Studies indicate dramatic results when used topically with or without corticosteroids
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/145575b3-eda0-4dd5-b0ea-c6e9ec3a0622/eye-drops-doctor-1184281742)
Eye drops
One of the most common medications for hypertension also may treat corneal damage, able to reverse corneal scarring and restore vision — potentially even in patients with eye injuries and diseases that occurred years ago. Losartan, taken orally by patients to control blood pressure, has shown dramatic results when tested in topical form on rabbit corneas and, most recently, as eye drops in humans.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Refractive and corneal surgeon Steven E. Wilson, MD, Director of Corneal Research at Cleveland Clinic Cole Eye Institute, says his work with losartan is the most significant discovery of his 30-year career. Cole Eye Institute Chair Daniel F. Martin, MD, calls it one of the great achievements in corneal research at Cleveland Clinic, research that is currently funded by nine National Institutes of Health (NIH) R01 or Department of Defense grants.
“The first major finding to come out of my lab was our 1996 publication showing that injury to the corneal epithelium causes apoptosis in underlying keratocytes,” says Dr. Wilson. “That is still our No. 1 cited paper. Then, in many studies, with the first being in 2013, we showed that basement membrane regeneration helps prevent corneal scarring. Those studies were important, but the potential clinical impact of losartan — the benefit it could offer to millions of patients worldwide — makes our latest work the most significant.”
Research recently published by Dr. Wilson’s team has led Cleveland Clinic to pursue a patent (currently pending) on “topical drug treatment to prevent or reduce corneal scarring.” The patent will cover losartan as well as other drugs in the same class that also potentially may prevent or treat myofibroblast-related scarring in the cornea.
For three decades, Dr. Wilson’s lab has been funded by the NIH and/or Department of Defense to study corneal wound healing and explore drugs that inhibit corneal scarring after injury, refractive surgery or infection. Part of the work has involved studying how scar-causing myofibroblasts develop, a process driven by transforming growth factor (TGF) beta-1 and TGF beta-2. The TGF beta connection led Dr. Wilson to consider the hypertension drug losartan, an angiotensin-converting enzyme (ACE) II receptor antagonist, which is known to inhibit TGF beta signaling.
Advertisement
To perform the first study of losartan’s effects on corneal scarring fibrosis, Dr. Wilson’s team applied for funding from the U.S. Department of Defense.
“The Department of Defense was interested in our work because wartime injuries to the corneal endothelium, due to chemical agents or trauma, are not uncommon,” says Dr. Wilson.
The three-year grant resulted in two landmark studies.
In the first one, published in Experimental Eye Research in early 2022, researchers tested the use of losartan in rabbits after descemetorhexis, the surgical removal of an 8 mm patch of Descemet’s membrane and corneal endothelium. Rabbits received topical losartan (0.4 mg/mL, six times per day) or oral losartan (a dose far greater in mg/kg than humans take for hypertension treatment, three times per day). After one month, corneas treated with the topical drug were clearer. Scarring had begun to disappear in the periphery, and the clearing effects were moving toward the center of the cornea. The development of myofibroblasts had been stunted. These effects of topical losartan on scarring were expected to be even greater after several months of treatment.
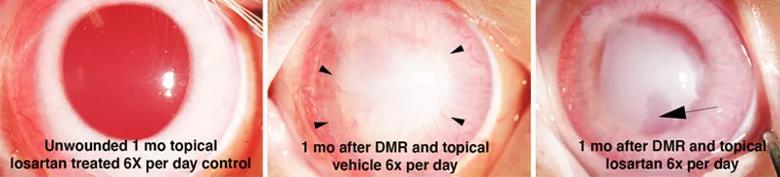
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f45f152b-4c74-426b-890e-2c23d44ecc02/22-EYE-3066210-CQD-Losartan-for-corneal-fibrosis-Wilson-inset2_jpg)
The first successful trial of topical losartan after removal of an 8 mm circle of Descemet’s membrane and endothelium (descemetorhexis, DMR). Left panel. An unwounded cornea treated topically six times per day with 0.4 mg/mL losartan for one month showed no signs of toxicity. Middle panel. A cornea that had descemetorhexis and then received topical vehicle six times per day for one month shows severe corneal scarring fibrosis extending into the periphery of the cornea and also corneal neovascularization (arrowheads). Right panel. A cornea that had descemetorhexis and then received topical 0.4 mg/mL losartan six times per day for only one month shows a markedly clearer peripheral cornea, along with a significant decrease in corneal neovascularization. An area of significant central stromal clearing (lacunae) is indicated by the arrow.
