How it’s done and which patients should consider it
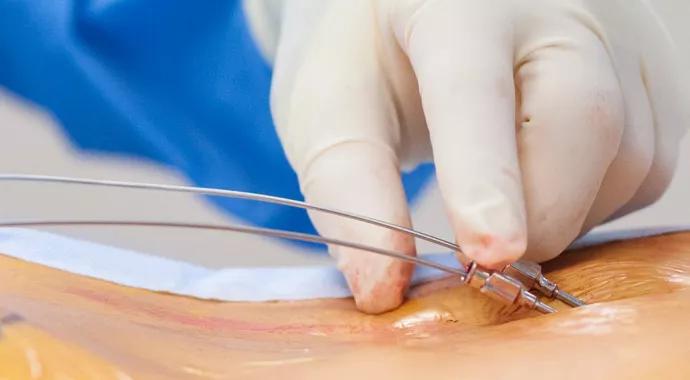
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/97015693-e053-4f4d-a273-cd277a1b0f59/DorsalStim2-690x380_jpg)
DorsalStim2-690×380
By Bruce Vrooman, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dorsal column stimulation (DCS), also known as spinal cord stimulation (SCS), is a neuromodulation therapy that works by applying an electrical current to the spinal cord at the source of the pain. It is an accepted treatment for patients with chronic back or limb pain who have not responded to other treatments. As the nerve fibers are stimulated, patients experience a pleasant sensation rather than the pain that had previously plagued them.
DCS systems have three primary components:
During the outpatient procedure, which takes approximately two hours, patients lie face down. They receive monitored anesthetic care, usually with fentanyl or propofol.
The surgeon makes an incision in the skin superficial to the lumbar spine and over the iliac crest. Using a scalpel, a small pocket – about 1 cm deep – is created to hold the IPG, which can either be rechargeable or non-rechargeable.
Next, the surgeon places a needle into the epidural space above the posterior elements of the spinal cord. This requires a small incision and some dissection with electrocautery. A small space is created under the subcutaneous fat and above the ligament so the needle can enter the epidural space.
Then the surgeon advances two flexible silicone leads through the needle. The leads have anywhere from four to 16 contacts, depending on the extent of the painful region.
Once the leads are advanced into the epidural space, they are steered into the thoracic region for abdominal pain or the cervical region for neck and arm pain. The leads are pulled down slowly while the patient is awake to report the results of the stimulation. Next, the needle is retracted and the leads are secured to ligaments in the back with a silicone anchor.
Advertisement
After the leads are secured, the surgeon uses a tunneling device to reach the pocket where the IPG is implanted. The leads are advanced through a straw to the IPG site, where they are connected and impedance is checked to ensure the leads are working.
Finally, the surgeon irrigates the pocket with an antibiotic solution and secures the IPG with two silk sutures. A mix of deep dermal sutures, subcuticular sutures and surgical glue is used to close the incisions and epidermis before a small dressing is applied.
Programming of the IPG occurs in the recovery area, and the patient is given the generator remote to control the DCS system.
DCS is not for everyone. It’s suited to chronic pain patients who have exhausted other treatment options and have reasonable goals for relief and resumption of normal activities. It is an elective treatment that can work in conjunction with medications and conservative therapies.
DCS is a relatively new treatment for neuropathic abdominal pain. More commonly, the therapy is used to treat:
It’s critical that patients rule out any organic cause for pain prior to undergoing DCS. At Cleveland Clinic, all candidates for the procedure must first meet with a pain psychologist, who runs a series of tests to evaluate the patient’s expectations. Then the case is presented to an interdisciplinary committee to discuss the patient’s background and confirm that other pain management options have been explored. For those who fit the criteria, DCS can be a good option to manage chronic pain.
Advertisement
Dr. Vrooman is a pain management specialist and anesthesiologist in Cleveland Clinic’s Department of Pain Management. He can be reached at vroomab@ccf.org or 216.445.9641.
Advertisement
Advertisement
Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies
Study participants also reported better sleep quality and reduced use of pain medications
Two-hour training helps patients expand skills that return a sense of control
Program enhances cooperation between traditional and non-pharmacologic care
National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
Pain specialists can play a role in identifying surgical candidates
Individual needs should be matched to technological features
New technologies and tools offer hope for fuller understanding