
Development leader harnesses shared purpose to fuel meaningful giving

A multi-pronged strategy for tackling cancer access problems

State-of-the-art facility expands global care, professional opportunities

Nursing leaders share knowledge, ideas and experience
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Freely accessible LEADconnection.org is a one-stop shop for advice and more

Cleveland Clinic’s new Global Director of Vaccine Development outlines plans, priorities

Reforms aim to address escalating healthcare spending with new global care-delivery strategies

Health system expands global network of physicians and specialists
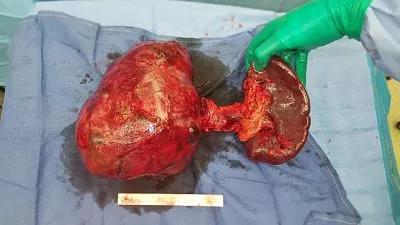
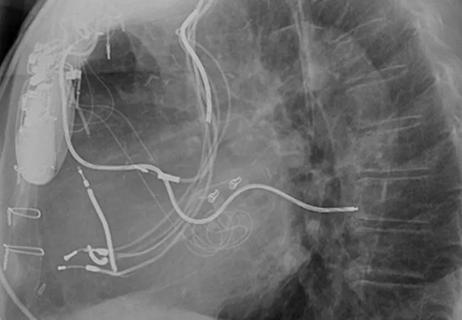
Seven-pound tumor requires complex, multidisciplinary care

Practice guidelines and key considerations
Advertisement
Advertisement