
Lower extremity edema (swelling caused by fluid trapped in the body’s tissues) is present in about 20% of the population. Though often due to heart disease, it also can be caused by valve disease of the veins (venous insufficiency) and/or lymphatics (lymphedema).
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Once the lower extremities receive oxygen from the arteries, the veins return the blood back to the lungs to obtain the oxygen, and the lymphatics filter the blood of excess fluids and “toxins” to be eliminated. These systems function by way of valves. The muscles of the lower limbs also assist the valves by functioning as a pump, like the heart, to propel blood and fluid upward.
When the valves do not function properly, varicose veins and/or edema can occur, resulting in pain and heaviness in the limbs, especially at the end of the day. This tends to worsen over time and can result in skin discoloration, hardening or thinning of the skin, ulceration and infection. It can turn into a vicious cycle of more pain and less mobility, which further worsens the disease.
Common causes of nonfunctioning valves include hereditary predisposition, age, sitting or standing for prolonged periods of time (causing pressure on the valves from gravity), previous history of deep venous thrombosis (which can damage the valves), trauma, and limited mobility or gait disturbance.
Medical history and examination will lead to the diagnosis of venous insufficiency and lymphedema. A baseline venous ultrasound helps to exclude acute deep venous thrombosis and may show evidence of chronic post thrombotic changes.
The management of venous insufficiency and lymphedema involves daily maintenance and is geared towards assisting the valves, which helps symptoms and prevents complications. This involves three components:
There are no medications to treat the valves, and diuretics are usually not helpful or indicated. Surgery to close or remove the diseased veins may be indicated in very symptomatic patients with varicose veins or those with complications associated with venous disease. In these cases, a venous reflux study is needed to map out the incompetent venous valves for surgical planning. Highly specialized microsurgery can be done to bypass nonfunctioning lymphatics (lymph venous bypass) or transfer healthy lymphatics to the area of diseased lymphatics.
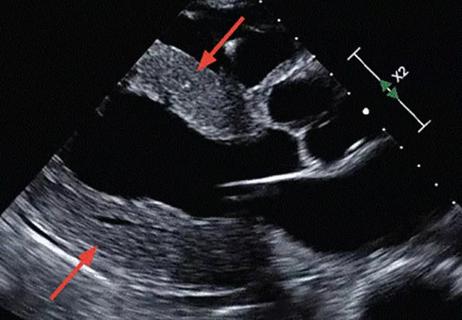
A case-based review of a condition more prevalent than once thought