Special glasses allowed surgeon to see 3D models and anatomic data superimposed on surgical field

A 60-year-old man with knee osteoarthritis presented at Cleveland Clinic London as a candidate for total knee replacement. Knee pain had dramatically reduced his quality of life as he was otherwise healthy and active. To optimise results of the surgery, the team at Cleveland Clinic London proposed a robotic-assisted knee replacement supplemented with augmented reality (AR) — technology rarely used in the U.K. and never before offered in London.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A relatively new concept in orthopaedic surgery, AR is not widely used in joint replacement. The system used at Cleveland Clinic London was introduced in 2021.
“In the past, orthopaedic surgeons had one replacement procedure for everyone — one way to insert implants,” says consultant orthopaedic surgeon Panagiotis Gikas, MBBS, MD, PhD, of Cleveland Clinic London. “Now with more advanced technology, we’re moving toward personalised medicine. Robotics was one step. The next step is AR, which provides more anatomic information for each patient, allowing surgeons to perform cuts at specific places, tailored to the specific anatomy. Ultimately, this should translate to better outcomes for patients.”
Prior to the procedure, Mr Gikas and the surgical team used advanced imaging software to visualise the patient’s knee joint in 3D. The virtual model, based on the patient’s CT imaging, helped the surgical team evaluate damaged bone and cartilage and determine the ideal size and position of the knee implant to restore the patient’s specific anatomy and preserve individual biomechanics. The model’s simulation of post-operative range of motion also contributed to preoperative decision-making.
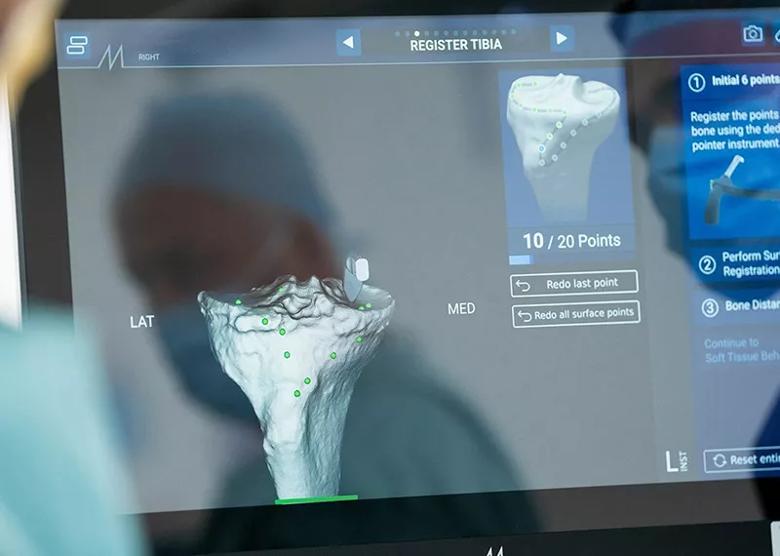
The patient was prepared for surgery, which included attaching two sensors, one in the patient’s femur and one in the tibia. These sensors would later provide real-time feedback to the surgical team, similar to other sensors attached to robotic surgery systems. However, by attaching sensors to the patient’s anatomy, close to the surgical field, the team did not need to limit their movement in the surgical theatre to avoid blocking the robot’s view of the field. In addition, sensors were inserted through the same incision, preventing the multiple incisions needed to attach sensors for other robotic systems.
Advertisement
Following registration of the patient’s knee, both in terms of static anatomy as well as dynamic ligament and soft-tissue tension, the team used the advanced AR software to choose the most appropriate bone cuts to optimise positioning of the implant. The goal was to replicate the patient’s exact physiologic biomechanics.
The surgical system’s tracking technology then guided the team’s instrument placement and implant position.
