Q&A with a pediatric neurosurgeon advancing the technique
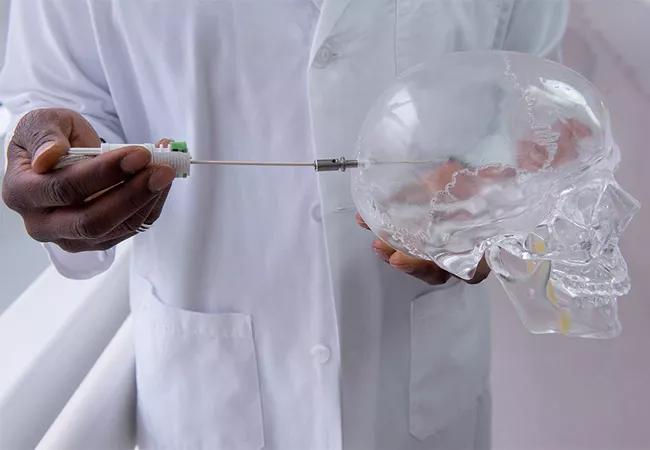
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ae154f8f-831b-4f41-acc7-274803c5497f/17-NEU-793-Onwuzulike-650x450_jpg)
17-NEU-793-Onwuzulike-650×450
When pediatric neurosurgeon Kaine Onwuzulike, MD, PhD, joined the staff of Cleveland Clinic Children’s in mid-2016, he brought along expertise in pediatric applications of MRI-guided laser interstitial thermal therapy (LITT) for treatment of brain tumors and other intracranial neoplasms. This makes Cleveland Clinic Children’s one of a small number of U.S. medical centers offering this minimally invasive modality to pediatric patients.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
LITT involves insertion of a high-power laser probe (along with a cooling catheter) through a drill hole in the skull to deliver targeted thermal therapy for ablative destruction of tumor tissue without harming surrounding tissue. Dr. Onwuzulike holds a skull model illustrating the concept in the photos above and below. LITT can be done as a frame-based or frameless stereotactic technique, depending on patient and tumor characteristics. It is performed in an MRI suite to enable guidance from a series of MR images throughout the procedure.
While use of LITT is well-described in adults, descriptions in the pediatric population are scarce. We recently caught up with Dr. Onwuzulike to ask him to outline a few essentials on current use of LITT in pediatric patients, as captured in the Q&A below.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ba61f7a9-12db-4699-a084-4c8570f7af7f/17-NEU-793-Onwuzulike-inset_jpg)
Q: Where does LITT fit within the general treatment approach to pediatric brain tumors?
Most pediatric brain tumors are typically treated via open surgical resection. When this is impractical or not feasible — such as in cases where the lesion is not surgically accessible — LITT can allow me to still treat the tumor. It also provides an additional treatment option in cases where surgery and/or adjunctive therapy, such as chemotherapy or radiation therapy, have failed. Moreover, LITT can be used in combination with these other therapies.
Q: Where might LITT fall in a stepped-care approach? Is it a last resort?
We are using LITT more and more in our treatment paradigm for pediatric tumors. It is typically used if surgery is not feasible, usually due to deep or eloquent tumor location or because of a child’s medical inability to undergo an operation.
Advertisement
It is not restricted to use as a last resort. We assess all tumors in terms of their surgical accessibility, response to adjuvant therapy such as radiation or chemotherapy, and whether they are amenable to thermal ablation. As such, we consider LITT as one of several potential first-line options within our overall treatment paradigm.
Q: What advantages does LITT promise over existing therapies for children?
A main advantage is its low-profile system and minimally invasive nature compared with traditional open surgery. In contrast to a conventional surgical intervention, LITT does not require a wide craniotomy; in fact, we perform LITT via a minute entry into the skull that’s less than 2 cm in diameter. In general, the minimally invasive nature of this modality confers a host of related advantages over conventional surgery, including less discomfort, decreased morbidity, shorter hospital stay, quicker recovery, fewer complications and better cosmetic results.
There are also advantages that are especially pertinent for pediatric patients, such as the fact that it does not require ionizing radiation and has no reported adverse effects other than the expected edema. Lastly, LITT is repeatable as often as indicated and can be used alone or with other treatment modalities, offering a lot of flexibility.
Q: Are there special considerations when applying LITT to pediatric patients?
LITT has no formal age limitations, and it has been used successfully in children as young as 6 months of age. Yet LITT does require that pediatric patients have sufficient skeletal maturity to allow the skull to be held in a semi-fixed system during therapy delivery.
Advertisement
LITT has been used effectively in several distinct tumor types of varying vascularity and volume, including large supratentorial and infratentorial lesions.
Q: What characteristics make a pediatric patient an appropriate candidate for LITT?
The most common indication for LITT is a surgically inaccessible lesion — cases where lesion location poses too high a risk from conventional surgery. Another common indication is resistance to adjuvant therapies. But even beyond these situations, LITT can be used for a wide variety of deep-seated brain tumors, including recurrent tumors.
Q: How should a pediatric center prepare itself to effectively offer LITT?
At the institutional level, successful implementation of this therapy for pediatric populations requires a multidisciplinary approach to cases that includes strong support from the relevant device manufacturers to ensure efficiency of use of the LITT system. Second, the institution must have an intraoperative MRI suite to allow real-time tracking of procedural progress. Finally, the treating surgeon must be thoroughly trained in the procedure and comfortable with this new technology.
Q: What should we look for in the future around development of pediatric LITT?
We are starting to use this therapy more and more in our pediatric populations, but published data remain scarce. I am hopeful we may start to see longer-term follow-up in larger cohorts of pediatric patients to allow better assessment of the efficacy of LITT in preventing tumor recurrence. Ultimately, multicenter trials are needed to better define its role in treating tumors and related pediatric disorders. Meanwhile the MRI-guided LITT systems will continue to evolve and are likely to be made compatible with robotic and computerized simulation applications currently in use.
Advertisement
Advertisement
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits
Newer protocols address testing, language and communication