Large study takes on a nuanced strategy question for the first time
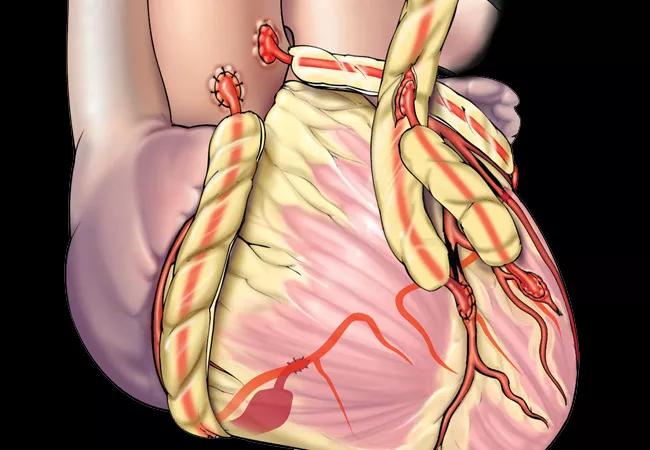
Survival following coronary artery bypass graft surgery (CABG) using bilateral internal thoracic artery (ITA) grafts is substantially influenced by the proportion of total myocardial mass perfused by the targeted vessels, a new Cleveland Clinic study finds.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Our findings support the use of a bilateral ITA approach that maximizes the myocardium supplied by the ITAs and steers clear of less-important targets,” says Cleveland Clinic cardiothoracic surgeon Faisal Bakaeen, MD, lead author of the large retrospective analysis, which was published in the Journal of the American College of Cardiology (JACC) (2020;75:258-268).
Whereas a survival benefit is well established for use of an ITA versus a saphenous vein bypass to the left anterior descending coronary artery (LAD), strong evidence is lacking for use of a second ITA graft rather than a vein graft for non-LAD targets.
So Dr. Bakaeen and colleagues retrospectively reviewed all 6,127 patients who underwent bilateral ITA grafting at Cleveland Clinic from January 1972 to January 2011. Of this group, 2,551 patients received one ITA graft to the LAD and had an assessable preoperative coronary angiogram.
Among these patients, the researchers set out to determine the survival effect of grafting to a dominant LAD — defined as one wrapped around the left ventricular apex — as well as to non-LAD target vessels. They scrutinized the angiograms to categorize non-LAD targets on the basis of their terminal reach toward the apex, with targets having > 75% reach graded as important (n = 1,698) and targets with ≤ 75% reach graded as less important (n = 853).
Mean follow-up duration was 14 ± 8.7 years, and multivariate analysis was used to pinpoint risk factors for mortality over time.
Analysis showed that patients in whom less-important additional target vessels were used were more likely to have a dominant LAD than were patients with important target vessels (51% vs. 35%; P < 0.0001). Overall, 179 patients (7.0%) had a second ITA grafted to multiple targets, and 43% of these cases involved multiple important targets.
Advertisement
While unadjusted survival was not influenced by the importance of the second ITA target, multivariate analysis revealed that grafting a second ITA to multiple important non-LAD targets was associated with significantly improved long-term survival relative to using a second ITA to only one important target or to nonimportant targets (P = 0.005). In patients with a nondominant LAD, grafting a second ITA to a less-important vessel was associated with a higher risk of operative mortality relative to grafting to an important vessel (2.4% vs. 0.51%; P = 0.007).
Saphenous vein grafts had no effect on long-term survival among recipients of bilateral ITAs, regardless of target importance.
“In patients who receive bilateral ITA grafts, choosing an anatomically important vessel for the second ITA is associated with lower surgical mortality in patients with a nondominant LAD,” notes Dr. Bakaeen. “Additionally, bypassing multiple important target vessels is associated with improved long-term survival. I would think of it as a dose-response relationship between the mass of cardiac muscle supplied by the ITA and patient survival. The best survival is achieved when all important targets are bypassed with ITAs when possible.”
In their study report, he and his co-authors translate their findings to two takeaway practical recommendations for formulating a bilateral ITA strategy:
Advertisement
“Our findings suggest that objective methods for quantifying the share of total myocardium perfused by each potential arterial target may help optimize long-term outcomes of CABG,” Dr. Bakaeen concludes.
In an accompanying editorial in JACC, cardiac surgeons from Cedars-Sinai Medical Center and the Icahn School of Medicine at Mount Sinai salute the Cleveland Clinic authors for “providing a uniquely granular insight into the importance of target anatomy” in coronary bypass surgery.
They add that the study provides “an honest insight into some of the challenges involved in adopting a multiarterial revascularization strategy across a wider platform.” The long-term rewards of such a strategy, they conclude, are “best realized through an individualized approach to target selection by surgeons with proficiency in multiarterial revascularization.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more