Treatment advancements tip the scales for surgery
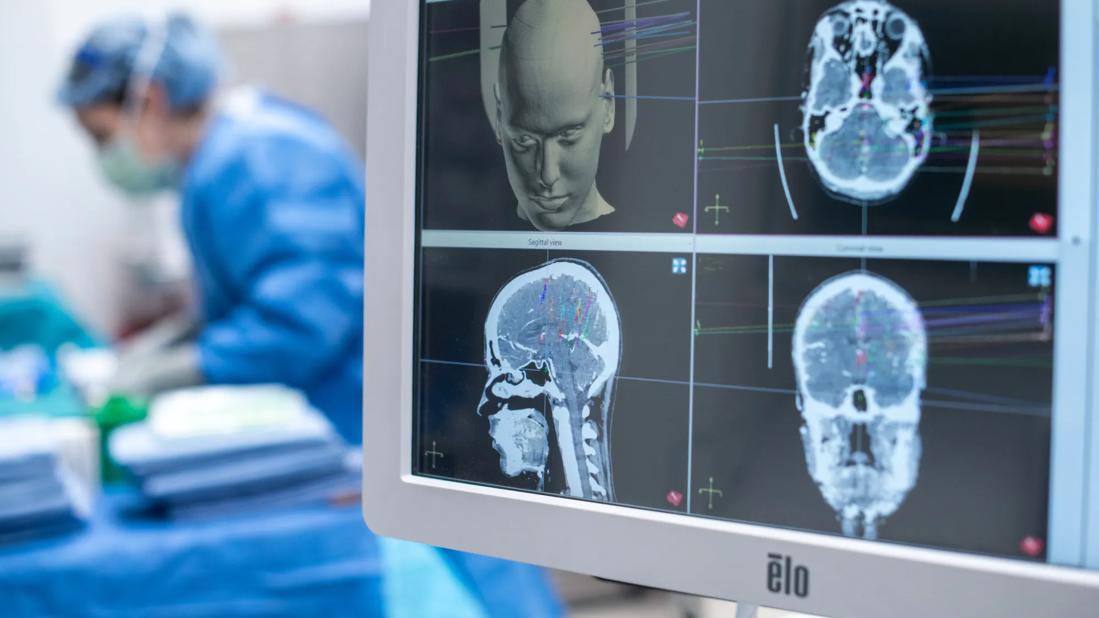
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/86a711c5-d215-4d6a-a85c-31c23fdfa850/NEU_2865231_04-21-22_008_AMO-jpg)
Epilepsy surgery
Times have changed, and so has brain surgery for epilepsy. No longer the treatment of last resort, epilepsy surgery today is safer, more effective, and often less invasive. Unfortunately, many people who would qualify for surgery never get a surgical evaluation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Approximately 30% of the 3.4 million people with epilepsy nationwide have intractable or drug-resistant epilepsy. These individuals have tried two or more appropriately selected and managed anti-epileptic drugs (AEDs) but failed to achieve seizure control.
“That’s a large population of patients who could benefit from a surgical evaluation,” says Camilo Garcia, MD, a board-certified epileptologist with the Cleveland Clinic Florida Epilepsy Center. “But only a fraction of patients are referred for a comprehensive evaluation, and often after 20 or more years of uncontrolled seizures.”
Decades with uncontrolled seizures contributes to poor quality of life resulting from psychological, social, educational, and vocational impacts. There is also a higher chance for seizure-related deaths, including drowning, motor vehicle accidents, and fatal status epilepticus, as well as sudden unexpected death in epilepsy (SUDEP).
“Patients and their physicians need to know that avoiding surgery is not the safest course of action,” asserts Dr. Garcia. “People are less likely to achieve postoperative seizure freedom the longer they have drug-resistant epilepsy before surgery.”
At Cleveland Clinic, about 60% of patients achieve long-term seizure freedom following epilepsy surgery. Data also show that many patients who do not achieve complete seizure freedom still report clinically meaningful quality-of-life gains.
“New imaging techniques and advanced surgical procedures have improved clinical outcomes and made surgery safer,” says Dr. Garcia. “The risk of complications and side effects of neurosurgical procedures is lower than ever.”
Advertisement
He also points to the volume-outcome relationshipin epilepsy surgery that demonstrates lower rates of adverse events at high-volume centers like those at Cleveland Clinic in Ohio and Florida, both level 4 epilepsy centers accredited by the National Association of Epilepsy Centers.
While these data should be reassuring to patients and their physicians, they are often not enough to overcome patient hesitancy. “Patients want to know how surgery will likely affect them personally, including the chance of achieving seizure freedom and their individual risk for complications,” explains Dr. Garcia.
Addressing this unmet need led Cleveland Clinic researchers, in conjunction with an international collaboration of major epilepsy centers, to develop statistical tools to provide objective, individualized prediction of postoperative seizure outcomes.
The first easy-to-use nomogram, introduced in 2015, provides a patient’s individualized probability of achieving seizure freedom after epilepsy surgery. More recently, a set of nomograms were specifically designed to better inform patients considering resection for temporal lobe epilepsy, the most common form of focal epilepsy, about their individualized risk for postoperative declines in verbal memory, naming and mood. These risk calculators are used across the Cleveland Clinic enterprise and are openly available for all clinicians to use.
One of the biggest advancements in epilepsy surgery is the ability to identify more precisely where a seizure originates through brain mapping. Data gained from stereoelectroencephalography (SEEG), a minimally invasive surgical procedure, helps determine who is a surgical candidate and which type of procedure would work best.
Advertisement
“At Cleveland Clinic Florida, we use a stereotactic robot to place the electrodes in the brain with great accuracy,” says Dr. Garcia. “Our Epilepsy Monitoring Unit will then capture data over the course of a week to locate the source of the seizure before the electrodes are removed.”
According to Dr. Garcia, most surgical evaluations at Cleveland Clinic Florida now include SEEG, and the majority of these patients go on to have surgery.
Resection is the best treatment for drug-resistant focal epilepsy, when seizures originate from one specific area of the brain. If the seizures come from multiple areas or near the eloquent cortex, other treatment options are available.
Laser interstitial thermal therapy (LITT), is a minimally invasive laser ablation procedure in which targeted tissue is heated and destroyed. Neuromodulation options include responsive neurostimulation (RNS), similar to a heart pacemaker, deep brain stimulation (DBS), and vagus nerve stimulation (VNS).
To ensure patients receive the most appropriate and effective care, each surgical candidate at Cleveland Clinic is reviewed during a Patient Management Conference by a multidisciplinary team of specialists in radiology, nuclear medicine, neurosurgery and epileptology from across the Cleveland Clinic enterprise, including Florida and the main campus in Ohio.
“Epilepsy surgery has advanced significantly in the past two decades, and we can provide much more personalized care,” says Dr. Garcia. “There is no reason for patients to suffer years with uncontrolled seizures.”
Advertisement
Advertisement
Evidence shows early evaluation improves survival and quality of life – yet many eligible patients are referred too late
2026 ADA Standards of Care promote holistic, multisystem management
Cleveland Clinic nephrologist in Florida addresses changes in clinical practice
Surveillance platform supports community clinicians and public health monitoring
Benefits include improved clinical outcomes and lower healthcare costs
Pulmonary endarterectomy plays central role in era of multimodal therapy
Evidence supports safety and efficacy of surgery in patients aged 80 years and older
One in four experience reduced anxiety