Results of a national database analysis of 1.5 million inpatients with AAA
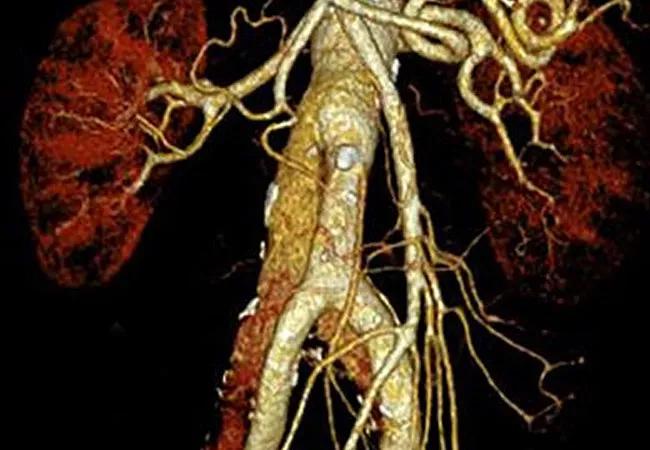
Antiplatelet therapy is associated with a significantly lower risk of developing an abdominal aortic aneurysm and reduces the likelihood of abdominal aortic dissection and rupture. So suggests an analysis of data from the U.S. National Inpatient Sample conducted by Cleveland Clinic researchers. The observational findings were described in a recent letter in the Journal of the American College of Cardiology.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Our investigation suggests that drugs that suppress platelet activity protect against the development and progression of abdominal aortic aneurysms,” says the study’s senior and corresponding author, Scott Cameron, MD, PhD, Associate Section Head for Research in Cleveland Clinic’s Section of Vascular Medicine. “The findings have important implications for a potential role of antiplatelet therapy in the condition.”
Abdominal aortic aneurysms (AAAs) often contain a nonocclusive thrombus in the lumen of the aneurysmal sac that consists of fibrin, inflammatory cells, platelets and red blood cells, as described in a recent review article by Dr. Cameron (Blood. 2018;132:2619-2628).
Prior research suggests that AAAs are associated with enhanced platelet reactivity, ramping up the synthesis and secretion of enzymes that injure and remodel the aorta. This remodeling may play an important role in aortic dissection and rupture. But whether trying to shrink the intraluminal thrombus with antiplatelet therapies would benefit patients has not been proven — and it may, in fact, cause harm instead by destabilizing the aneurysm.
This study analyzed the U.S. National Inpatient Sample, the largest publicly available inpatient healthcare database in the U.S. Out of more than 245 million hospitalizations between 2009 and 2016, the researchers identified the following groups:
Advertisement
Multivariate regression analysis was used to evaluate whether long-term and current antiplatelet medication use was protective against AAA development, dissection and rupture. The regression model included 26 variables, including age, sex, tobacco use, obesity and a variety of comorbid conditions as well as hospital characteristics.
They found that the use of antiplatelet agents was associated with the following outcomes:
No similar protective effects were observed for patients taking long-term anticoagulants.
Dr. Cameron points out that the study is limited in that it depends on accurate coding (including for over-the-counter drugs, such as aspirin) and that individual antiplatelet classes could not be analyzed separately. He also notes that although the results suggest that antiplatelet therapy may be useful for patients after an acute aortic event, this population is not represented in the database, as antiplatelet therapy is contraindicated following aortic dissection or rupture.
“Current guidelines recommend screening for abdominal aortic aneurysm for at-risk patients followed by surgical or endovascular repair if the infrarenal aorta reaches a certain size,” comments Cleveland Clinic’s Chair of Vascular Surgery Sean Lyden, MD, a co-author of the study. “Our findings suggest that antiplatelet drugs may play a protective role during that ‘wait and see’ period.”
Advertisement
According to Dr. Cameron, the research “provides more evidence of a link between enhanced platelet reactivity and harmful remodeling of the aorta.” He adds that future studies should further evaluate the role of circulating platelets in aneurysmal disease, with an eye toward characterizing the impacts of different classes of antiplatelet drugs.
“Aspirin blocks cyclo-oxygenase, whereas other antiplatelet agents block different receptors,” he explains. “Evaluating their possible role — individually and in various combinations — should be the focus of future investigation for determining safe and effective therapy.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more