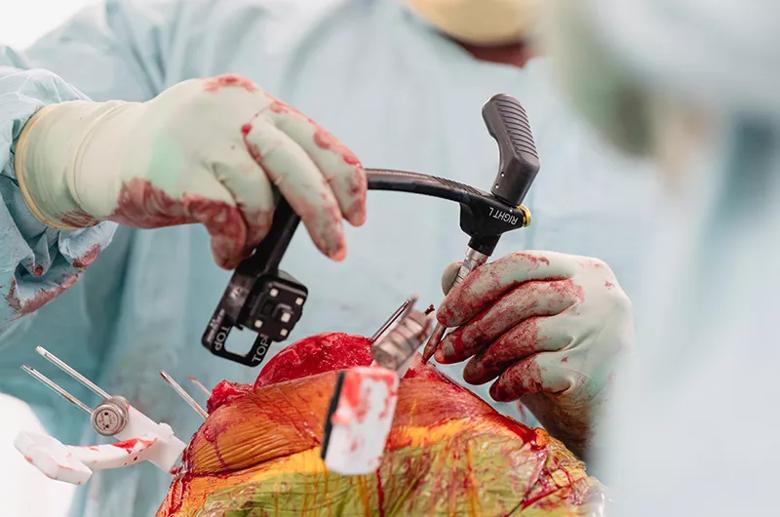
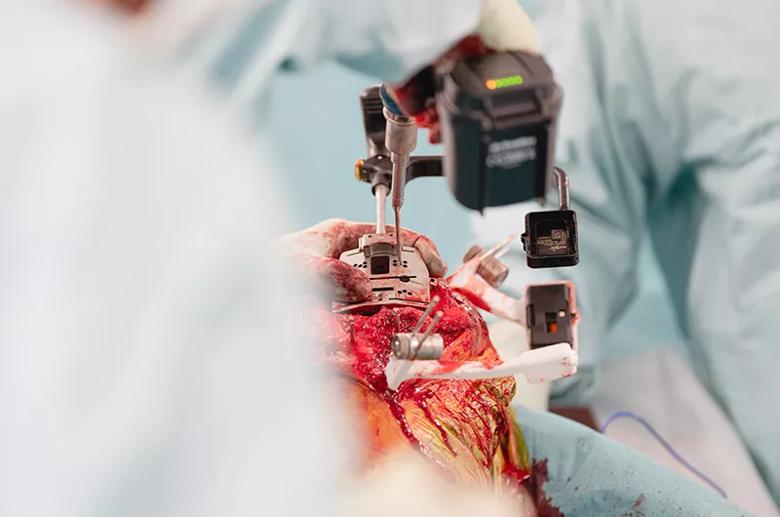
Throughout the procedure, Mr Gikas wore AR glasses, which displayed not only an interactive 3D model of the patient’s knee but also the patient’s anatomic data as if superimposed on the surgical field. AR experts call this “enhanced visualisation.”
“I could see the knee and see the measurements at the same time, rather than needing to look up from the field to see data on a monitor,” says Mr Gikas. “It provided a more intuitive environment in which to operate and helped enhance my decision-making in real time.”
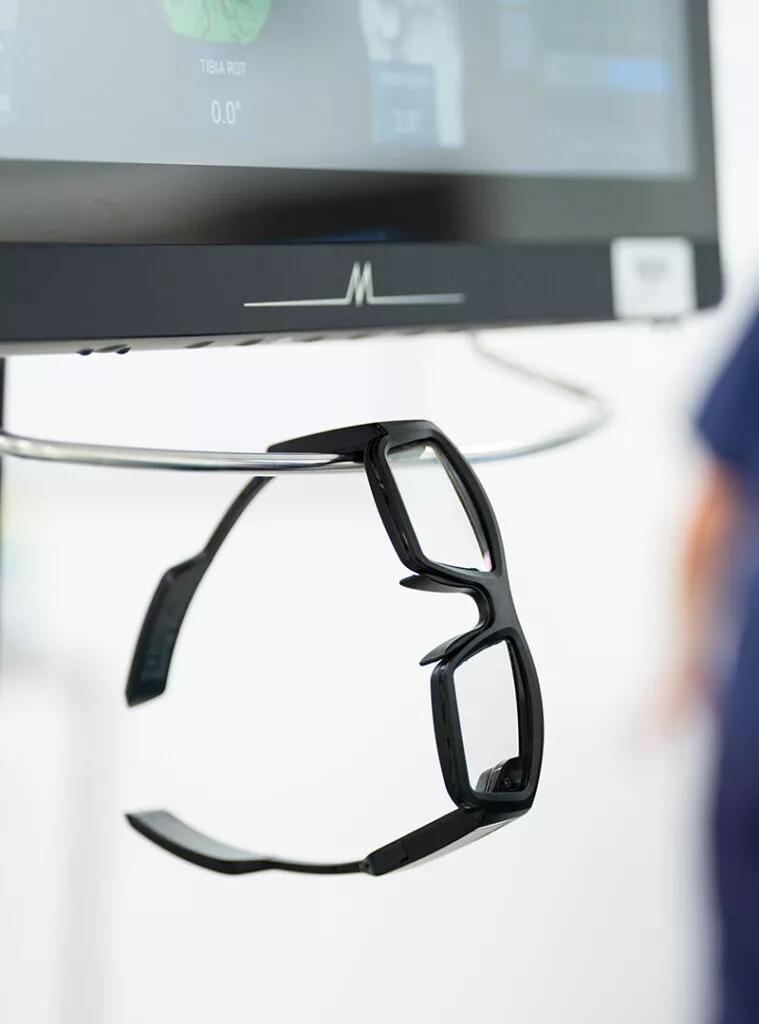
In addition to static anatomic measurements, which are common in robotic surgery systems and valuable in directing the position of implants, the AR-based system provided functional measurements, such as ligament tension.
“We were able to measure the tension of ligaments around the knee before the surgery and then ensure we replicated those measurements after the implant was positioned,” says Mr Gikas.
One day after surgery, the patient was able to walk and bend his knee to 90 degrees. The patient was walking independently at two weeks and returned to work, driving and other activities of daily living at four weeks.
Advertisement
“No randomised studies exist to show the advantages of using this technology versus conventional procedures, but orthopaedic practitioners know that more accuracy is always a good thing,” says Mr Gikas. “If we can cut a bone within 1 mm of accuracy and take steps to precisely match a patient’s post-operative function to their native function, it can only mean better outcomes for the patient.”
Surgical technologies incorporating AR are the newest frontier in orthopaedics, he adds, helping surgical teams tailor care for the unique anatomy and specific needs of each patient.
Cleveland Clinic uses AR technology in joint replacement procedures at its main campus in Cleveland, Ohio. AR also has been adapted by Cleveland Clinic research scientists and physicians for use in a wide array of clinical applications, from treating aortic aneurysms to treating liver cancer to completing a total face transplant surgery.
Advertisement
Advertisement

Self-care may be just as effective for some patients

Most return to the same sport at the same level of intensity

Higher than 5-year rates for prostate cancer and melanoma and about the same as breast cancer

Insights to help orthopaedic practices comply with the 2025 CMS mandate

Dr. Piuzzi wins 2025 Kappa Delta Young Investigator Award for pioneering work

Largest cohorts to date reveal low rates of major complications

More report a clinically meaningful change in function at 90 days compared to patients with lower BMI

Patient climbs Mount Kilimanjaro 8 months after surgery