First cases set the course for a full spectrum of intrauterine therapies
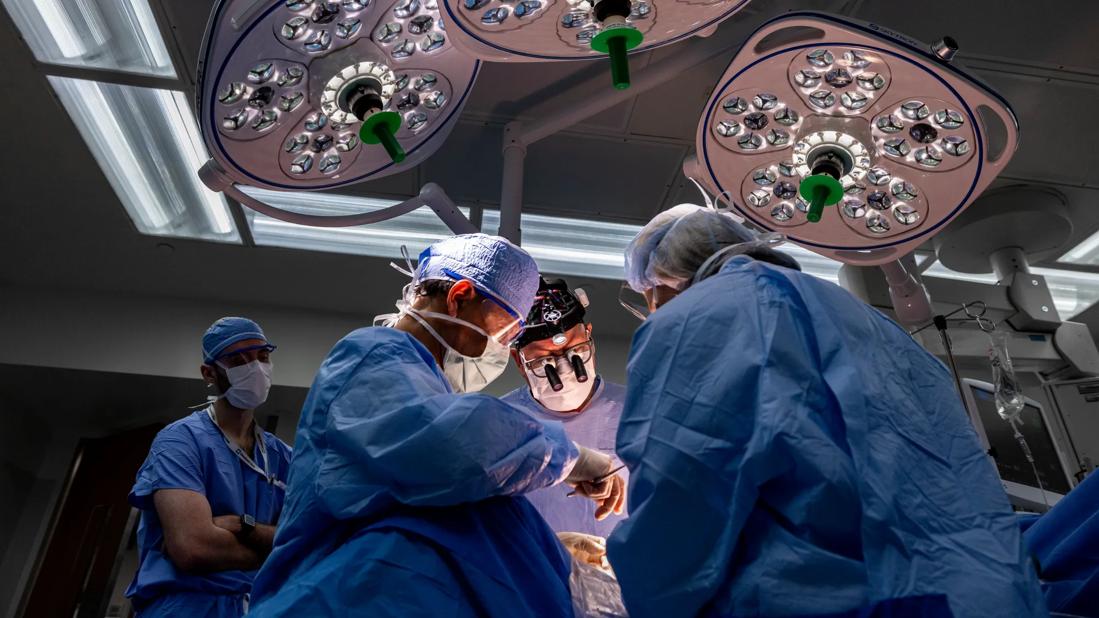
Led by one of the world’s most experienced fetal surgeons, Darrell Cass, MD, the first intrauterine myelomeningocele (MMC) repairs in Northern Ohio were performed at Cleveland Clinic.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
MMC, or open spina bifida, is the most common central nervous system congenital defect, occurring in approximately 1,645 births annually in the United States. The condition develops in the first four weeks after conception and is characterized by incomplete neural tube closure and a fluid-filled sac containing an exposed, extruded segment of spinal cord and nerves.
With the intrauterine surgical closure of their neural tube defects, these tiny patients’ Arnold-Chiari malformations have reversed, thus decreasing the risk for hydrocephalus and the need for shunting. The fourth MMC repair procedure was completed recently and caesarian delivery will be coordinated when the fetus is closer to term. Neurological evaluations are ongoing in the first two infants to determine their degree of motor functioning, which is expected generally to improve as a result of the fetal operations.
Historically, MMC lesions were surgically closed postnatally, limiting the prevention of neurologic loss. As prenatal diagnostic capabilities and technology (particularly ultrasonography and magnetic resonance imaging) improved, MMC could be detected and characterized as early as the first trimester, raising the prospect of fetal surgical repair.
“By successfully repairing [the defect] before birth, we are limiting the ongoing damage to the spinal cord from the intra-amniotic environment,” explains Dr. Cass. “In ultrasound studies of fetuses with spina bifida, we can witness them doing functions with their legs and ankles that are lost later in the pregnancy.”
Advertisement
In the first MMC procedure, Dr. Cass and Amanda Kalan, MD, used ultrasound to ensure the exact location and lie of the fetus within the uterus, ensuring that the uterine incision they were about to make was optimal to access the fetus’s MMC lesion while avoiding the placenta. Dr. Cass made a 4.5-centimeter uterine incision, using staples to control bleeding and infusing warm Ringer’s lactate to maintain uterine volume and fetal temperature. Pediatric neurosurgeons Kaine Onwuzulike, MD, PhD, and Violette Recinos, MD, then performed a multi-layer closure of the MMC lesion. They dissected the placode to release it from the arachnoid membrane, allowing it to retract into the spinal canal, then mobilized and sutured the dura, myofascia and skin. Drs. Cass and Kalan, closed the hysterotomy, replaced the uterus into the mother’s abdomen, and closed the laparotomy incision. Tocolytics were infused intravenously to suppress preterm labor.
These fetal surgeries were firsts for pediatric anesthesiologist Tara Hata, MD, who serves as the Pediatric Anesthesia Head for Fetal Surgery. “These cases are quite unique,” Dr. Hata says, “because you are really caring for and anesthetizing two patients — the mother and the fetus. One of the most important aspects of anesthetizing a pregnant woman is maintaining uterine blood flow.”
“We have all of this going on with the mother — who is under general anesthesia — but the fetus also needs to be completely immobilized,” Dr. Hata continues. “Many of the medications given to the mother do cross the placenta, providing some anesthesia to the fetus, but we also administer intramuscular injections to the fetus to ensure immobilization and provide additional pain relief.”
Advertisement
Throughout the procedures, Francine Erenberg, MD, a pediatric cardiologist, added a layer of safety through echocardiography. “In my practice, we tend to use fetal echocardiogram because of some suspected problem or genetic risk. In this case, we actually monitor the fetal heart rate mostly to check that the fetus is tolerating the procedure. As soon as the uterus is exposed, we begin continuous visualization of the fetus’s heart, watching for changes that might indicate that the stress of the surgery or medications are causing problems to the patient’s heart or circulation,” Dr. Erenberg says.
