Results from calcification volume quantification of intracranial and extracranial arteries
CT angiography-derived severity of calcium burden of the intracranial and extracranial arteries in ischemic stroke patients correlates with older age, smoking and large artery atherosclerosis. And calcification volumes can help differentiate ischemic stroke mechanisms in patients younger than age 65. So conclude two studies of a Cleveland Clinic stroke registry using automated quantitative analysis of vascular calcification volumes presented at the 2020 International Stroke Conference this week.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“CT angiography of the head and neck for acute stroke is now routine in many emergency departments, providing a wealth of potentially useful information for clinical and research purposes,” says stroke neurologist Ken Uchino, MD, Head of Research and Education in Cleveland Clinic’s Cerebrovascular Center and principal investigator of both studies. “Systematic automated quantification of images of the aorta and neck and brain arteries reveals important clues about the causes and risk factors of ischemic stroke.”
While calcification of the aorta and coronary arteries has been studied extensively relative to the risk of cardiac events, vascular calcification measures of head and neck vessels are underutilized to evaluate ischemic stroke risk, although such measures are now frequently obtained from patients with suspected stroke. In addition, the significance of vascular calcifications in relation to stroke mechanisms is not well understood.
These investigations used available CT angiography images from Cleveland Clinic’s recent experience with patients with acute ischemic stroke. Researchers employed machine learning techniques to measure the volume of vascular calcification in the images in order to identify risk factors for ischemic stroke and glean information on underlying stroke mechanisms.
Both studies assessed CT angiograms from 388 consecutive patients (55% male; mean age, 66.6 years) managed for acute ischemic stroke in 2018 from a prospective Cleveland Clinic registry. Calcification volumes in the intracranial, extracranial and aortic arteries were measured by automatic artery and calcification segmentation methods and analyzed using deep-learning U-net model and region-growing algorithms. Severe vascular calcification was defined as the upper quartile calcification volume (> 812 mm3).
Advertisement
One investigation found that the presence of severe calcification was independently and significantly increased in the following groups:
Older age was the most significant risk factor identified, with mean calcification volumes ranging from 225 mm3 in patients younger than 60 years to 1,213 mm3 for patients 80 years or older.
The second study analyzed the relationship between calcification volumes and stroke subtypes, using the TOAST classification. Among the 388 registry patients in the analysis, the overall prevalence of atherosclerotic calcification was 95.9%. Stroke subtypes among these patients broke down as follows:
In patients younger than age 65 years, calcification volumes correlated significantly with stroke subtype, with large artery atherosclerosis having significantly higher mean volume (567 mm3) relative to cardioembolism (213 mm3; P = 0.021) other/undetermined (180 mm3; P < 0.001) and small vessel occlusion (176 mm3; P = 0.014). In patients older than 65, calcification volume differences between subtypes were not statistically significant.
Advertisement
According to Dr. Uchino, the studies yield the following take-home messages:
“CT angiography is currently used for ischemic stroke patients mainly to find severe stenosis as a cause of stroke and to target occlusion for acute reperfusion therapy,” he observes. “But with automated quantification of vascular calcification, we may be able to classify the cause of stroke more easily and gain important insights into underlying mechanisms.”
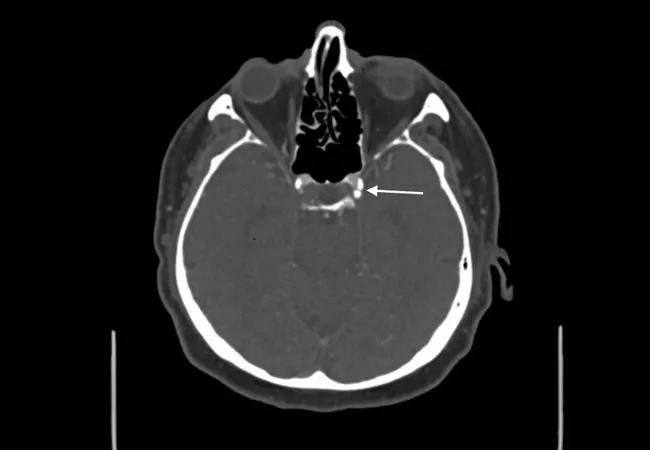
Image at top shows calcification (arrow) in the intracranial carotid artery of a patient with acute ischemic stroke.
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help