Insights from the medical intensive care unit during a pandemic
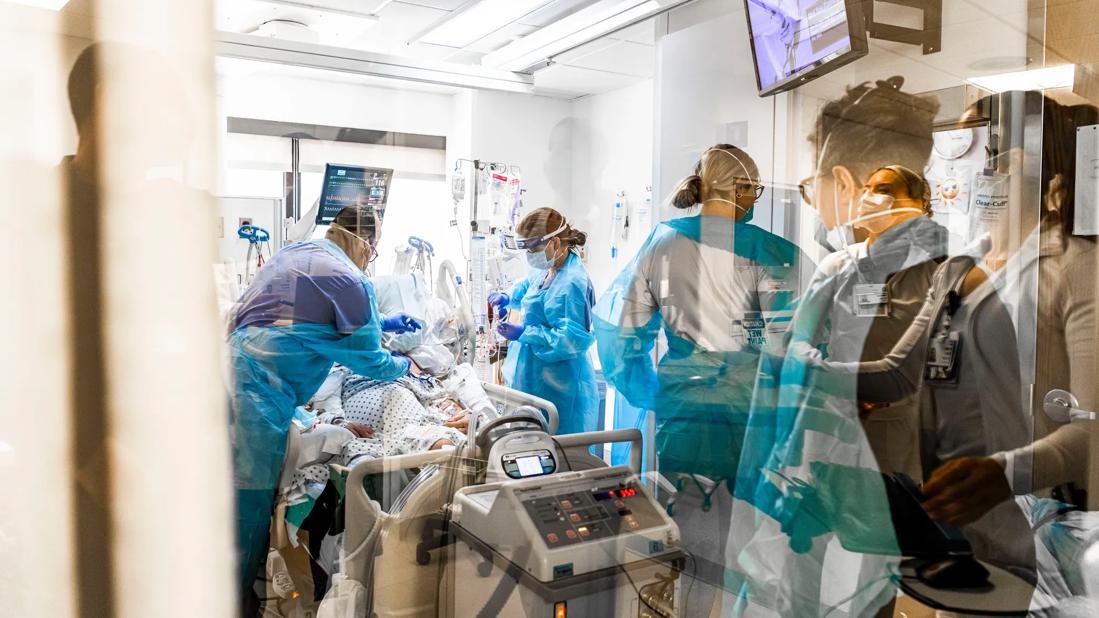
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5e73a3ad-a935-426b-b0a7-ec03e2b04e5b/HRC_2881047_04-28-22_034_MLC-jpg)
650×450-Buddy-System-Covid-Doffing
By Eduardo Mireles-Cabodevila, MD and Mani Latifi, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
We had time to prepare. Not much, by usual standards, but we had three weeks until admitting a patient who tested positive for COVID-19 to our unit. Nearly one week later and our cohort unit behaved as if we had been preparing for years. In a sense, we did. For the last two years, we have been working on building high-functioning teams by fostering an interprofessional and multidisciplinary practice, recognizing our team members’ abilities, roles and responsibilities, building a psychologically safe environment and flattening legacy hierarchies. All of this allowed for our team to rapidly adapt, innovate and be highly functional.
Our team has two cardinal rules that are both equally important: 1) provide our patients with the best care and 2) keep our caregivers safe. This becomes more relevant during the time of a novel disease pandemic with caregiver transmission as high as 11%, according to some published series.1 To date (Apr. 7, 2020), our unit has had around 100 patients with COVID-19 or suspected of having it. Here is a glimpse into how we run this unit.
Our cohort unit, with capacity for up to 43 patients, aims to limit exposure of other patients and focus our team on best practices. The most important practice is proper personal protective equipment (PPE) donning and doffing. As do all other hospitals, we follow our infection prevention recommendations. This is based on our supply, the evidence and the risk.
During the first week of the outbreak, it became paramount that all caregivers understood how to follow proper techniques. Improper use can place caregivers, patients and others at risk. It is not just the PPE, it is also how you use it. We all recognized this was the most important behavior to acquire. We wondered, how do you teach a unit with a pool of around 500 caregivers to don and doff without wasting PPE in the learning process? There are not sufficient videos, classes or pamphlets to make everyone proficient. Besides our own team, we also had others (consultants, radiology techs, environmental services, etc.) come into our unit, and they were also at risk.
Advertisement
In response, we created the buddy system. Every caregiver who enters or exits the room is observed donning or doffing by a buddy outside the room. This behavior changed the unit and made us safer. We heard comments from many caregivers, stating they feel safer in the cohort area than anywhere else in the hospital.
Our team is also committed to fostering innovation guided by our principles. It became clear that we needed to preserve PPE as much as possible. Following our goal of staying safe and providing patients with the best care, we recognized we needed to limit all unnecessary traffic into patient rooms. We determined that entering the infected patient’s room should only happen when it was essential. We decided to bundle care, performing as many tasks as possible during each entry. We also limited room entry to those who absolutely needed to be in there.
Our nursing and respiratory therapy teams worked on the placement of medication administration pumps and ventilator screens with controls outside of patient rooms (this decreased our PPE use by about 50-60%). Not only that, but we were able to maintain more efficient titration of medications and ventilator settings as the patient required. This decreased sedative use and hastened weaning from the ventilator. We had only one member perform a dedicated and comprehensive physical exam each day, which is then shared with all other necessary care/consulting teams to further limit entrance.
Finally, instead of rounding as a large group as we are used to doing in the medical ICU, we developed a system of remote rounding with only the intensive care attending physicians at the bedside. All other team members participate electronically through a tablet device mounted on the portable computer stand. Like those mentioned here, there are many small but meaningful interventions created by our team members that build an environment for us to deliver the best and safest possible care.
Advertisement
Finally, our culture at Cleveland Clinic is to embrace change. As a constant feature of the organization, the team recognizes change is unavoidable. This framework allows rapid cycle changes in times of crisis. In the last months, we have learned and unlearned a lot of new behaviors. There are not enough classes and competencies performed that could keep up with the pace of change in a pandemic. Our education platforms had to adapt to deal with this. However, even with a robust educational platform and curriculum available for all caregivers, permeation and retention of knowledge is a challenge. In these trying times, we believe it is the team in the unit that collectively transmits the behaviors that become the culture.
About the authors
Dr. Mireles-Cabodevila is the Director of the Medical Intensive Care Unit at Cleveland Clinic.
Dr. Latifi is a Pulmonary and Critical Care Medicine Physician at Cleveland Clinic Medical Intensive Care Unit
Reference
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19