Scientific evidence for and clinical experience of using JAK inhibitors in the treatment of COVID-19
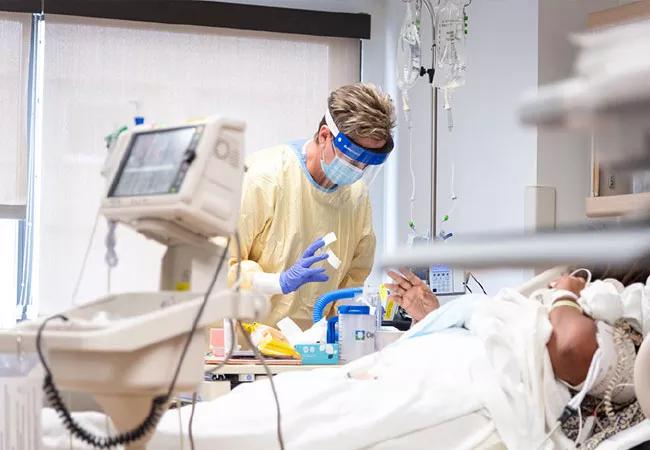
COVID-19-related mortality rates have declined dramatically in the U.S. since the beginning of the pandemic, especially in patients hospitalized in intensive care units. This may be in part because of more aggressive management of the hyperinflammatory phase of advanced COVID-19 with dexamethasone. More recently, the use of the Janus kinase-signal transducer (JAK) inhibitor baricitnib have emerged as a potential alternative strategy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Rheumatologists Leonard Calabrese, DO, and Cassandra Calabrese, DO, consider the evidence for and clinical experience with JAK inhibitors in COVID-19 in recent articles published in the Cleveland Clinic Journal of Medicine’s Curbside Consults.
The Janus kinase-signal transducer and activator of transcription (JAK-STAT) signaling pathway mediates biologic activity for a number of inflammatory cytokines and mediators. Rheumatologists use JAK inhibitors across a broad spectrum of immune-mediated inflammatory diseases, such as rheumatoid arthritis.
According to the authors, “JAK-STAT activation contributes to a host of critical events, such as hematopoiesis, inflammation, the development of the immune system, and deployment of a variety of effector pathways. Cytokines are one of the major products of cells of innate and adaptive immunity, and more than 60 factors bind to receptors termed type I and type II cytokine receptors and mediate their downstream effects through the JAK-STAT pathway of signal transduction.”
These cytokines can be the source of uncontrolled inflammation in the setting of advanced COVID-19. Because data supporting the identification of a single cytokine to target has been problematic, a broad-based inhibitory approach is appealing.
Several small trials and case reports have been published on the use of baricitnib, ruxolitinib and tofacitinib in COVID-19. Results from these reports, overall, indicate significant improvement in clinical and laboratory parameters and no major safety issues. However, “vigilance for infectious complications is critical in the use of JAK inhibitors in this setting,” the authors state.
Advertisement
Additionally, JAK inhibitors increase the risk of venous thromboembolism. Thus, physicians should also watch for hypercoagulable complications.
Both dexamethasone and JAK inhibitors are poised to suppress the hyperinflammatory phase of advanced COVID-19, the authors state. “Dexamethasone, a long-acting glucocorticoid, binds to glucocorticoid receptors, which are ligand-dependent transcription factors. Liganded glucocorticoid receptors in turn bind to glucocorticoid-responsive elements in target genes, thus influencing a host of cellular processes,” which can be broadly immunosuppressive.
JAK inhibitors work by modulating the biologic activity of a broad array of inflammatory cytokines. However, given the increased risk of infectious and cardiovascular complications, careful laboratory monitoring is vital.
To read the article as originally published in the Cleveland Clinic Journal of Medicine’s Curbside Consults, please visit https://www.ccjm.org/content/early/2021/02/24/ccjm.87a.ccc060?cct=2334#ref-3.
Advertisement
Advertisement

Patients report improved sense of smell and taste

Clinicians who are accustomed to uncertainty can do well by patients

Unique skin changes can occur after infection or vaccine

Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition

As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients

Early results suggest positive outcomes from COVID-19 PrEP treatment

Could the virus have caused the condition or triggered previously undiagnosed disease?

Five categories of cutaneous abnormalities are associated with COVID-19