Clinical trial explores utility of HoloLens in percutaneous procedure
A Cleveland Clinic research team recently launched a first-of-its-kind clinical trial evaluating the use of the Microsoft HoloLens augmented reality device for improving the accuracy and effectiveness of percutaneous microwave ablation to destroy liver tumors.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cleveland Clinic research scientists and physicians are adapting HoloLens for use in a wide array of clinical applications. Clinicians are using the fully self-contained holographic computer to enhance the treatment of aortic aneurysms, ovarian cancer and even face transplant surgery. Now they’re adding treatment of liver tumors to the list.
“This is the first time in the world, to our knowledge, extended reality surgical navigation has been evaluated in a liver tumor ablation procedure,” says Karl West, MS, Director of Medical Device Solutions at Cleveland Clinic, staff in Lerner Research Institute’s Department of Biomedical Engineering, and one of the inventors of the technology. “HoloLens provides an entirely different way to visualize the tumor’s location. It is a paradigm shift and may have potential applications for a variety of other procedures and diseases.”
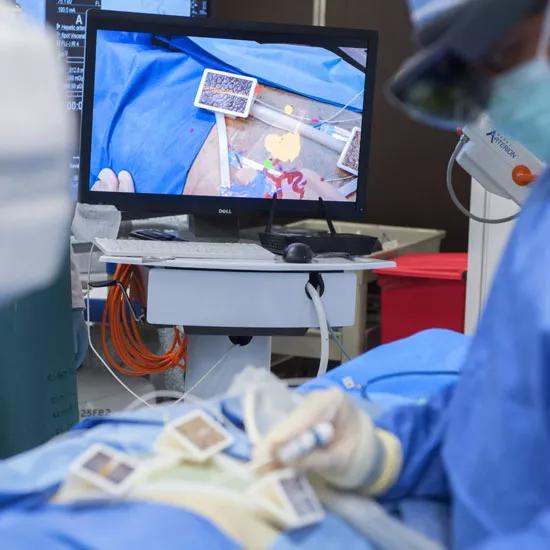
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5238c805-452a-4da5-917b-d5d69000d9b3/HoloLens-screen-in-focus-_550x550_jpg)
The study compares 2D standard of care images (ultrasound, fluoroscopy, CT), displayed on a conventional flat panel screen, with 3D holographic images, which layer virtual projections on top of the user’s real-world view. This 3D holographic image is projected onto the patient, allowing the clinician 360 degrees of visualization for guidance and navigation of tracked instruments.
“The images a surgeon interacts with through the headset are based on real patient data,” says Mr. West. “Once a virtual model is constructed, we mark fixed points in the patient’s anatomy and anchor the model to the patient. We can look down into the patient’s body and see views never before possible.”
Advertisement
Using the holographic image, the interventional radiologist guides a biopsy needle into the tumor with enhanced precision. The team then delivers microwave energy through the needle to heat and destroy the abnormal tumor tissue. Throughout the procedure, the physician uses head-mounted glasses to see the patient’s internal anatomical structures and verify tumor location with the technology’s mini global positioning-like system. In the trial, surgeons and staff will then rate the usability of the system on a Likert Scale.
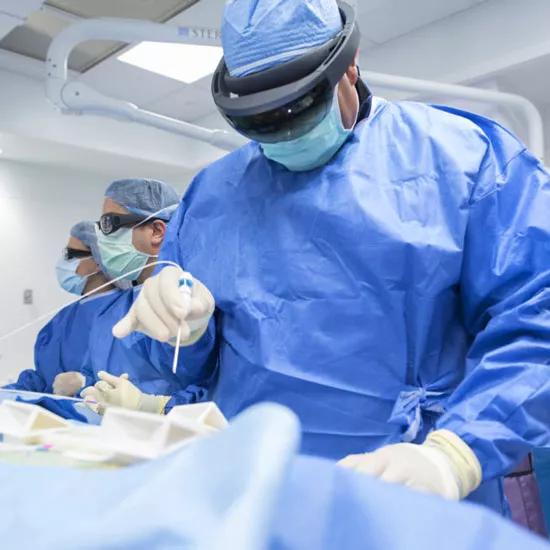
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2214d77a-d1af-4f81-8909-8a6b06f2696a/Dr_-Martin-HoloLens_550x550_jpg)
“We are assessing if this augmented reality system can overcome the limitations of displaying images such as ultrasound, fluoroscopy and CT on 2D flat screens,” says Charles Martin III, MD, Director of Interventional Oncology in the Department of Radiology and principal investigator of the trial. “The transformative technology allows a physician to see the patient’s anatomy in a completely unique way. I feel it can assist in enhancing minimally invasive therapies for patients. It provides an unprecedented ability to better visualize the patient’s anatomical structures and map out the most precise path to the tumor in real time.”
The researchers hope to enroll five patients in the study and complete the trial by the end of 2019.
Advertisement
Advertisement
First full characterization of kidney microbiome unlocks potential to prevent kidney stones
Researchers identify potential path to retaining chemo sensitivity
Large-scale joint study links elevated TMAO blood levels and chronic kidney disease risk over time
Investigators are developing a deep learning model to predict health outcomes in ICUs.
Preclinical work promises large-scale data with minimal bias to inform development of clinical tests
Cleveland Clinic researchers pursue answers on basic science and clinical fronts
Study suggests sex-specific pathways show potential for sex-specific therapeutic approaches
Cleveland Clinic launches Quantum Innovation Catalyzer Program to help start-up companies access advanced research technology