The one-stop THRIVE clinic addresses renal, psychosocial, educational and other challenges alongside cardiac surveillance
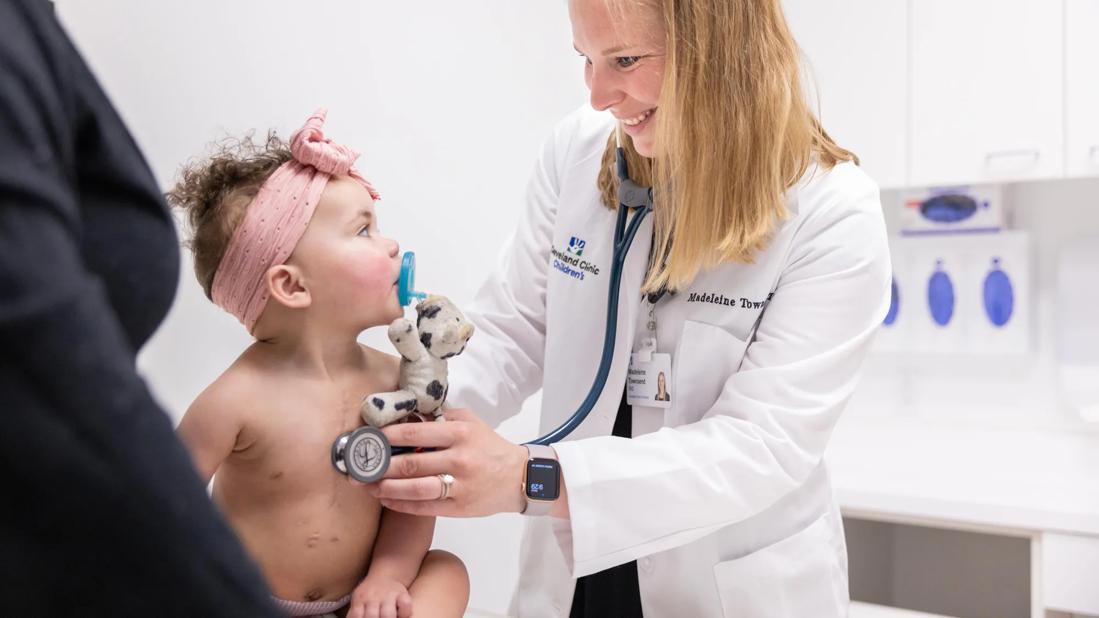
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/799a9eba-ac29-44d7-ba23-6e7342cc94ac/CCC_3982358_06-08-23_1223_AMO-jpg)
Dr. Townsend examining a toddler after heart transplant
Survival and long-term graft success are no longer the only priorities in pediatric heart transplant care. As more children live longer after transplant, clinicians are increasingly focused on the medical, psychosocial and developmental issues that shape long-term well-being.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“From a cardiac perspective, we’re doing a good job,” says Madeleine Townsend, MD, a pediatric heart failure and transplantation cardiologist at Cleveland Clinic. “We know how to monitor patients with heart transplants. We’ve increased graft survival. We’ve improved immunosuppression. But sometimes, we’ve overlooked the other parts of living with a heart transplant.”
Mental health struggles are common in these patients, she notes. So is renal dysfunction, often triggered by long-term use of immunosuppression medications. School performance can cause concern. Social and financial stressors can arise.
To address these needs more systematically, Cleveland Clinic Children’s launched the THRIVE (Transplant, Health, Resiliency, Independence, Vitality, Empowerment) program in 2025. The multidisciplinary clinic for pediatric heart transplant recipients focuses on preventing or identifying post-transplant complications early, improving quality of life for patients and their families, and supporting health into adulthood.
Held monthly at Cleveland Clinic Children’s, the THRIVE clinic provides patients with an annual evaluation beginning one year after heart transplant.
Visits begin with blood draws, including routine transplant, cardiometabolic and nephrology labs, followed by echocardiography and ECG. Patients and families then remain in a private exam room while specialists rotate through for individual consultations, including:
Advertisement
Most visits are completed within four hours, and families receive test results and care recommendations before leaving.
Traditionally, follow-up for pediatric heart transplant has been more reactive, says THRIVE program coordinator Colleen Nasman, RN, BSN, a heart transplant nurse at Cleveland Clinic Children’s for nearly 30 years.
“We used to focus on graft success and adherence to immunosuppressive medications,” she says. “If we’d notice another concern, we’d refer patients to nephrology or psychology or other specialties for a separate visit. Now the THRIVE program combines this care into one visit. It’s much more proactive and holistic.”
A patient’s well-being after heart transplant extends well beyond cardiac status, she notes.
“Some of our kids on certain forms of immunosuppression experience side effects like unwanted facial hair and changes in their gum tissue,” Nasman says. “Sometimes they feel self-conscious about looking different, having a scar on their chest or needing to leave class to take their medication.”
These concerns may not surface during a conventional cardiology follow-up, but the THRIVE model is designed to bring them to light.
“Some experiences are more universal than patients and families realize, and we can offer help,” Dr. Townsend says. “Heart transplant comes with financial and emotional costs, not just for patients, but for parents and siblings as well.”
According to Dr. Townsend, the program’s formal structure distinguishes it from less coordinated approaches used elsewhere. By aligning testing and specialty visits on a single day, the clinic reduces the burden of fragmented follow-up for families while identifying noncardiac complications early.
Advertisement
In one annual visit, the team can address issues such as:
In its first year, the THRIVE program has been well received by families and has improved follow-up engagement, according to the team. Staff are also tracking clinical and operational metrics, including new diagnoses of chronic kidney disease and hypertension, as well as referrals to endocrinology, sleep medicine and other specialties.
The team has refined clinic operations over time. For example, door signs now indicate which specialist will enter next, and nursing and administrative staff have further streamlined provider coordination and scheduling.
For transplant programs considering a similar model, Nasman’s message is clear: “This model is doable. Patients and families have seen the value in it. Some of our long-term patients weren’t always returning for follow-up appointments as advised. Now that we’ve merged their annual follow-ups into one visit on one day, adherence is better.”
Better follow-up should translate into better outcomes, adds Dr. Townsend.
“In chronic childhood illness, the more we can be proactive about patient care and focus on overall well-being, the more we can improve outcomes long-term,” she says.
Advertisement
“These patients are so complex,” Nasman says. “It’s not just cardiac survival we need to think about. A graft may survive for decades, but if a patient is repeatedly hospitalized with renal failure or chronic kidney disease that was not addressed early, quality of life suffers. That patient is not thriving.”
Children who are thriving after heart transplant are often easy to recognize, Dr. Townsend says. They are in school, participating in sports or the arts, and spending less time in the hospital.
“When a child is thriving, you can’t tell they had a heart transplant,” she says. “The child and family know they need to take medication and attend follow-up appointments, but it’s not a struggle. It’s just a natural part of life. Seeing these kids do well is the best part of my job.”
Advertisement
Advertisement
Largest study to date confirms mortality rates similar to DBD transplant and reveals risk factors
More than 30% of patients die when early dialysis is needed after surgery
Highlights and insights from recent Cleveland Clinic experience
Results from a large registry study provide an updated picture of recurrent rejection
Findings from more than 7,500 donor-recipient pairs
Study validates a noninvasive alternative to invasive coronary angiography
AHA statement provides the latest comprehensive, evidence-based information
A new CME opportunity in Chicago, May 15-16