Patient able to avoid surgery and radiation despite having rapidly growing mass
A 72-year-old woman with a history of small skin cancers presented with a rapidly enlarging, painful mass on her right shoulder. A biopsy confirmed squamous cell carcinoma, and imaging demonstrated right axillary adenopathy. She was evaluated for surgical resection, which would have required likely flap and axillary nodal dissection, followed by radiation therapy. Instead, her medical team chose to treat her immediately with immunotherapy, and she had a remarkable response within days of receiving her first dose.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The patient had several smaller skin cancers removed over the past five years. In late 2022, she noticed a small nodule as well as several lesions on the back of her neck, and planned to discuss this with her dermatology physician’s assistant at Cleveland Clinic’s Richard E. Jacobs Health Center in Avon, OH at her regularly scheduled checkup.
The nodule began growing quickly, and upon examination, the physician’s assistant knew immediately that this was different from the previous instances of skin cancer. The physical exam and subsequent PET scan revealed a 3.1-centimeter subcutaneous mass as well as axillary hypermetabolic adenopathy compatible with metastatic disease. The physician’s assistant biopsied the area, and immediately called the multidisciplinary tumor board for non-melanoma skin cancer at Cleveland Clinic’s Taussig Cancer Institute.
Often in skin cancer cases, a medical oncologist may not see the patient until they’ve had surgery, but in cases of advanced cutaneous squamous cell cancer, it’s essential for all medical specialists — including medical oncology, dermatologists, surgeons and radiation oncologists — to be involved up front in determining treatment and management, explains Jessica Geiger, MD, the treating medical oncologist at Taussig Cancer Center.
“Even before we had seen the patient, we were consulting with one another about treatment options to expedite the best care as quickly as possible,” says Dr. Geiger. Within less than two weeks of the initial referral, the patient saw her new multidisciplinary team, who worked together to come up with the most effective course of treatment.
Advertisement
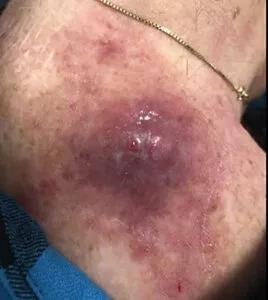
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2e8386e6-4665-462e-87ba-6302457901ee/23-CNR-3809431-CQD-Inset-3-800x895-1-268x300_jpg)
Lesion at the time of initial oncology consult
Surgical resection is the standard of care for advanced cutaneous squamous cell carcinoma, but it would have been a major undertaking in this case. “By this point, resection would have involved extensive primary surgery to the right shoulder tumor, as well a complete axillary lymph node dissection given nodal metastatic disease, similar to what is performed for breast cancer, and that can come with a lot of pain, issues with range of motion/movement, as well as potentially lifelong struggles with lymphedema,” says Dr. Geiger. “Additionally, with the rate of speed the lesion was growing, it didn’t make sense to wait to get on the operating room schedule, not to mention the additional time the patient have to wait to heal after surgery before starting radiation.”
Certain phenotypes of skin cancer are likely to respond very well to immunotherapy, and that was the case with this patient. The lesion was fast growing, poorly differentiated histology, and was accompanied by pain and inflammation. Those characteristics made it highly likely immunotherapy would be effective. Additionally, recent research bolstered the team in considering this approach.
In a phase 2 clinical trial recently published in the New England Journal of Medicine, 51% of patients with advanced cutaneous squamous cell carcinoma achieved a pathologic complete response and 13% had a major pathologic response (defined as </= 10% tumor viability) after receiving four cycles of the immunotherapy cemiplimab. “In this case, the patient was technically resectable from the start, but that resection would have been very extensive, would require further reconstruction, and the patient would still be facing radiation to a functionally sensitive area, so the team felt giving immunotherapy was a good option to potentially avoid surgery and radiation altogether while maintaining an excellent outcome and prognosis,” explains Dr. Geiger.
Advertisement
Immunotherapy was not without its risks. Though most patients tolerate it well with few side effects, immune-related toxicities may occur. Patients also need to be monitored extremely closely to ensure the disease isn’t progressing, as this could put them at risk of losing the window of resectability. “I like to see patients personally with every cycle to clinically evaluate them, at least initially, to ensure response to therapy and obtain photos,” says Dr. Geiger. “CT scans are also utilized to objectively assess response and are typically done every third or fourth cycle.”
Dr. Geiger explained the pros and cons of treatment options with the patient, who decided to proceed with immunotherapy. She quickly started a regimen of cemiplimab, which she receives as a 30-minute infusion every three weeks.
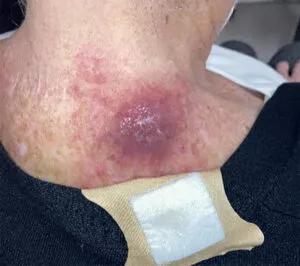
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/52401912-3a88-4ee8-aabe-2fec72d12ec5/23-CNR-3809431-CQD-Inset-2-800x710-1-300x266_jpg)
Skin cancer lesion
The patient received her first dose of immunotherapy on September 27, 2022. By the time she returned three weeks later for her second cycle, there was evidence of dramatic response to therapy. CT scans in the following months showed the lesion and lymph node continue to shrink substantially.
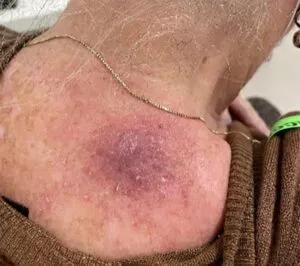
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7ca8609b-a197-4db6-a6a6-5f26c642beda/23-CNR-3809431-CQD-Inset-1-800x710-1-300x266_jpg)
Lesion on day 1 of C2 cemiplimab
Now in her 10th cycle, the patient is doing extremely well. She has had no side effects, and continues to work full time. She continues to show response to therapy on imaging, as her skin lesion is almost completely gone. She has had a near complete response on imaging, and will continue immunotherapy for 1-2 years, depending on imaging and clinical course.
Advertisement
Advertisement

Pembrolizumab does not improve outcomes, but immunotherapy may still offer benefit

Major study demonstrates importance of having a multidisciplinary approach to treatment for large, locally advanced tumors

Identifying candidates for further screening and treatment

Satellitosis or in-transit metastasis is a rare yet significant risk factor for this skin cancer that should be reflected in clinical staging systems.
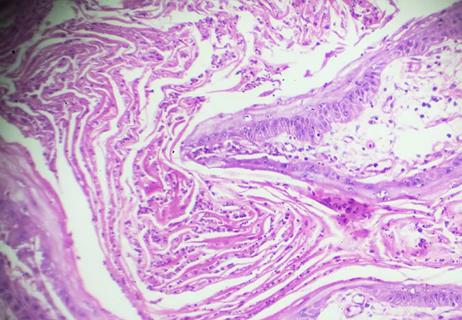
Majority of patients achieve complete pathologic response after four-dose cemiplimab therapy

Phase 2 trials investigate sitagliptin and methimazole as adjuvant therapies

Why Cleveland Clinic is launching its cardioimmunology center

Collaborative patient care, advanced imaging techniques support safer immunotherapy management