A pharmacogenomics clinical specialist urges caution
by Jennifer Hockings, PharmD, PhD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
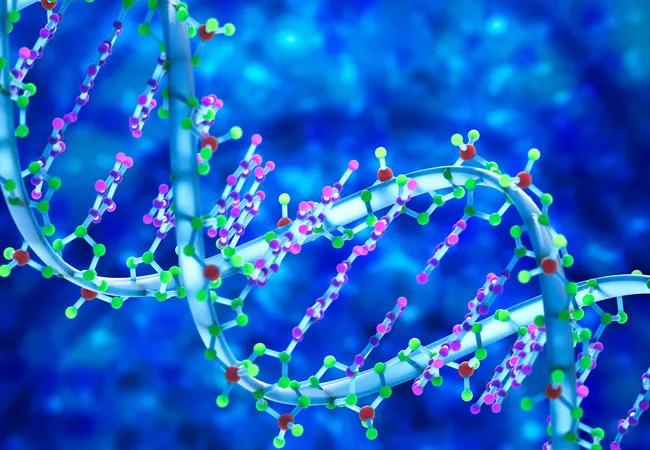
On October 31, 2018, the Food and Drug Administration (FDA) announced its approval of the first direct-to-consumer (DTC) pharmacogenomics test. Pharmacogenomics is the study of how an individual’s genetic variations impacts his or her response to drugs. Pharmacogenomics testing can help providers prescribe medications and doses that are safe and effective by optimizing clinical outcomes with minimal adverse effects.
The DTC test will be performed and marketed by 23andMe, a company well-known for its DNA testing services originally focused on genealogy. In recent years, 23andMe’s services were expanded to include genetic health risk and carrier status reports, which the company has collated under health services. According to the FDA, the pharmacogenomic reports from 23andMe are not intended to guide treatment decisions, as they do not provide information on specific response to medications. Rather, the intent is to help patients frame discussions with their healthcare providers. Results would need to be confirmed with an independent clinical pharmacogenomics test.
With any DTC pharmacogenomics tests, healthcare providers must keep significant limitations in mind. First, there are limited variants for each gene that are detected and reported. Variants that are not tested for will result in a report of *1, indicating a normal function allele for that gene. Individuals with two *1 alleles are considered to be normal metabolizers for that gene, showing that the patient can tolerate certain medications at labeled doses. 23andMe will report on eight genes involved in drug metabolism with a total of only 33 variants — variants that are expressed at a higher allelic frequency in the Caucasian population. Unfortunately, variants that are expressed at higher frequency in patients of African, Asian and Hispanic populations are not included in the 23andMe test, which may lead to false reports about the number of patients with “normal metabolizer” phenotypes and inaccurate discussions between patients and clinicians.
Advertisement
Equally concerning, in my opinion, is that it is not clear from the information provided by the FDA whether 23andMe will detect copy number variants for CYP2D6. This detects individuals who have deletions or extra copies of CYP2D6, which corresponds to loss or gain of function, respectively. The impact of altered CYP2D6 function can be illustrated with codeine and tramadol. Both drugs are metabolized by CYP2D6 to their respective active metabolites to provide pain relief. Those patients with additional copies of CYP2D6 are at risk of adverse effects, including respiratory depression and excessive somnolence, whereas those with deletions may not experience pain relief. It would be difficult to accurately predict response to either medication if copy number variants were not included in the report. It is possible that the FDA has emphasized that patients and clinicians should not use DTC tests for treatment decisions for this reason.
While the approval of the first DTC pharmacogenomics test provides exciting opportunities to educate the general public about the clinical value of pharmacogenomics, it also must be viewed with caution. Perhaps the silver lining is that, with this approval, the FDA is establishing criteria and expectations to help standardize pharmacogenomic testing. Moving forward, this may lead to pharmacogenomics-guided therapy as standard of care.
Dr. Hockings is a pharmacogenomics clinical specialist for the Genomic Medicine Institute.
Advertisement
Advertisement

Study identifies Ketorolac as a potential repurposable drug

The relationship between MTHFR variants and thrombosis risk is a complex issue, but current evidence points to no association between the most common variants and an elevated risk

One-time infusion of adenovirus-based therapy is designed to restore heart muscle function
Cleveland Clinic researchers receive $2 million grant from the National Institutes of Health

New Cleveland Clinic fellowship fosters expertise in the genetics of epilepsy
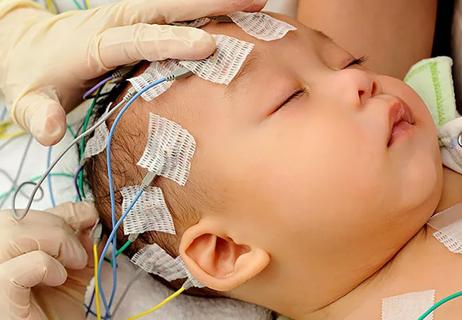
Integrates genetic and clinical data to distinguish from GEFS+ and milder epilepsies

First-of-kind study aims to enable prevention of brain disorders before symptoms appear

Advanced genomic research techniques show potential to treat a variety of conditions