A reduction in the number of incisions for implantation simplifies the procedure and improves patient experience
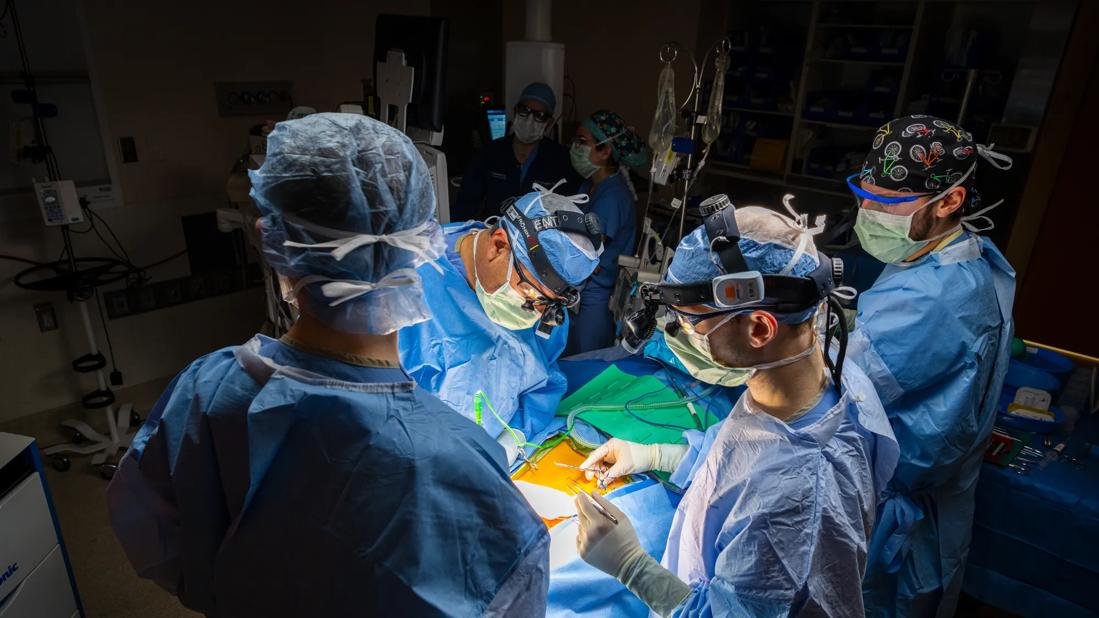
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2ed21f39-4b91-4253-8cbb-3be21662717e/Hypoglossal-Nerve-Stimulation-kominsky)
Kominsky, MD, in surgery
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The FDA recently approved an improvement to a surgical procedure for implanting a neurostimulation device to treat obstructive sleep apnea (OSA). The Inspire® Upper Airway Stimulation (IUAS) device is used to treat patients with moderate to severe sleep apnea who were unable to use CPAP. Originally, the implantation procedure required three incisions, but the FDA has now approved a two-incision implant procedure, which reduces procedure time and pain for the patient.
Surgical therapy has been part of the comprehensive treatment options for obstructive sleep apnea (OSA) over the past 40 years. A new category of surgical therapy became available in 2014 when the FDA approved the first neurostimulation device for the treatment of OSA. In addition to moderate to severe apnea, other criteria for IUAS include an apnea-hypopnea index between 15 and 65, BMI in the 32-35 range (depending on insurance carrier), less than 25% central apneas and age 18 and above.
The IUAS consists of three parts —the implantable pulse generator (IPG), a stimulation lead and a sensing lead. The original outpatient surgery required three separate incisions in order to implant the device. One incision is made in the upper neck to place the stimulation lead around the hypoglossal nerve, and another incision is made in the upper chest to place the IPG.
The third incision is made over the lateral chest to place the sensor between the 5th and 6th ribs. Once implanted the device is activated, it works by sensing the patient’s respiration and creating a coordinated stimulation of the tongue. This stimulation stiffens and protrudes the tongue slightly which opens the airway while sleeping.
Advertisement
Following the FDA approval for the two-incision approach, the IPG and the sensor are now placed through the same incision. The sensor is placed deep onto the pectoralis major muscle between the second and third ribs in the anterior chest. This new technique is an improvement over the three-incision version.
The surgery, which originally took around 100 minutes on average, is shorter by about 20 minutes because there is one less incision to create and then sutured closed. The patient also has a smoother recovery because there is one less surgical site that could cause post-operative pain. This is also beneficial for women who wear a bra because this third incision was positioned under the area of the typical bra strap.
Recovery is usually about 7-10 days due to some soreness at the operative sites. Patients are advised not to resume any strenuous activity for 3-4 weeks after surgery.
The Inspire implant program at Cleveland Clinic leverages the multidisciplinary nature of our group. Close collaboration between sleep medicine providers and sleep surgeons creates an environment of success for our patients. The Cleveland Clinic group model promotes interdisciplinary care. Constant communication between providers promotes improved results. If there are any issues that need to be addressed after activation, there is an easy pathway for surgical reevaluation.
An international multi-institutional registry of implanted patients, which the Cleveland Clinic is a part of, showed the success rate of the therapy to be between 70 and 80%. This new technique will maintain that excellent success rate while increasing patient satisfaction due to having one less surgical site.
Advertisement
Advertisement
Systematic review indicates more can be done for higher-risk patients
Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor
Case study illustrates the potential of a dual-subspecialist approach
Evidence-based recommendations for balancing cancer control with quality of life
Study shows no negative impact for individuals with better contralateral ear performance
HNS device offers new solution for those struggling with CPAP
Patient with cerebral palsy undergoes life-saving tumor resection
Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition