Many amputations can be prevented
By Georgeanne Botek, DPM, and Gina Hild, DPM
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Diabetic foot disease is a leading cause of disability all over the world. Lower-extremity amputation (LEA) due to this condition greatly decreases quality of life and patient function, increases healthcare costs, and leads to increased mortality. Diabetes disproportionately accounts for the majority of LEAs, while peripheral arterial disease, infection and ulcerations are the leading underlying pathologies.
Up to one in four persons with diabetes mellitus develops foot ulcers. Of these cases, up to 24% result in LEA. However, many amputations can be prevented.
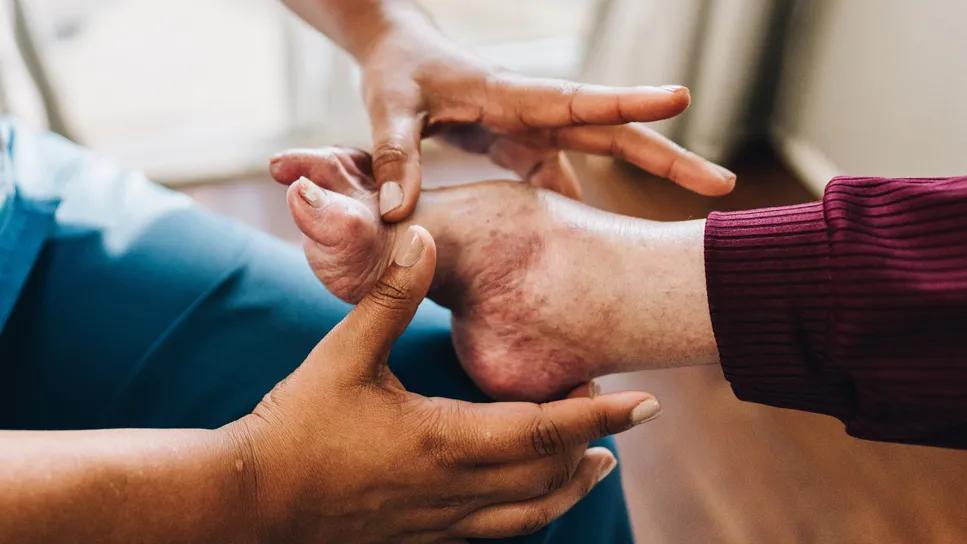
The multidisciplinary team within Cleveland Clinic’s Foot & Ankle Center — comprised of podiatric surgeons, vascular surgeons, orthopaedic surgeons, infectious disease specialists, physical therapists and orthotists — works collaboratively to address medical optimization, arterial perfusion and infection eradication in order to create a functional lower extremity. In the outpatient clinic, our team of podiatrists performs comprehensive foot evaluations for high-risk patients, screening for factors that could lead to diabetic foot complications. We endeavor to identify and curtail vascular disease early by:
A 62-year-old man presented to the emergency department after tripping over tubing on his vacuum-assisted closure device being worn for prior lower-extremity surgery. His past medical history included type 2 diabetes mellitus with peripheral neuropathy, mild peripheral arterial disease and stage 3 kidney disease. Several months prior, he underwent surgery for an infection in his posterior calf with subsequent latissimus dorsi muscle flap. This was complicated by a new dorsal medial foot ulceration, which was addressed with a medial column resection of his foot. Podiatry was consulted in the emergency department after he sustained a fall, which caused a subtle dorsal dislocation of his midfoot (Figures 1 and 2).
Advertisement
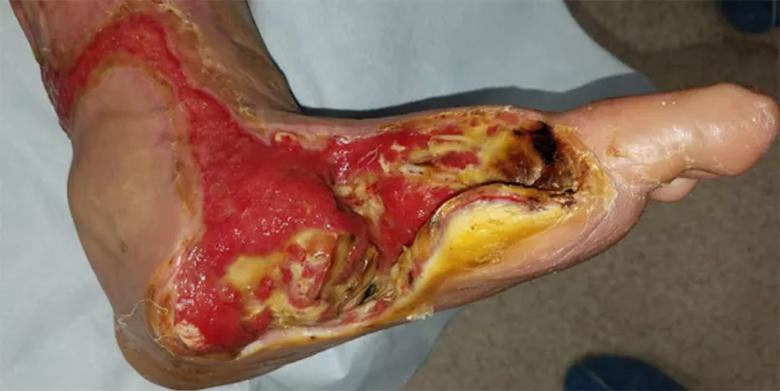
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d9f0280e-ce72-46de-8177-c2233a8cc45b/21-ORI-2415309-FIGURE-1_jpg)
Figure 1. Clinical photo of emergency department presentation with absence of medial column of foot.
