What clinicians need to know about cutaneous manifestations of COVID-19
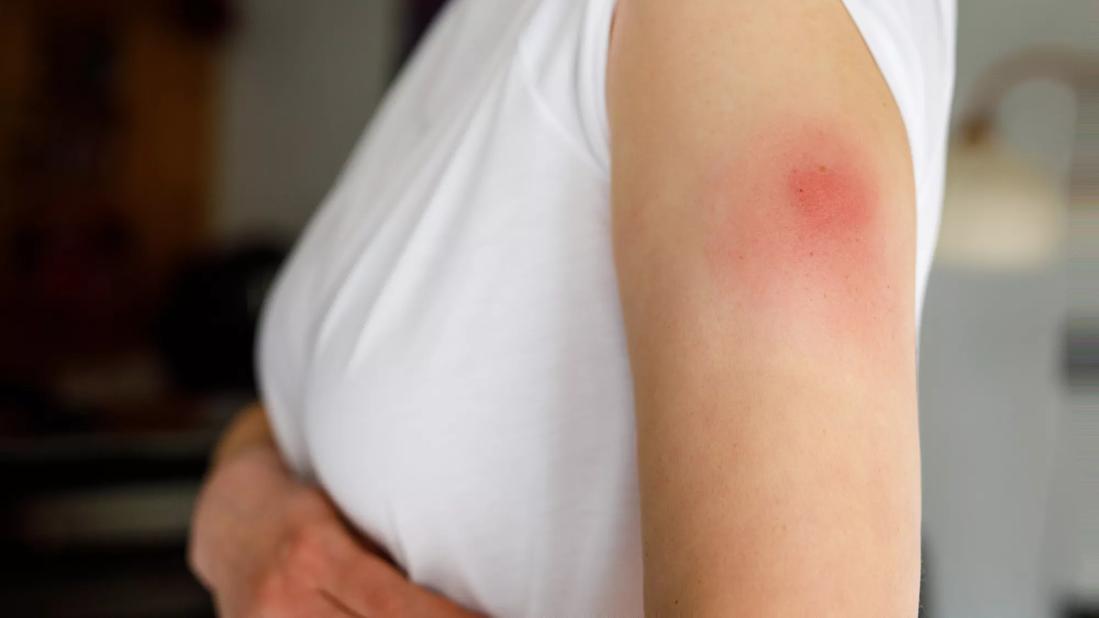
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/03a0840d-6fbf-4204-ac7a-a5b38f95587b/covid-arm-1309903762)
Arm rash
Along with fever, dry cough and shortness of breath, COVID-19 has been associated with a wide range of symptoms, but the disease’s cutaneous manifestations have not been widely discussed. Now, early reports from Italy and Thailand indicate that skin rash might be another symptom of COVID-19.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“I’m not sure it’s widely known outside the dermatology community, and we’re just starting to see reports even in the dermatology literature,” says Sarah Young, MD, a medical dermatologist at Cleveland Clinic. Clinicians should know that, while it appears that some patients may indeed experience skin symptoms, there is not yet any known specific rash associated with COVID-19 patients or associated with severe disease.
An early report from dermatologists working with COVID-19 patients in Italy found that, in a group of 88 confirmed positive patients, 20% developed skin symptoms, with a little under half developing a rash at the onset of disease, and a little more than half developing it after hospitalization. Of the affected patients, the most common manifestation was erythematous rash, or a patchy red rash. A few developed urticaria, or hives, and one developed chickenpox-like blisters. The trunk was the most commonly involved site.
In another report, doctors in Thailand described a COVID-19 patient initially misdiagnosed with dengue fever, who presented with petechiae, or broken blood vessels, a rash common in dengue.
More recently, Dr. Young notes, there have been reports of COVID-19 patients developing livedo reticularis, or mottling, which could indicate occlusion of blood vessels near the skin.
“It’s so varied, what we’re seeing, and the rashes being reported can be seen in a variety of other diseases, so there’s not one specific rash reported thus far that says, ‘Yes, this patient has COVID-19,’” says Dr. Young.
Advertisement
A big question dermatologists hope to answer is whether the presence of a rash, or the type of rash that develops, is a clue to the course or severity of the disease. “Does having a rash affect prognosis in any way?” Dr. Young asks. “We don’t know that yet.”
More information is coming. The American Academy of Dermatology (AAD) has established a COVID-19 registry for physicians and health care professionals treating COVID-19 patients who develop dermatologic manifestations, or patients with an existing dermatologic condition who develop COVID-19. “I do think reports are starting to come out, so as we are building these types of registries, I think we will start to see more information about skin symptoms,” Dr. Young says.
The AAD has also established a dedicated COVID-19 dermatology platform with free access to information and resources for healthcare providers.
Until more is known, clinicians should be aware that a rash may be a symptom of COVID-19, and know that skin symptoms, in addition to other clinical clues, may be used to support a diagnosis or as a factor in deciding whether or not to recommend a patient be tested for the disease. Physicians should also be aware of the potential for misdiagnosis, especially in light of the variety of rashes that have been reported.
Healthcare providers should treat the rash symptoms as needed to keep the patient comfortable, and expect that any skin conditions should resolve with the resolution of the disease, Young says.
Cleveland Clinic’s dermatology team is available, she adds. “Our medical teams are just doing such an excellent job caring for these patients and caring for their other vital organs, so if clinicians see skin manifestations, I hope they reach out,” she says. “We’re here, we’re interested, and we hope to provide valuable input that may lead to improved detection, prognosis and treatment of affected patients.”
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19