A noninvasive approach to map eloquent areas before surgery
Cleveland Clinic epileptologists are advancing clinical care of epilepsy with transcranial magnetic stimulation (TMS) to perform cortical mapping prior to brain surgery. Their early experience with TMS for preoperative mapping of motor areas in two patients — one adult and one child — is being used to guide surgical decision-making in the context of upcoming patient management conferences. Both patients had previously undergone mapping with stereoelectroencephalography (SEEG), allowing comparison of the two techniques.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Our goal is to standardize our use of TMS for defining eloquent areas in patients we are evaluating for epilepsy surgery,” says Dileep Nair, MD, an epileptologist in Cleveland Clinic’s Epilepsy Center. “This tool offers important additional evidence not gained by other methods and fills a critical gap for infants and children, who often cannot be assessed with functional MRI.”
The gold standard of preoperative assessment for brain surgery is direct cortical stimulation with intracranial EEG, a method requiring craniotomy and implantation of electrodes to deliver electric pulses.
TMS has the important advantage of being entirely noninvasive. Electricity passes through a coil of wires, generating an electromagnetic field directed through the skull by a device held against the head (see Figure 1). Unlike an electric current, an electromagnetic field is unimpeded by the scalp, skull and cerebrospinal fluid, enabling stimulation pulses to be precisely delivered from an external source. When TMS is combined with a frameless stereotactic navigational system — so-called navigated TMS — highly accurate pulses can be delivered with imaging guidance (Figure 2).
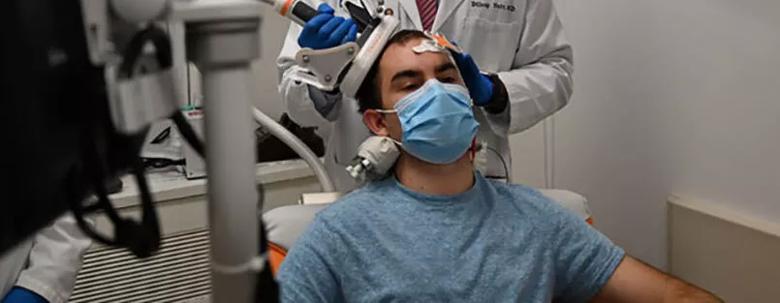
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/a856973b-424f-4e2c-8234-2708df2caae5/20-NEU-1915483-Navigated-TMS-to-guide-management-of-refractory-epilepsy_CQD-inset_805x313-2_jpg)
Figure 1. A candidate for epilepsy surgery undergoes navigated TMS for cortical mapping. A figure-of-eight coil is placed over the patient’s scalp, activating various parts of the brain to allow mapping of specific brain functions such as motor function and language. The resulting data are used to inform various types of brain surgeries, including epilepsy and brain tumor surgery.
Advertisement
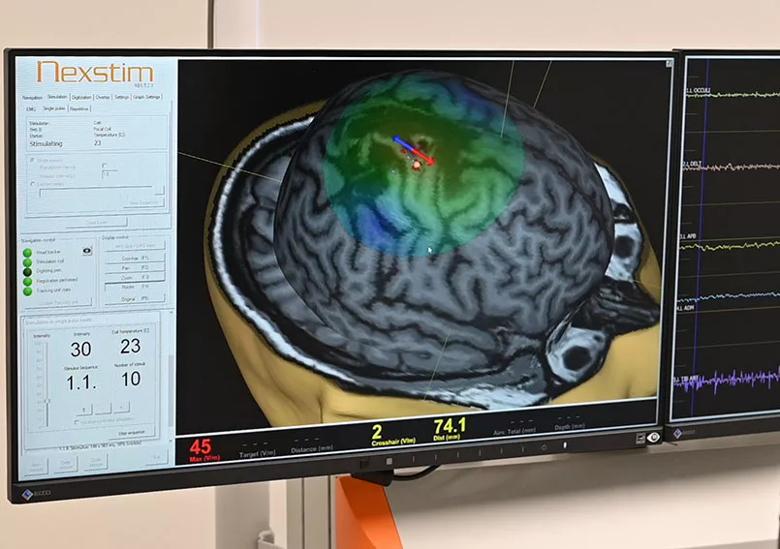
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d75071b4-4954-44eb-a8e5-d8dd4e6ad6c4/20-NEU-1915483-Navigated-TMS-to-guide-management-of-refractory-epilepsy_CQD-inset_805x567_jpg)
Figure 2. Monitor display during a TMS mapping session. The red-blue arrow indicates where the electric field is induced in the brain, with the colored area showing the extent of the electromagnetic field. Dots indicate the various stimulation sites, which are color-coded according to strength of response. EMG activity is simultaneously recorded to measure the strength of the motor evoked potential induced by TMS.
Functional MRI is currently the most commonly used noninvasive method for cortical mapping. But unlike structural MRI, which can be performed under sedation, functional MRI requires patients to be awake and lie very still for long periods so that motor and language functions can be assessed. This makes it impractical for infants and young children and may pose challenges for adults who are claustrophobic or have difficulty lying still for long periods.
“We use our navigated TMS system while patients are fully awake,” says Dr. Nair. “That way we can watch for movements or changes in speech patterns while we stimulate various brain regions, guided by the patient’s structural MRI scan.” Notably, however, it does not require the degree of patient stillness demanded by functional MRI.
In addition to this advantage for pediatric patients, TMS is also a useful adjunctive modality for adults. Moreover, it can be used to assess patients facing surgery for a brain tumor that may be near an eloquent area.
A TMS mapping session takes about one to two hours and is usually scheduled as a half-day outpatient visit or added to an inpatient EEG session. The primary contraindication is the presence of a nonremovable metal-containing implant in the head, such as a cochlear implant, deep brain stimulator, responsive neurostimulation device or stent in the neck or brain.
Advertisement
Some patients experience mild local pain and headache after a TMS session, but these symptoms are transient.
Uses of TMS have been explored for the past two decades, with its first clinical use approved by the FDA in 2008 for treating major depression. Since then, it has been used to treat obsessive-compulsive disorder and other psychiatric conditions, movement disorders and migraine pain.
Unlike navigated TMS for cortical mapping, therapeutic TMS is conducted with low-frequency repetitive and sequential pulses of stimulation. This “rTMS” technique is being studied for use in epilepsy to abort ongoing epileptic activity. It may also have potential use in patients suffering from status epilepticus or other forms of drug-resistant epilepsy not amenable to surgery.
Navigated TMS can also be used to map connections between different parts of the brain. “Research into neural networks can contribute to our fundamental understanding of the brain,” says Dr. Nair. “It could ultimately lead to better evaluation of patients for neuromodulatory treatment for epilepsy, as well as for pain, depression and other psychiatric disorders.”
Clinical use of TMS for epilepsy is, as yet, offered at only a handful of centers nationwide. It is FDA-approved for use in epilepsy for preoperative mapping of both motor and language areas.
“TMS is an important addition to our armamentarium to care for patients with epilepsy,” Dr. Nair observes. “Having different avenues of presurgical assessment for brain surgery is critical for optimizing outcomes.”
Advertisement
Advertisement
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits