A broad differential diagnosis
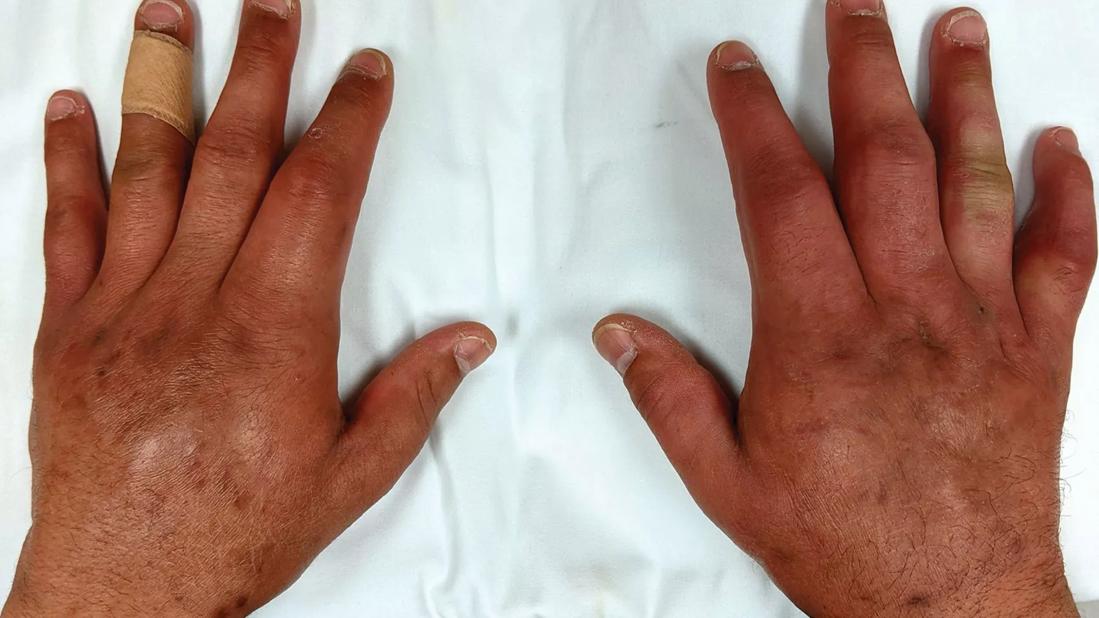
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0d3a8723-472e-4e85-a6b4-b9badc032b06/F1_large__jpg)
puffy hands
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A 37-year-old man presented to the rheumatology clinic for evaluation of swelling of his fingers and hands. The symptoms began eight months earlier and at first were intermittent, but in the last four months, they had become persistent. The swelling started in the right (nondominant) hand, and then affected the left hand within a few weeks.
He reported limited range of motion in his fingers and wrists, with loss of hand dexterity and difficulty picking up objects or putting on socks and shoes. He denied any features suggestive of systemic sclerosis, including Raynaud phenomenon, ischemic digital ulcers, heartburn, dysphagia, dry cough and exertional shortness of breath. He reported no other chronic medical illness.
He said he smoked marijuana and half a pack of cigarettes per day. After two years of sobriety, he had restarted using intravenous (IV) drugs (opiates and methamphetamine) about one month earlier.
On examination, the dorsal and palmar aspects of both hands, fingers and wrists were diffusely swollen with limited range of motion. However, there was no clinical evidence of inflammation (synovitis) of the wrist and finger joints, i.e., no joint swelling, tenderness, heat or redness.
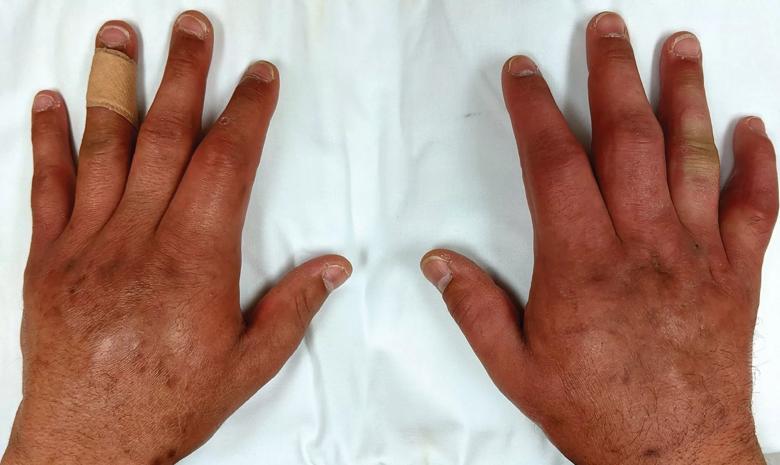
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0d3a8723-472e-4e85-a6b4-b9badc032b06/F1_large__jpg)
Both hands, including fingers and wrists, were diffusely swollen, with limited range of motion.