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/fbd07510-7a30-4a3a-8648-6de2a812a6dc/19-DDI-3810-fetalSurgery-163-CQD-800x550-2-300x206_jpg)
Drs. Erenberg and Hata monitor mother and fetus carefully, and recommend interventions, such as reintroduction of fluid to the uterus, administration of medications to accelerate the fetal heart rate or make adjustments to hemodynamic support for the mother.
To prepare for Cleveland Clinic’s initial fetal surgery efforts and the program’s eventual expansion in scope, Dr. Cass and members of the multidisciplinary team spoke with their counterparts and observed fetal surgeries at hospitals in Ann Arbor, Cincinnati and Denver.
Dr. Hata, along with McCallum Hoyt, MD, MBA, who serves as Head of Obstetric Anesthesia for Cleveland Clinic and is the Obstetric Anesthesia Head for Fetal Surgery, consulted with anesthesiologists in Boston, Cincinnati, Denver, Houston and San Francisco to compare their protocols and develop best practices. The two physicians are still in the process of making minor tweaks to a standardized Cleveland Clinic protocol based on their experience caring for these first four patients.
Advertisement
“We planned for these procedures for probably a year, with multiple simulations where we went into the operating room, talked through each step, including what we might find and what we might do and who would stand where. With more than two dozen people involved, this level of teamwork is essential,” Dr. Erenberg adds.
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/735f8a49-be65-42fd-94b9-ad8179ab1bce/DDSI-1497211_02-27-19_056_ST-300x200_jpg)
Cleveland Clinic Children’s Fetal Care Center is a collaborative team of highly skilled and compassionate healthcare professionals who offer state-of-the-art techniques and interventions with a family-centered approach. Families are first greeted by fetal care coordinators, who guide them through the process from referral through the postpartum period.
In these first MMC repairs, Carrie Budzar, BSN-RN, a fetal care coordinator, organized multidisciplinary appointments and scheduled any pre-op procedures. “As a fetal care coordinator, I monitor all referrals and connect them to team specialists based on what’s going on with their pregnancy. I spend a lot of time with the family making sure they meet all providers and are properly counseled,” Ms. Budzar explains. “Then, the evening before surgery, the entire surgical team meets with the family for a final discussion to make sure everyone is comfortable with and agrees to the plan of care. After surgery and discharge, I continue to work with the family to arrange follow-up care and, eventually, plan for delivery.”
Dr. Cass has high praise for his colleagues in the team’s first fetal surgery efforts together.
“It’s as good an outcome as we can see anywhere in the world,” he says. “Our anesthesiologists were the best I’ve worked with — cool and confident. Dr. Kalan and the others in maternal-fetal medicine are amazing to work with. Dr. Erenberg did a great job monitoring the baby to make sure nothing went wrong. The repair that our neurosurgeons did was the best I’ve seen, and it was brand new for them. And the nurses, care coordinators and operative team were incredibly dedicated, enthusiastic, well-prepared and attentive.”
Advertisement
The next steps are to prepare for additional and more complex cases, Dr. Cass says, and to make sure potential patients and referring physicians are aware that full-spectrum fetal surgery is now available in the region.
Advertisement

Benefits of neoadjuvant immunotherapy reflect emerging standard of care

Multidisciplinary framework ensures safe weight loss, prevents sarcopenia and enhances adherence

Study reveals key differences between antibiotics, but treatment decisions should still consider patient factors

Key points highlight the critical role of surveillance, as well as opportunities for further advancement in genetic counseling

Potentially cost-effective addition to standard GERD management in post-transplant patients

Findings could help clinicians make more informed decisions about medication recommendations

Insights from Dr. de Buck on his background, colorectal surgery and the future of IBD care

Retrospective analysis looks at data from more than 5000 patients across 40 years