Glaucoma specialist lends remote monitoring units to patients
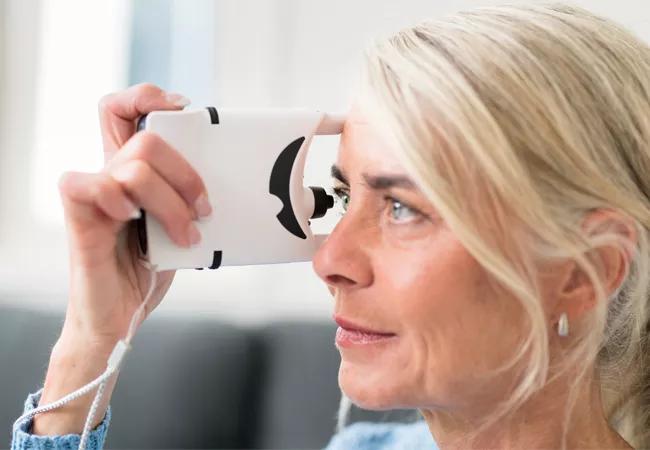
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/cda2846a-2498-448a-be99-f6620afbb3eb/22-EYE-2846128-CQD-Glaucoma-Home-Tonometry_Sood_650x450_jpg)
22-EYE-2846128 CQD-Glaucoma Home Tonometry_Sood_650x450
Patients with conditions like diabetes and hypertension routinely monitor key indicators at home, so why not patients with glaucoma? That’s the thinking behind the growing use of home tonometry.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Eye pressure is critical when monitoring patients for glaucoma,” says Shalini Sood-Mendiratta, MD, a glaucoma specialist at Cleveland Clinic Cole Eye Institute. “Taking pressure readings at home can provide valuable insights and guide clinical care decisions.”
That’s especially true for patients with low-tension or normal-tension glaucoma, whose disease may be progressing even though their eye pressure is not high. Monitoring pressure at home can reveal fluctuations not evident in an office setting.
“We might be missing those patients who have pressure spikes when they’re not in our office,” says Dr. Sood-Mendiratta. “Home monitoring gives a better assessment of how well their disease is actually controlled.”
Studies have shown that eye pressure fluctuates for many patients with glaucoma, and that the highest pressure readings can occur in the late afternoon or evening.
That was the case for one of Dr. Sood-Mendiratta’s patients, whose glaucoma was worsening even though his eye pressure readings during office visits were normal.
“This patient wanted more data, so he bought himself a home tonometry unit,” she says. “We found he was having pressure spikes later in the day. We realized that he does have these larger fluctuations, which explained why we’re seeing progression of his disease.”
The case was an “aha!” moment for Dr. Sood-Mendiratta and motivated her to expand use of home tonometry in her practice. Her office recently acquired six home tonometry devices and began lending them to patients. The program will expand to 10 devices by summer 2022.
Advertisement
In addition to revealing hidden fluctuations in pressure, home tonometry can be a valuable tool for patient education, she said.
Glaucoma is often called the “silent thief of vision” because it can progress without causing symptoms. That can make it tough for patients to consider potentially burdensome or invasive treatment options, like medication or surgery. The patient may not see an immediate need or benefit.
“Home tonometry devices can help support conversations between patients and physicians,” says Dr. Sood-Mendiratta. “Collected data give feedback to the patient to help them better understand if their disease is well controlled or not, and appreciate management recommendations from the clinician.”
In addition to guiding treatment decisions, home tonometry could be used to follow patients over time to determine if treatment is working.
The U.S. Food and Drug Administration approved the first home tonometry device in 2017. Adoption of home tonometry increased during the COVID-19 pandemic, when more ophthalmologists began looking for remote monitoring options.
Dr. Sood-Mendiratta began using the device in her clinic during the pandemic because it did not require anesthesia and required less proximity to the patient than traditional tonometry. To take a reading, the patient holds the device to their eye and aligns it by looking at a green light. They then press a button to release a disposable probe. Measurement is based on how quickly that probe rebounds.
When patients borrow one of these devices for at-home use, they measure their eye pressure multiple times a day for approximately two weeks, and then return the device to the clinic. Technicians upload the data, and the physician reviews the results with the patient at a follow-up in-person or virtual visit.
Advertisement
“In the future, not everything will have to be done in the office,” says Dr. Sood-Mendiratta. “I think there’s a lot of potential for incorporating more telemedicine in ophthalmology, and this is a step in that direction.”
Ultimately, home tonometry can be a tool not only to improve glaucoma diagnosis and treatment, but also to help patients better manage their own care.
“With chronic conditions, anytime you have patients who are more involved in understanding their disease, they’re also more invested in following through with medications and complying with visits,” says Dr. Sood-Mendiratta. “Home tonometry is a way for patients with glaucoma to become more empowered in managing their disease.”
Image courtesy of iCare USA.
Advertisement
Advertisement
The drug does not provide lasting disease control for most patients
New service for patients with diabetes will make annual screening more convenient
Gonioscopy can help determine next steps in reducing IOP
Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
A review of pathophysiology, risk factors, clinical presentation and treatment options
How computational tools and personalized biomechanics can improve keratoconus detection, ectasia risk assessment and surgical outcomes
Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma
Registry data highlight visual gains in patients with legal blindness