Laboratory studies revealed a normal complete blood cell count, comprehensive metabolic panel, C-reactive protein and thyroid-stimulating hormone level. Other tests with negative results included urine toxicology screen, hepatitis B and C and human immunodeficiency virus serology, and testing for rheumatoid factor, anti-cyclic citrullinated peptide antibody, antinuclear antibody and antibodies to extractable nuclear antigens.
Advertisement
A radiograph of the right hand showed diffuse soft-tissue swelling. Computed tomography of the right hand also showed diffuse soft-tissue edema and skin thickening, most prominent over the dorsal side. There was no enhancing fluid collection or gas in the soft tissues and no bony cortical destruction. Based on the presentation, the history and the evaluation, the diagnosis was puffy hand syndrome.
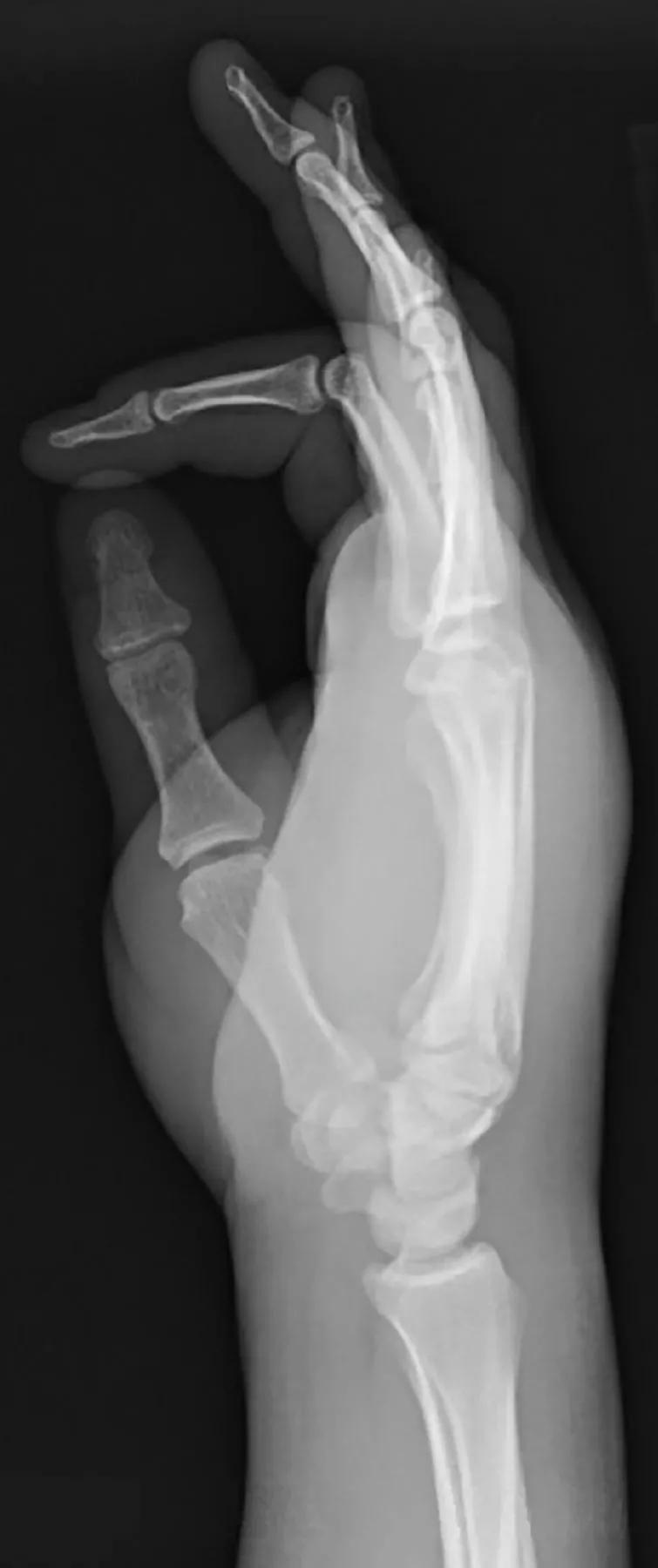
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/e3e7e884-f1dc-45ff-b97c-4f95c81cc746/F2_large__jpg)
Radiography of the right hand showed diffuse soft-tissue swelling.
