Exploring rates, drivers and implications of failed catheter removal
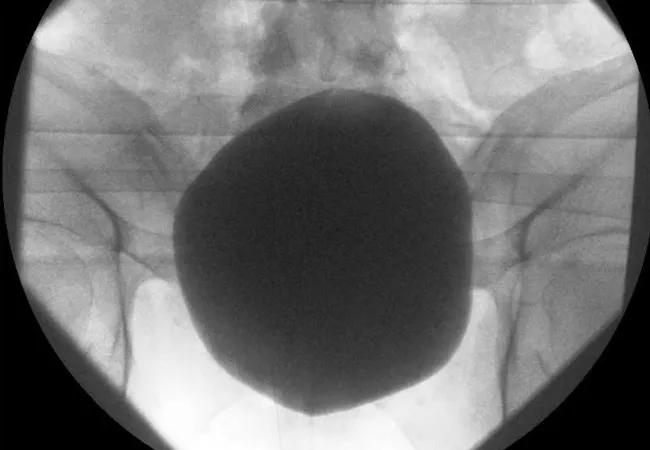
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3072fd5f-7a68-47dc-bc27-c91cfe65233a/cystogram-smooth-bladder_650x450_jpg)
cystogram-smooth-bladder_650x450
Failed removal of indwelling urinary catheters (IUCs) among hospitalized stroke patients is widespread but potentially preventable, according to a Cleveland Clinic study published earlier this year in PM & R, the journal of the American Academy of Physical Medicine and Rehabilitation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The single-center retrospective study documented failed IUC removal in more than a quarter of stroke patients who had an IUC inserted during their admission and identified a number of factors associated with failed removal.
“The problem of failed IUC removal cuts across care venues as patients move from acute care to rehabilitation settings, making it a challenge to study,” says lead author Frederick Frost, MD, Chairman of Cleveland Clinic’s Department of Physical Medicine and Rehabilitation. “Management of failed IUC removal often falls to rehabilitation clinicians.”
“Our study represents a first step toward developing a predictive model that can inform decisions around IUC removal in hospitalized stroke patients,” adds co-author Irene Katzan, MD, MS, a neurologist in Cleveland Clinic’s Cerebrovascular Center.
The study evaluated all 432 patients admitted to Cleveland Clinic’s Joint Commission-certified Comprehensive Stroke Center with a primary diagnosis of ischemic or hemorrhagic stroke over a 20-month period from 2012 to 2014. Of these patients, 175 had an IUC removed. Among those 175 patients, 46 (26 percent) experienced a failed IUC removal, defined as removal followed by a catheter reinsertion.
Factors that were independently associated with failed removal fell into two categories. Those that were known before catheter removal included white race, greater impairment in functional status at admission, and hemorrhagic (rather than ischemic) stroke. Factors that were not known until after catheter removal included greater length of stay in the acute care hospital (likely a proxy for functional impairment) and discharge to a destination other than home.
Advertisement
The study authors note that stroke patients often fulfill numerous criteria for placement of urinary catheters, such as bladder dysfunction and critical illness. They add that catheter-associated urinary tract infection is a serious problem and that reducing ‘catheter days’ is a worthy goal insofar as it targets unjustified catheter use. But the association of IUCs with inpatient morbidity is a complex issue, they contend, since failed IUC removal is itself associated with substantial morbidity, including increased risk of urinary retention and bladder overdistension (as shown in the image at the top of this post).
“There are subpopulations of patients in whom catheters should be left in place, both short and long term,” says Dr. Katzan. “Protocols for reducing catheter days must account for the special situations where IUCs are medically necessary, and equal consideration must be given to identifying patients in whom IUC removal poses more risk than continuing IUC use.”
Rehabilitation professionals are in an ideal position to ensure such protocols are sensitive to these clinical nuances, Dr. Frost observes. “Because we’re adept at managing bladder and bowel care in patients with disabilities, we’re well equipped to educate our acute care colleagues on the implications of failed IUC removal,” he says.
“As we learn more about the clinical scenarios and timing that may predict successful catheter removal, we’re likely to find that delaying removal in selected patients could result in an overall reduction in catheter days,” he notes.
Advertisement
Larger, prospective, multicenter studies will be needed first, he adds, but the current study shows that such studies are warranted.
“Ideally, patients who need IUCs will have them and patients who don’t need them will have them removed, in service of the broader goal of curbing medical complications and facilitating the rehabilitation phase of care,” Dr. Frost concludes.
Advertisement
Advertisement
Inferior clinical outcomes continue into mechanical thrombectomy era, large analysis finds
How to use? Consider starting during the acute attack and seek patient preferences for chronic use
Quantitative imaging adds diagnostic value beyond 3T MRI in nearly half of patients
Expert shares insight on intrathecal baclofen pumps to treat spasticity
Opportunities and impacts of a growing surgical approach
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights