Findings suggest new ways to improve outcomes
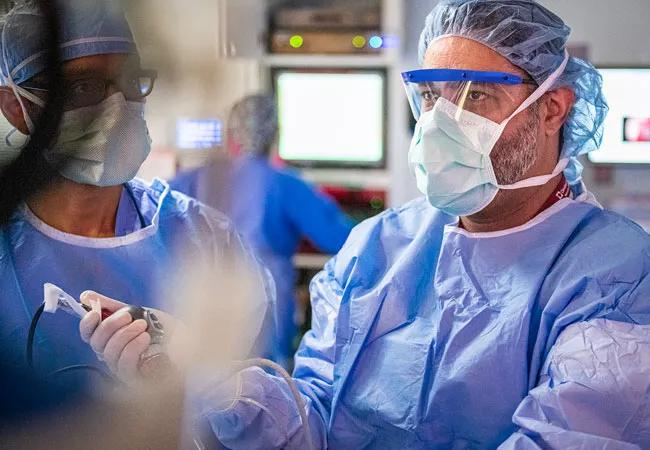
Postoperative visits to the Emergency Department (ED) use considerable healthcare resources and can disrupt recovery for patients at a critical time. To better understand why patients who have endoscopic skull base surgery (ESBS) come to the ED and who are readmitted or discharged, the Cleveland Clinic Head and Neck and Neurological Institutes analyzed ED visits over a five-year period. “Readmissions are recognized as an important measure for healthcare systems. Many patients who are readmitted to the hospital come in from a visit to the ED, and we realized that ED visits after ESBS hadn’t really been looked at before. We wanted to better understand who returns to the ED early after skull base surgery, for what reasons, and what exactly happens after that, in terms of who is admitted and who is not,” explains Raj Sindwani, MD, senior study author and Section Head of Rhinology and Skull Base Surgery and Co-director of the Minimally Invasive Cranial Base and Pituitary Surgery Program.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The investigators did a retrospective review of all Cleveland Clinic ESBS cases from January 2017 through June 2022. Of 559 ESBS cases, 61 patients (10.9%) presented to the ED within 30 days following discharge. The median postoperative day for patients presenting to the ED was six days and 14 patients (23%) missed their first postoperative appointment. The majority of patients – 38 (62.3%) – were discharged home while 23 (37.7%) were readmitted to the hospital.
The most common reasons for ED visits in the group that were later discharged home were headache (15), epistaxis (7) and nausea/vomiting (5); the most common reasons in the readmitted group were nausea/vomiting (7) rhinorrhea (7) and headache (5). The most common readmitting diagnoses were adrenal insufficiency (13%) and hyponatremia (13%). Readmitted patients were significantly older than those who were not readmitted: 63 years vs. 47 years.
Both discharged and readmitted patients had comparable evaluations while in the ED: a median of four blood tests, one imaging study and one consultation.
In a related analysis of the same cohort, investigators looked at the area deprivation index (ADI), a validated measure of socio-geographical disadvantage, and its relationship to postoperative outcomes following ESBS, including ED visits and hospital readmissions within 30 days of surgery. It was the first study to do so. ADI is calculated from United States Census data that has been correlated with a variety of poor medical and surgical outcomes. In this study, ADI scores were obtained using patients’ home addresses.
Advertisement
Patients who were readmitted had a lower median ADI (were more socio-geographically advantaged) than patients who were discharged, 38 compared to 78. Otherwise, there were no other significant differences in demographic, medical or surgical variables between the two groups. “We expected to see differences based on ADI. It’s not surprising that disadvantaged patients have a different relationship with the healthcare system and possibly use the ED for minor complaints,” says Dr. Sindwani. “These results also made us wonder about health literacy, and whether our patients were fully grasping the education we gave them before surgery in relation to what to expect postop.”
The study findings suggest ways to improve patient outcomes and prevent unnecessary ED visits. “We have an opportunity to better educate patients about what is normal and expected after skull base surgery. We can also offer more support, counseling and touchpoints after surgery and perhaps schedule earlier postoperative visits,” says Dr. Sindwani.
Since the most common readmitting diagnoses were endocrine-related, closer follow up with the endocrinology team and greater visibility to these issues during the early postoperative period may help address potential issues.
To ensure that patients appreciate what the postoperative period will be like and when to come back for their first postoperative visit, “we need to consider ADI and look closely at individual patients’ needs, resources and support system,” says Dr. Sindwani.
Advertisement
With more than 60% of patients who present to the ER discharged home, these visits represent another opportunity for improvement. “Perhaps we can streamline the number of tests and consultations to reduce costs and better utilize healthcare resources when patients at lower risk for readmission are identified,” Dr. Sindwani says.
~
In addition to Dr. Sindwani, the investigators included the other members of the Cleveland Clinic Endoscopic Skull Base Team: rhinologist Troy Woodard, MD, and neurosurgeons Varun Kshettry, MD, and Pablo Recinos, MD.
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2241209/13504206)
Advertisement
Advertisement

Despite advancements in the specialty, patient-centered care needs to remain a priority

Novel approach begins reinnervation before tumor resection, preserving a young woman’s smile

This technical solution expedites the patient’s ED to admissions process

Caregiver collaboration and patient education remain critical
Akron General and Union Hospital increase throughput and patient satisfaction by rethinking their approach to care

Structured data helps identify older adults at risk for poor outcomes, defines patients who require more comprehensive assessments

Specialized unit provides patients with faster, more targeted care

Remotely based physicians use telehealth technology to evaluate lower-acuity patients in the ED, express clinic or during an EMS response