Puffy hand syndrome, a common complication of IV drug use, is not a well-recognized condition among general practitioners. However, addiction specialists, dermatologists and vascular medicine specialists are familiar with this syndrome.
In patients who do not volunteer a history of IV drug use, a rheumatologist may also be consulted, as the differential diagnosis includes scleroderma, mixed connective tissue disease and the syndrome of remitting seronegative symmetrical synovitis with pitting edema (RS3PE).
The precise pathogenesis of puffy hand syndrome remains unknown. Hand edema, which is initially pitting, becomes more indurated over time, as there is progressive fibrosis of the subcutaneous tissues. The swelling is asymmetric and intermittent at first, often affecting the nondominant hand; over time, it becomes persistent and symmetric, as in this patient.
Repeated injection of agents that can induce vascular and dermal sclerosis results in an inflammatory reaction with granuloma formation, similar to a foreign-body granulomatous reaction. Over time, the dense dermal fibrosis obscures the superficial veins and the extensor tendons on the dorsum of the hands. The edema is painless and nonpitting and is unaffected by elevation. Edema may also affect the feet when injection drug users use veins in the feet, legs or groin.
Advertisement
The main risk factors are repeated injections in the superficial veins on the dorsum of the hands (preferred by IV drug users because of easy access), and not using a tourniquet during the injections. The condition is more common in females. The risk increases with unsterile injection practices, suggesting that repeated local infections also contribute to the lymphatic destruction and consequent lymphedema.
Neviaser et al performed venography, lymphangiography, and deep-skin biopsies in 4 patients with puffy hand syndrome. Deep venous patterns were entirely normal. In contrast, lymphangiograms showed extensive collateralization at the elbow, suggesting the destruction of deep lymphatic channels. Biopsy studies showed extensive fibrosis in the subcutaneous tissues.
This study indicated that puffy hand syndrome results primarily from lymphatic obstruction, and that there may be concomitant local scarring resulting from inflammatory reactions at injection sites. Venous obstruction does not appear to play a primary role but can coexist in some cases. Repeated insults are needed for swelling to develop.
The differential diagnosis of puffy hand syndrome is broad and includes conditions that cause anasarca, such as congestive heart failure, nephrotic syndrome, cirrhosis of the liver and severe hypoalbuminemia. Other causes include upper-extremity venous thrombosis, deep palmar space infection, complex regional pain syndrome, lymphedema resulting after axillary lymph node removal or irradiation, and filariasis.
Advertisement
Rheumatologic diseases causing puffy hands include rheumatoid arthritis, crystal arthropathies, systemic sclerosis, mixed connective tissue disease, nephrogenic systemic fibrosis and RS3PE syndrome.
A thorough history and physical examination, followed by judicious use of laboratory and other investigations, should help determine the underlying cause of puffy hands.
Treatment is mostly symptomatic. Intravenous drug use should stop permanently. Long-term use of low-stretch bandages and elastic compression gloves may be useful in decreasing the puffiness of the hands and fingers.
Our patient quit IV drug use and is currently undergoing drug rehabilitation and psychiatric counseling. So far, he has not regained much movement in his hands and fingers.
Dr. Chatterjee is staff in the Department of Rheumatology in the in the Orthopedic and Rheumatologic Institute. This article is republished with permission from the Cleveland Clinic Journal of Medicine.
Advertisement
Advertisement
Researching the biological basis for why treatment is or is not effective
Scribing system helps create more face-to-face interactions
A conversation with Leonard Calabrese, DO
The case for continued vigilance, counseling and antivirals
High fevers, diffuse rashes pointed to an unexpected diagnosis
No-cost learning and CME credit are part of this webcast series
Summit broadens understanding of new therapies and disease management
Program empowers users with PsA to take charge of their mental well being