Improving patients’ quality of life through targeted drug delivery
Over time, chemotherapy and radiation therapy can lead to severe neuropathic pain for cancer patients. Other sources of cancer pain come from bone metastases, nerve and spinal cord compression, as well as pressure on the organs. Cleveland Clinic Pain Management specialists work in collaboration with oncology physicians and palliative care specialists to help cancer patients control pain when other remedies fail.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Sometimes the pain becomes unbearable for patients and medications cannot provide very good pain control,” says Sherif Costandi, MD of Cleveland Clinic’s Department of Pain Management. “This is when we can help, by pinpointing the patient’s source of pain and providing targeted drug delivery to improve pain control.”
Dr. Costandi relays a recent patient success story. In August 2016, a 60-year-old lung cancer patient’s excruciating pain was abated with the implant of a special pump to deliver medication in his spine. The patient’s cancer had metastasized to his bones and brain and he had been on several opioid medications for a few years. Dr. Costandi noted that between the poor pain control and the disabling side effects of his escalating opioids, the patient reported that he no longer wanted to live. The intrathecal pump was implanted to deliver local anesthetics and opioids with variable concentrations, at a much smaller dose than when it is taken by other routes.
“The patient was happy to find out that there were other viable and more effective therapeutic options,” says Dr. Costandi. “It was a remarkable improvement for this patient, showing how effective the intrathecal pump can be for long-term cancer patients.”
The pump relieves pain and improves function without the often debilitating side effects of opioids, which over the long term, can include severe constipation and feelings of drowsiness and dizziness. At this patient’s six-month follow-up appointment in early 2017 to check on his pump and medication dosage, the patient reported that his cancer pain was minimal and that his quality of life had greatly improved.
Advertisement
During a recent flare up of this patient’s pain, Dr. Costandi says the patient still opted not to take additional oral opioid medication for the breakthrough pain. Instead, the patient requested that he receive the patient therapy manager option, which enables patients to self-administer pain medication through the intrathecal pump. This allowed the patient to increase, within limits, the amount of the drug he needed at specific moments of pain. It turned out to be a successful option for this patient.
Dr. Costandi says the intrathecal drug pump implant works well for patients who fail to respond to oral opioids and may benefit from an alternate therapy as well as those who experience pain relief from opioids but are limited by severe side effects. Intrathecal pump implants optimize pain relief for patients with a life expectancy of more than three months.
“This and other interventional therapies can greatly improve a cancer patient’s quality of life and help them to wean off of opioids, especially if they are experiencing severe side effects,” he says.
In recent years, another therapy that is becoming more established as an alternative or additional technique to help relieve cancer pain is the OsteoCool system, notes Dr. Costandi. This technique uses bipolar water-cooled radiofrequency ablation to treat spinal pain that is secondary to metastatic vertebral tumors. This outpatient procedure involves a probe being inserted at the vertebral level. It is best for patients who have one to three lesions that have been localized to the spine, are not candidates for radiotherapy and do not have a neurological deficit – or spinal cord compression.
Advertisement
“We have seen great outcomes with OsteoCool,” says Dr. Costandi. “It helps patients to improve quality of life with minimal recovery time and lessens overall opioid use and its associated fatigue.”
Dorsal root ganglion (DRG) stimulation is a neuromodulation therapy, similar to traditional spinal cord stimulation (SCS) that is being applied more and more to relieve cancer pain. Rather than placing electrodes over the posterior aspect of the spinal cord as in SCS, leads are implanted on the dorsal root ganglion, a cluster of neurons in the posterior root of spinal nerves, which modulate all bodily sensations. DRG stimulation is a particularly effective therapeutic approach for patients with chronic intractable neuropathic pain.
DRG stimulation offers a highly-directed stimulation field, which can focus stimulation to the painful area. The FDA has approved DRG stimulation for lower extremity CRPS, which could include neuropathic pain conditions and chronic pain following surgeries (like thoracotomy) commonly performed in cancer patients.
“When it comes to providing cancer care, it is a true multidisciplinary effort to help our patients,” says Dr. Costandi as he works in collaboration with oncologists and palliative care specialists. “In Pain Management, we are taking pain relief techniques that have been developed over time and using them to help in the fight against cancer pain. In the setting of malignancy, these therapies give us hope.”
Laura Shoemaker, DO, of Cleveland Clinic’s Palliative Medicine team agrees, “Our colleagues in Pain Management provide a range of medical and procedural expertise so we can offer approaches that deliver the greatest benefit for the relief of pain, while subjecting patients to the least amount of burdensome side effects.” She adds: “Collaborative work with Pain Management is a patient-centered approach that optimizes quality of life for our patients.”
Advertisement
Advertisement

Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies

Study participants also reported better sleep quality and reduced use of pain medications

Two-hour training helps patients expand skills that return a sense of control
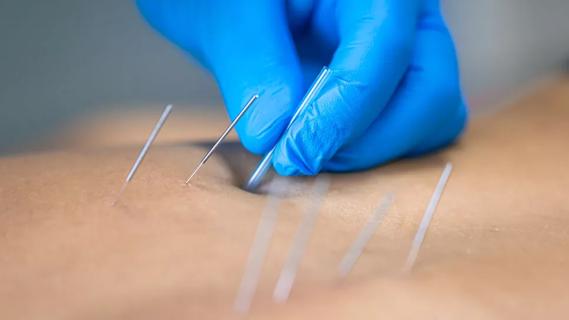
Program enhances cooperation between traditional and non-pharmacologic care

National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
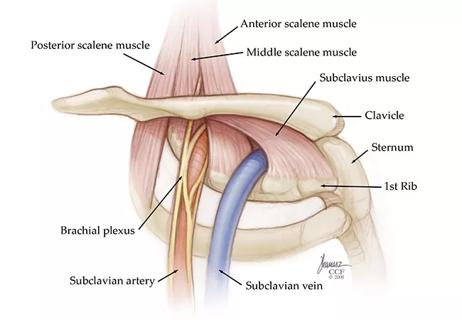
Pain specialists can play a role in identifying surgical candidates
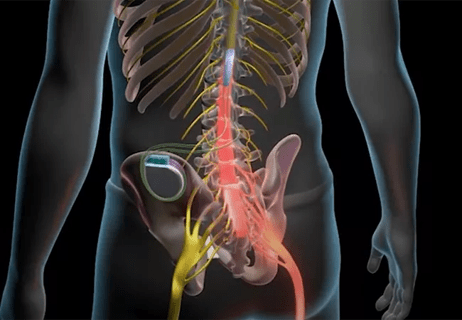
Individual needs should be matched to technological features
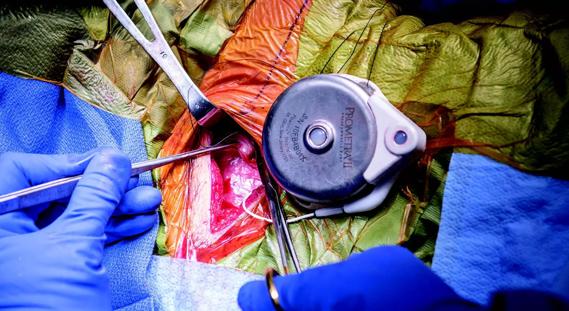
New technologies and tools offer hope for fuller understanding