An overview of case reports and management
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Nonthrombotic pulmonary embolism (NTPE) is uncommon and can be difficult to diagnose. My colleagues and I recently reviewed this complete or partial occlusion of the pulmonary vasculature resulting from inorganic particulate matter and foreign bodies in Chest. The below images demonstrate accidental embolization from radiation seeds and vertebroplasty cement.
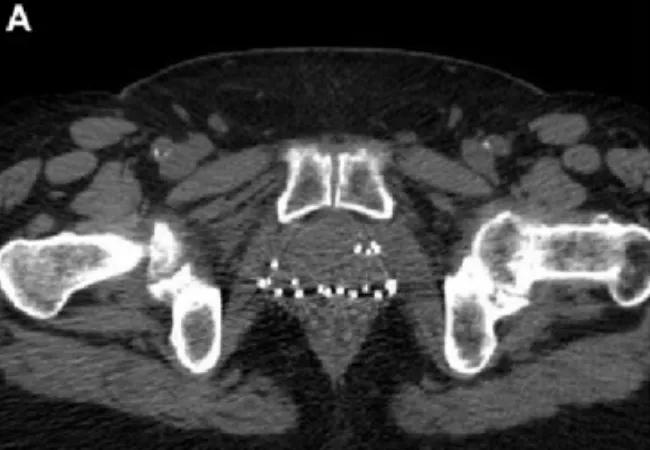
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7f483710-d5ff-4be2-b0fd-436c2bdb11e2/18-PUL-4794-Inset-Image-01-650pxl-width_jpg)
This image demonstrates the risk that brachytherapy seeds carry of embolization to the pulmonary artery. In the axial noncontrast pelvic CT at the level of the symphysis pubis, you can see numerous brachytherapy seeds embedded in the prostate. A transperineal approach to implantation carries a higher risk of embolization. An ultrasound-guided transrectal approach also carries this risk. Seeds implanted close to the periprostatic tissues or urethra migrate at a rate of 5.9-55 percent, and the rate of NTPE from distal embolization to the pulmonary vasculature ranges from 0-0.98 percent.
Note the multiple tiny embolized brachytherapy seeds in the right lung (arrows) on this postero-anterior chest radiograph (B), as well as the metallic density indicating an embolized brachytherapy seed in the right upper lobe on the axial CT at the level of the aortic arch (C).
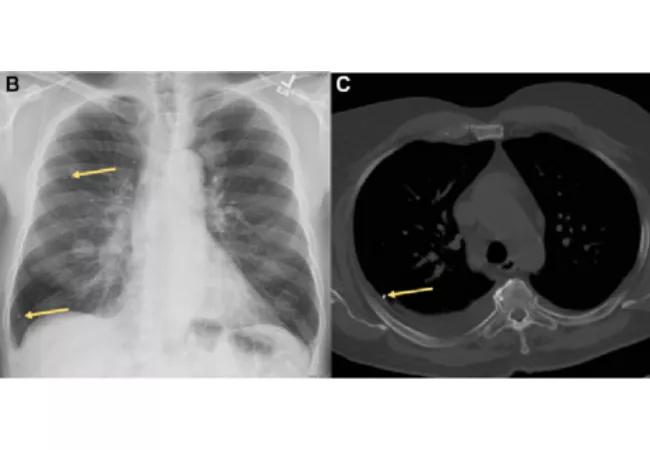
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b3a170ee-3c9d-4bc3-af96-8066085df39f/18-PUL-4794-Inset-Image-02-650pxl-width_jpg)
Fortunately, no mortality has been directly linked to these types of NTPE. Thus, current recommendations discourage the removal of embolized seeds because embolectomy is more dangerous than expectant management.
Percutaneous vertebroplasty using injection of polymethylmethacrylate (PMMA) into a collapsed vertebra is indicated for pain relief and mechanical strengthening. Venous extravasion occurs in approximately 24 percent of cases but only occasionally leads to life-threatening PE.
Advertisement
Note the PMMA cement within the thoracic vertebral body with embolization of similar attenuation material in subsegmental arteries (arrows) in the axial CT chest image (A). Coronal chest CT maximum intensity projection reconstruction shows radiopaque PMMA in multiple subsegmental pulmonary arteries. Note that use of bone windows increases diagnostic yield.
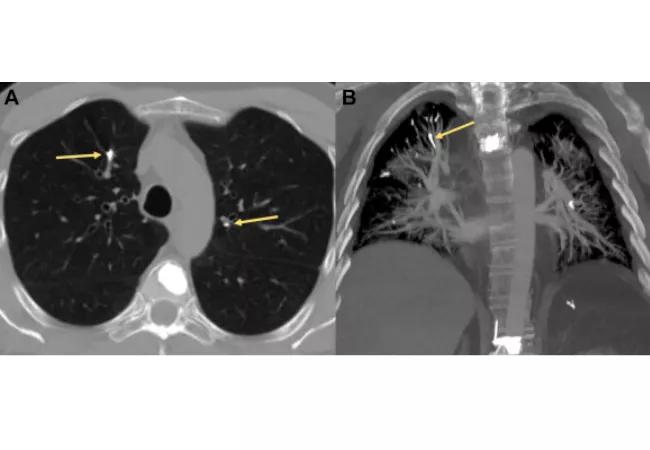
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/4e573d4b-1023-41ab-88ea-52c4f12b5d61/18-PUL-4794-Mehta-Inset-Image-03-650pxlwidth_jpg)
Many patients are asymptomatic, but others can present with many symptoms, from a chemical odor of PMMA to tachycardia and cardiopulmonary arrest. Management of these patients is currently unstandardized and ranges from conservative management to percutaneous retrieval and surgical embolectomy.
These are rare occurrences, and patients may present with a wide spectrum of signs and symptoms from none to severe. Accurate diagnosis requires extensive knowledge of imaging modalities and postprocessing tools. Future posts will review other macroscopic emboli like catheter tips and guidewires, microscopic emboli like ethiodized oil and silicone embolus, and talc granulomatosis.
Cleveland Clinic coauthors include Sanjay Mukhopadhyay, MD, staff, Department of Anatomic Pathology, Derick Asah, DO, resident, and Subha Ghosh, MD, staff, Department of Diagnostic Radiology.
Dr. Mehta is staff in the Department of Pulmonary Medicine.
Images and text republished with permissions from Elsevier. Originally published in Chest.
Advertisement
Advertisement
The Center for Environment, Place and Health Research connects clinicians with mapping tools and other real-world data resources to help guide medical insights
Exploring the true prevalence of AATD among Americans and why so many remain undetected
Rapid growth and collaboration have advanced the Lung Nodule Program, but patient engagement barriers persist
A physician's perspective on confirmation imaging, diagnostic confidence and choosing the right robotic platform for patients
A look into recent developments in the diagnosis of LAM and its clinical presentation
Takeaways from the most recent annual meeting centered around clinical advances, AI integration and professional development
Recent breakthroughs have brought attention to a previously overlooked condition
A review of treatment options for patients who may not qualify for surgery