Complex microsurgery may reduce risk of lymphedema
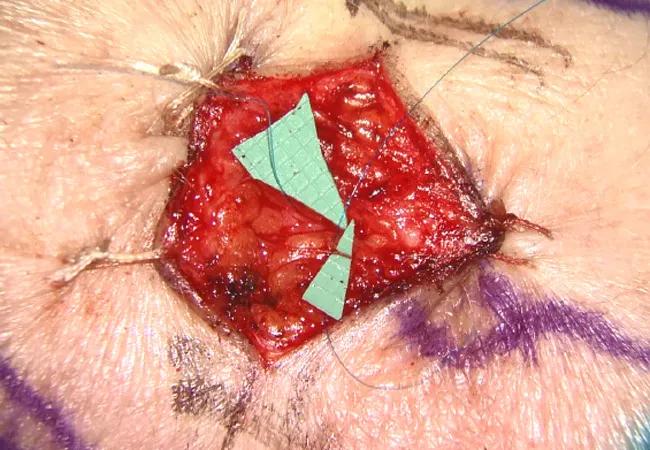
Researchers at Cleveland Clinic are studying whether performing lymphaticovenous bypass (LVB) concurrent with breast cancer surgery will reduce a patient’s risk of developing lymphedema. In this Q&A, plastic surgeon and Director of Cleveland Clinic Microsurgery and Breast Reconstruction Fellowship, Graham Schwarz, MD, discusses the Lymphedema Prevention Study.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Q: Do we know why some individuals develop lymphedema and some do not?
A: Individuals who require more extensive lymph node removal and radiation are among those with the highest risk of lymphedema. When a patient with breast cancer requires an axillary node dissection and has multiple lymph nodes removed, there is a disruption in the connections that allow lymph fluid to drain from the arm to the torso. Scar fibrosis of remaining pathways and obstruction of transected lymphatics occur. Radiation treatment following surgery can further damage the channels. Protein-rich fluid accumulates in the arm producing chronic inflammation, scar and fat deposits and limb enlargement.
Q: Can you tell us about LVB and the current study?
A: The Lymphedema Prevention Surgery study is an ongoing collaboration with Cleveland Clinic’s breast surgery oncology team. We are exploring the use of prophylactic lymphaticovenous bypass surgery coupled with lymphatic mapping techniques to reduce the incidence of lymphedema in breast cancer patients who are at high risk for developing the condition. Our hypothesis is that when a patient has an axillary lymph node dissection, we can reduce the patient’s risk of developing lymphedema by re-routing disrupted lymphatic channels that drain the arm and avoid injury to remote lymphatic channels uninvolved in the breast cancer resection.
Q: What types of patients are candidates for the study?
A: The procedure is typically performed when we know prior to surgery that a patient will need an axillary lymph node dissection in conjunction with a lumpectomy or mastectomy. We identify these patients based on results from ultrasound, breast MRI or biopsy showing that there is cancer in the lymph nodes.
Advertisement
Q: Could you describe how lymphovenous bypass surgery is performed in conjunction with breast cancer surgery?
A: Prior to surgery, we obtain a baseline arm circumference, bioimpedance measurements and ICG fluorescence lymphangiography with a Near-Infrared Camera, which allows us to visualize how the patient’s lymphatics are functioning.
The breast surgeon performs the mastectomy or lumpectomy and the axillary lymph node dissection. An important component of this technique is the use of reverse lymphatic mapping with a combination of special tracer dyes that allow us to identify the lymphatics that are draining the fluid from the arm. In most instances, there is overlap between the lymph nodes that drain the breast and the lymph nodes that drain the arm. If some of the lymph nodes and lymph vessels that drain the arm can be spared, that is helpful. If they cannot be spared, they can be marked so that we can identify them.
After the cancer surgery is completed, the plastic and reconstructive surgery team will isolate a suitable vein and employ microsurgery techniques to perform lymphaticovenous anastomoses. The goal is to restore a pathway for lymph fluid to be transported to the vein system, thus maintaining continuity of upper extremity lymphatic drainage.
Q: Do you have concerns about how post-surgery radiation might impact the effectiveness of the LVB?
A: This is a key question we are exploring in the study. It is possible that if we do the LVB and then a patient has radiation, it could disrupt the new lymphatic pathways that we created. Our hope is that if we immediately reestablish continuity of the damaged lymphatic pathway, this may mitigate the impact of radiation fibrosis on an already surgically compromised area.
Advertisement
Q: What do you see as the importance of lymphaticovenous bypass in the broader field of breast cancer treatment?
A: Lymphedema is an underappreciated complication of cancer treatment that can be debilitating and have a substantial negative effect on a person’s life. We have the expertise to give patients access to new procedures that may prevent lymphedema by avoiding lymphatic injury and restoring lymphatic continuity using LVB when lymph channels are cut. We also offer LVB as an option to help patients who are currently affected by lymphedema.
Advertisement
Advertisement

Early results show strong clinical benefit rates

The shifting role of cell therapy and steroids in the relapsed/refractory setting

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors

Study shows significantly reduced risk of mortality and disease complications in patients receiving GLP-1 agonists