outcomes.
Advertisement
“For example, how much weight do you need to lose to get these mortality and morbidity outcome benefits?” he says. “When we get into that more granular data, it can help us tailor those outcomes and perhaps use some of those data points as targets to advise our patients.”
Advertisement
Advertisement
New program looks to innovative approaches for advancing early detection and multicancer prevention
Patients have a significantly higher risk of developing fistulas and experiencing future Crohn’s-like changes
Cleveland Clinic researchers developed an objective tool to assess response following total neoadjuvant therapy.
Patients may benefit from booster appointments, psychological support
Research demonstrates cirrhosis regression in one-third of patients, with higher rates using alternative assessment
Elevated risk persists for more than a year after surgery, plus more insights from the first study to quantify risk specifically for CRC surgery
Large, retrospective study indicates improved outcomes after one and five years of treatment
Multidisciplinary collaboration is fueling breakthroughs in endoscopic and surgical technology