Locations:
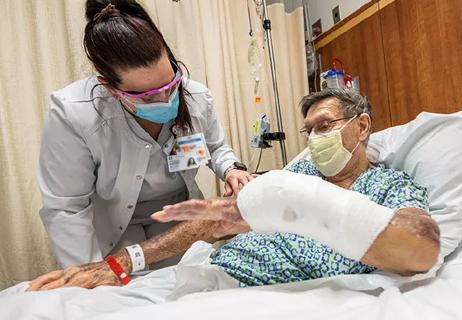
Advice for those pursuing a WOC nursing career

Educational program helps reduce skin injuries
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Advertisement