Delay in treating fracture with entrapment can cause permanent double vision, other sequelae
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/323904b8-6973-465f-91fc-23ae6e8f5c9f/17-EYE-1421-Hwang-CQD-Hero_jpg)
17-EYE-1421-Hwang-CQD-Hero
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A 12-year-old boy with an orbital injury caused by jumping and hitting himself with his knee presented to an outside emergency department with complaints of double vision, left eye pain and nausea. Computed tomography scan of the orbit showed a left orbital floor fracture. The patient was discharged with a recommendation for outpatient ophthalmology follow-up.
Three days after the injury, the boy was evaluated by an outside ophthalmologist, who immediately sent him to Cleveland Clinic’s Cole Eye Institute. We saw him the same day. Although prior imaging studies were not available at the time, upon examination the patient still had double vision, restriction in upgaze and nausea.
These are all clinical signs of an entrapped muscle, a serious condition that can cause permanent double vision due to muscle ischemia. An entrapped muscle also can cause heart arrhythmias due to the oculocardiac reflex that places tension on a muscle, leading to bradycardia and, potentially, asystole.
Based on the clinical exam, we suspected an entrapped muscle and immediately brought the boy to the operating room, without waiting for imaging studies.
Intraoperatively, I identified the entrapped tissue within a trap-door orbital floor fracture. I successfully reduced the entrapped tissue with careful hand-over-hand technique, being vigilant not to injure any orbital tissues. After this, an absorbable implant, which would dissolve over the next few months, was placed over the fracture.
The patient initially had a stunned inferior rectus muscle, which resolved. At one-month follow-up, he showed no diplopia and no late sequelae with full extraocular motility.
Advertisement
Delay in treating fracture with entrapment can cause permanent double vision and other sequelae, including bradycardia and nausea through the oculocardiac reflex.
To prevent these sight- and life-threatening sequelae, it is vitally important for ophthalmologists — and emergency department physicians — to be keenly aware of the clinical signs of orbital entrapment when a patient presents with orbital injury. This is especially true in patients under the age of 15 because flexible pediatric bones are more likely to cause entrapment with trap-door fractures, as well as in patients with signs of restriction of extraocular motility and symptoms of double vision, nausea and bradycardia (oculocardiac reflex). These can be life-threatening as well as sight-threatening.
When patients such as this boy present in the emergency department, they should be evaluated by either ophthalmology or facial trauma experts, especially in the presence of complaints of nausea.
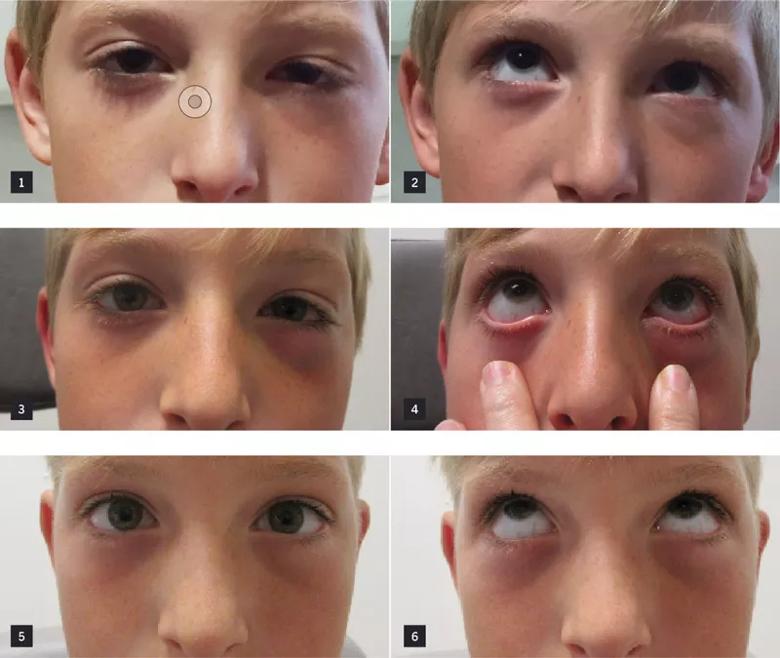
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/137b7ffc-1db3-47cc-9c1b-574964dc088e/17-EYE-1421-Hwang-CQD-inset_jpg)
Figures. The patient at presentation with stunned muscle with restriction in upgaze secondary to entrapment (Figures 1 and 2), one week postoperatively (Figures 3 and 4) and one month postoperatively (Figures 5 and 6). His restriction in upgaze resolved by one month postoperatively.
Dr. Hwang is an oculoplastic surgeon.
Advertisement
Advertisement
The drug does not provide lasting disease control for most patients
New service for patients with diabetes will make annual screening more convenient
Gonioscopy can help determine next steps in reducing IOP
Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
A review of pathophysiology, risk factors, clinical presentation and treatment options
How computational tools and personalized biomechanics can improve keratoconus detection, ectasia risk assessment and surgical outcomes
Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma
Registry data highlight visual gains in patients with legal blindness