Advertisement
“The oral dose was far higher than what a human would use for hypertension, yet it had no effect on the cornea,” says Dr. Wilson. “Using oral and topical doses together also did not increase the effect of the topical dose. We think it’s because losartan’s oral route does not penetrate the cornea like the topical route does.”
This first study showed that even with epithelium at the front of the cornea intact, topical losartan can affect the entire cornea, all the way to the endothelium at the back. This is a critical finding, notes Dr. Wilson. While previous studies have suggested the scar-healing effects of antibodies to TGF beta, those and other substances will not penetrate a closed (healed) epithelium. As a result, their overall effect on scarring fibrosis is limited.
“It likely will take weeks to months of a continuous anti-TGF beta effect to see any meaningful reduction of fibrosis in humans,” says Dr. Wilson.
In the second study, published this summer in Translational Vision Science & Technology, the team evaluated the use of topical losartan and corticosteroid to heal rabbit corneas from alkali burn injuries to the epithelium, stroma and endothelium. Compared to corneas treated with losartan (0.8 mg/mL, six times per day) or corticosteroid alone, those treated with both medications had significantly decreased opacity and fewer myofibroblasts in the stroma after one month of treatment.
A third study (publication pending), supported by Research to Prevent Blindness funding, evaluated the use of topical losartan (0.8 mg/mL, six times per day) to treat late haze after photorefractive keratectomy. Again, the team found decreased corneal opacity and fewer myofibroblasts in the stroma after one month.
Advertisement
All three of these recent studies showed that topical losartan decreased the production of myofibroblasts, the main type of cell responsible for corneal opacity after injury or infection. While all three studies involved applying losartan preventatively, at the same time as the model injury, Dr. Wilson believes topical losartan can have similar success on any scarring caused by myofibroblasts, no matter how longstanding.
“The development of myofibroblasts is a dynamic process,” he says. “The cells are constantly dying and dividing, relying on a continuous supply of TGF beta-1 or -2 or both. If we interfere with TGF beta signaling, even if the corneal injury occurred months or years ago, myofibroblasts will likely undergo apoptosis. In their place, normal corneal cells — keratocytes and corneal fibroblasts — will move into the damaged tissue and restore the cornea’s transparency.”
Earlier this year, in Brazil, physicians that trained as Dr. Wilson’s fellows at Cleveland Clinic and University of Washington put that theory to the test. They created a topical losartan solution for off-label use in patients (which is allowed in Brazil if the medication is approved for oral use).
One patient with a free cap after LASIK surgery had developed severe diffuse lamellar keratitis, resulting in severe scarring fibrosis that limited vision to 20/200. Within five months of treatment with the losartan eye drops at 0.8 mg/mL six times per day, the patient’s cornea had returned to total transparency and the patient’s vision was 20/30.
Advertisement
A second patient with scarring and neovascularization developing years after radial keratotomy saw a dramatic decrease in fibrosis just 15 days after beginning use of losartan eye drops. The patient is continuing use of losartan, and further improvement is being noted.
Most recently, the physicians have begun using topical losartan in patients with recurrent herpes simplex keratitis.
While none of these cases has been published to date, early results are promising.
“The first two patients are far enough along that we know they have had dramatic clearing,” says Dr. Wilson. “In my experience, no other drug treatment has performed like this.”
Today, conventional treatment of corneal injuries involves topical corticosteroids. Corticosteroids may have a slight effect on scarring, but do not completely reverse it, says Dr. Wilson. And long-term use of corticosteroids is not without risk. Scarring that is reversed during short-term use may return when use is stopped.
However, according to the Wilson team’s study in Translational Vision Science & Technology, a combination of losartan and corticosteroid may be the most effective treatment for any infections, burns or other corneal scarring conditions with high levels of inflammation.
The team is taking a closer look at that thanks to a new three-year Department of Defense grant beginning this fall. They also will study the effect of topical losartan in different corneal injury models, in pre-existing injuries, in different treatment regimens and when combined with neovascularization-reducing drugs.
“Topical losartan likely can prevent or reverse scarring anywhere in the anterior segment of the eye, anywhere there are myofibroblasts, which cause the most severe, persistent types of scarring,” says Dr. Wilson. “That would include conjunctival fibrosis from etiologies like trachoma or scarring of conjunctival blebs after glaucoma surgery. If myofibroblasts are the cause of the scarring and the topical drug can reach the site of scarring, losartan is likely to be effective.”
Advertisement
The drug does not provide lasting disease control for most patients
New service for patients with diabetes will make annual screening more convenient
Gonioscopy can help determine next steps in reducing IOP
Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
A review of pathophysiology, risk factors, clinical presentation and treatment options
How computational tools and personalized biomechanics can improve keratoconus detection, ectasia risk assessment and surgical outcomes
Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma
Registry data highlight visual gains in patients with legal blindness