Study demonstrates benefits in health status, depression and more
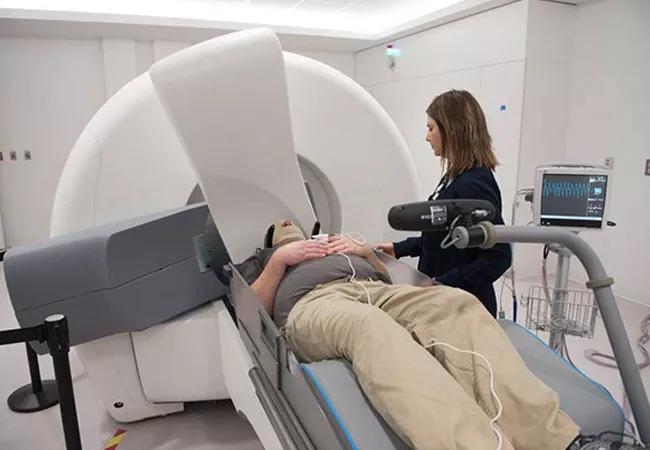
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/28da3c69-0a90-4689-99ad-9b3362d77f8e/17-NEU-834-Chao-650x450_jpg)
17-NEU-834-Chao-650×450
Treating trigeminal neuralgia with stereotactic radiosurgery leads to improved outcomes in multiple quality-of-life measures, according to a prospective Cleveland Clinic study recently published online by the International Journal of Radiation Oncology • Biology • Physics.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“For a condition like trigeminal neuralgia that has such a tremendous impact on quality of life, it’s important to determine whether treatment not only lessens pain but improves well-being,” says principal investigator Samuel T. Chao, MD, a radiation oncologist with Cleveland Clinic’s Rosa Ella Burkhardt Brain Tumor and Neuro-Oncology Center. “Our research demonstrates that stereotactic radiosurgery does so for this disease.”
Stereotactic radiosurgery (using Gamma Knife®) is one of several treatment options for patients with trigeminal neuralgia, a condition that can cause facial pain so severe that the disorder is sometimes called the “suicide disease.” Because the pain typically arises without warning, patients may become shut-ins out of fear of being out in public if an attack occurs.
Medications are not always effective, and those that do work well may be poorly tolerated, especially in older patients, who make up a large share of the affected population.
Stereotactic radiosurgery offers a minimally invasive treatment option with rates of pain control of up to 80 percent — especially at doses above 83 Gy — albeit with a risk of resulting facial numbness.
Despite these encouraging pain control rates, data are scarce on radiosurgery’s impact on quality-of-life measures in trigeminal neuralgia. Most studies have had the limitations of being conducted retrospectively, describing physician-reported (rather than patient-reported) outcomes and using categorical pain response scales, which don’t allow quantitative analysis of treatment effects.
Advertisement
The new study prospectively collected quality-of-life data on 50 patients before and after undergoing stereotactic radiosurgery for trigeminal neuralgia at Cleveland Clinic from 2008 to 2014. Measures were patient-reported using the following questionnaires:
All quality-of-life outcomes were collected from patients at routine appointments and entered into a prospectively maintained database at Cleveland Clinic.
According to Dr. Chao and his co-authors, the EQ-5D instrument has not been validated in patients with trigeminal neuralgia but provides multiple advantages for this kind of research. “It’s a global assessment of patient health status that can be applied to different diseases, it is easily completed by patients without physician input, and it provides quantitative quality-of-life measurement, allowing for comparative studies,” explains Cleveland Clinic fellow Rupesh Kotecha, MD, who served as the study’s first author.
Patients’ median age at time of radiosurgery was 65 years (range, 31-85), the median radiation dose was 83 Gy (range, 80-86) and median follow-up was 13 months (range, 3-89). Radiosurgery was the primary treatment for 43 patients (86 percent), with the others having undergone at least one prior surgical procedure.
Advertisement
On the study’s primary clinical outcomes (assessed using Barrow Neurological Institute scales), patients achieved high rates of 12-month freedom from pain failure (92 percent) and 12-month freedom from facial numbness (89 percent).
Meanwhile, patients reported significant benefits in multiple health status measures within approximately five to nine months after stereotactic radiosurgery. Specific results included the following changes from pretreatment status to last follow-up:
On multivariate analysis, higher prescription dose (86 Gy vs. <82 Gy) was the sole variable associated with improvement on the EQ-5D.
Given the small sample size, it was not possible to draw conclusions about selected patient populations, such as those with trigeminal neuralgia that is atypical or multiple sclerosis-related.
The study authors encourage other institutions to routinely collect and analyze quality-of-life data on their patients. As an example, Dr. Chao cites microvascular decompression as another treatment option for trigeminal neuralgia — one that may offer more permanent pain relief but requires a few days of hospitalization.
Advertisement
“Does microvascular decompression make sense for the elderly?” he asks. “What are the costs compared with improved quality-of-life parameters for various age groups? These kinds of questions are critical for every institution to examine on the treatments they provide.”
Advertisement
Advertisement
How to use? Consider starting during the acute attack and seek patient preferences for chronic use
Quantitative imaging adds diagnostic value beyond 3T MRI in nearly half of patients
Expert shares insight on intrathecal baclofen pumps to treat spasticity
Opportunities and impacts of a growing surgical approach
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges