Initially under-recognized, cutaneous manifestations are increasingly reported
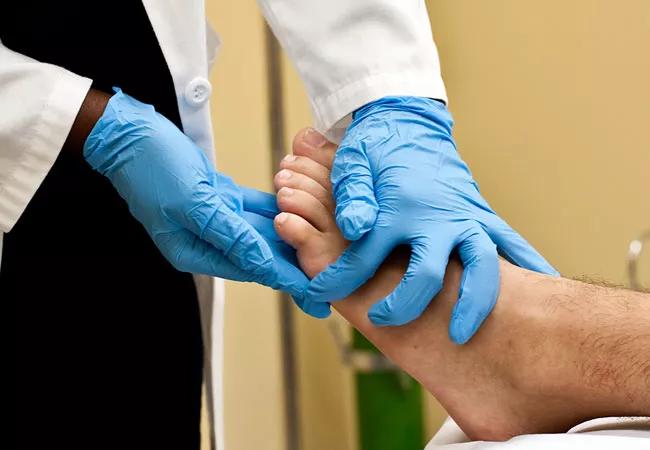
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/31b15459-aaac-410a-9950-54748c3c7073/20-PSX-1887418_CQD_650x450_157586048_jpg)
20-PSX-1887418_CQD_650x450_157586048
Although the recently expanded list of COVID-19 symptoms does not include skin changes, such as rash or discoloration of digits, we are seeing an increasing number of reports, says Sarah Young, MD, a medical dermatologist at Cleveland Clinic.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As of April 29, 2020, the U.S. Centers for Disease Control and Prevention lists the following as symptoms of COVID-19: cough, shortness of breath, fever, chills, repeated shaking with chills, diarrhea, muscle pain, headache, sore throat and new loss of taste or smell. While this is a wide range of symptoms, there has been more limited discussion of cutaneous manifestations of COVID-19.
“The symptoms of COVID-19 are evolving, but do not yet include rash. At this point, when we see rashes in patients, we should still follow the standard protocol to determine — based on symptoms, risk factors and exposures — if screening for COVID-19 is appropriate,” Dr. Young says.
“There currently is not enough data to support that a rash alone is enough to warrant testing for COVID-19, especially in light of the limited number of tests available right now. Assuming some of these rashes are true manifestations of COVID-19, we also do not yet know an exact timeline as to when the rash starts in the disease process, at what point the patient might test positive for COVID-19, and when to expect resolution. Our goal would be to prognosticate based on the rash, but at this point we just don’t have the data,” she says.
The term COVID toes is fairly a nonspecific term used to describe a purple or pink discoloration often with papules involving the tips of the toes, Dr. Young says. At this time, there appear to be multiple causes of this finding, including either impaired blood flow to the toes or pernio or chilblain-like toes. There are sometimes subtle differences in the appearance of these types depending on the cause, and this is where a dermatologist can be helpful.
Advertisement
“We know that in general, patients with COVID-19 are in a proinflammatory state and are at risk for clotting. It’s too early to say at this point, but we’re trying to investigate systemic inflammation and clotting as possible different causes of COVID toes based on the individual patient. Since everyone’s body reacts differently to exposure to the virus, we don’t know which factors determine a patient’s presentation or outcome,” Dr. Young states.
The rashes are generally nonspecific in appearance and varied (i.e., a rash on the whole body vs. COVID toes). Sometimes they are asymptomatic; however, the rashes have also been described in the literature as painful or itchy, or both.
These rashes seem to mimic rashes we have commonly treated in dermatology clinics prior to the pandemic, explains Dr. Young. The first step toward treatment is determining the cause of the toe discoloration. Then, treatment focuses on the underlying cause. If the cause of the COVID toes is related to impaired blood flow, Dr. Young states that critically ill patients could potentially be at risk for skin damage or damage in other organs if impaired blood flow is also occurring elsewhere in the body.
Perhaps partly because the rashes were so similar to those seen before COVID-19, it seems that they may have been initially under-recognized.
“The rashes could look like hives, a reaction to medication, or perniosis. Since all these causes were varied and existed prior to COVID-19 but were associated with other entities, it was hard to pick up that the rashes were related to COVID-19. I think we’re recognizing it now because as more reports of rashes emerged, more physicians began looking for the rashes. The rashes are gaining recognition not just among providers, but also with patients. Finally, the use of teledermatology in the United States may be helping us to associate the rash with COVID-19, as dermatologists are able to extend themselves virtually to see more patients,” says Dr. Young.
Advertisement
As medical professionals around the world have worked to understand this evolving pandemic, many have shared their experiences in the literature. But there is still not much data.
“At Cleveland Clinic, we’re seeing findings similar to those reported in the literature at large. However, similar to what’s happening at those other institutions, not every patient with these rashes warrants testing. The only true way to know if they are related to COVID-19 is if every patient is tested, which isn’t always appropriate,” Dr. Young continues.
“Because of the nontraditional ways we’ve been collecting information, and the fact that not everyone is eligible for COVID-19 testing, we don’t have enough data to characterize the rashes at this point. We don’t know which age group is more likely to develop the rash, what other conditions might make patients more susceptible to rash, when the rash is specific to COVID-19 or being caused by other factors, or how patients that develop rash will fare compared to those who do not.”
“I think we’re still in a data collection phase when it comes to these rashes,” Dr. Young cautions.
She notes that it is important to remember that just because a patient has a rash on their toes, it doesn’t necessarily mean that they have COVID-19. Dr. Young encourages providers to include dermatology in patient assessment when rash is present, but then to send the patient through the standard screening protocol to determine whether or not they are eligible for testing.
Documenting cases is also important. In an effort to streamline data collection, Dr. Young and others at the Cleveland Clinic are creating a COVID-19 patient registry to specifically study the skin rashes occurring in these patients. Additionally, the American Academy of Dermatology has developed a COVID-19 Dermatology Registry. In this registry, physicians and health care professionals treating COVID-19 patients can log any dermatologic manifestations of COVID-19, or document patients with an existing dermatologic condition who develop COVID-19, for future research.
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19