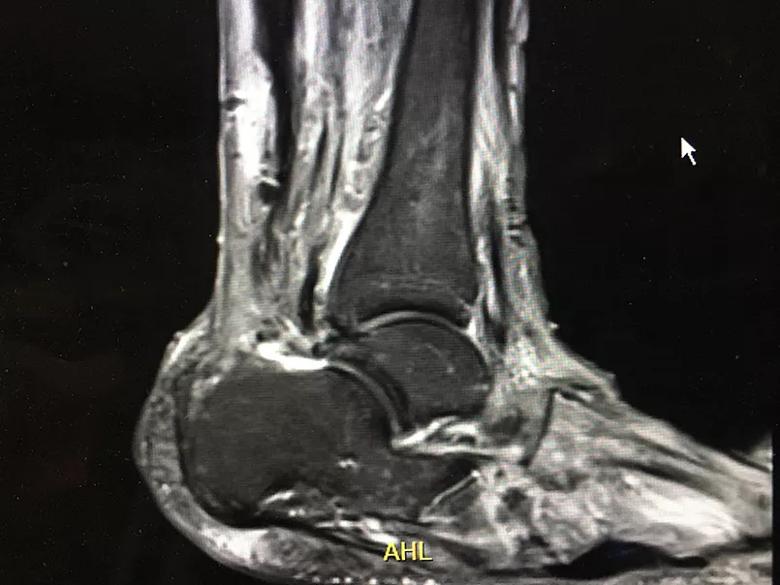
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c530975d-ff42-4774-8784-cbb098ef3154/21-ORI-2415309-FIGURE-7_jpg)
Figure 2. MRI findings compatible with osteomyelitis.
The patient insisted that he did not want to have his leg amputated as had been suggested by other surgeons. Long discussions ensued with the patient regarding the risks and benefits of a major LEA versus limb salvage, which would still involve surgical debridement of his large soft tissue defect and eradication of infection. He was approximately four months away from a major personal event, and he wanted to save as much of his lower extremity as possible and remain functional or mobile.
Noninvasive vascular testing was performed, which revealed potential satisfactory arterial circulation to heal a Chopart amputation (i.e., amputation of the forefoot and midfoot, leaving the talus and calcaneus). At this point, a staged surgical approach was decided. The first procedure was to debride the wound and remove the metatarsal bases, which were known to be infected. Cultures were obtained for targeted antibiotic treatment, and negative-pressure therapy was employed to determine flap and tissue viability (Figures 3 and 4).
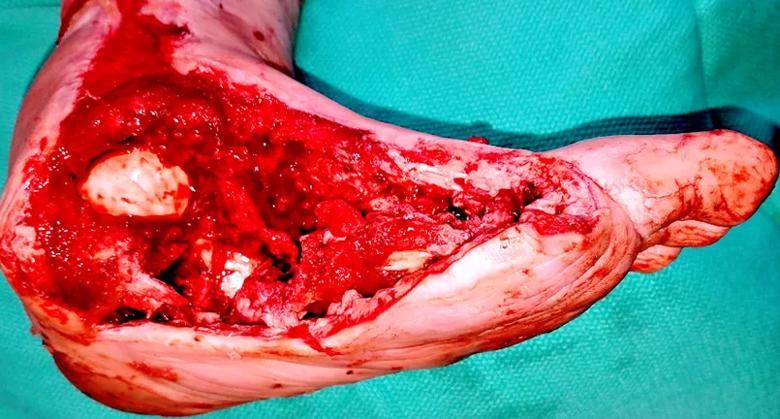
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3f497285-4640-4480-b157-6e19ed797b22/21-ORI-2415309-FIGURE-3_jpg)
Figure 3. After first surgical foot debridement. Staging has been shown to yield better outcomes in reaching a definitive amputation level without re-amputation or a higher level of amputation.
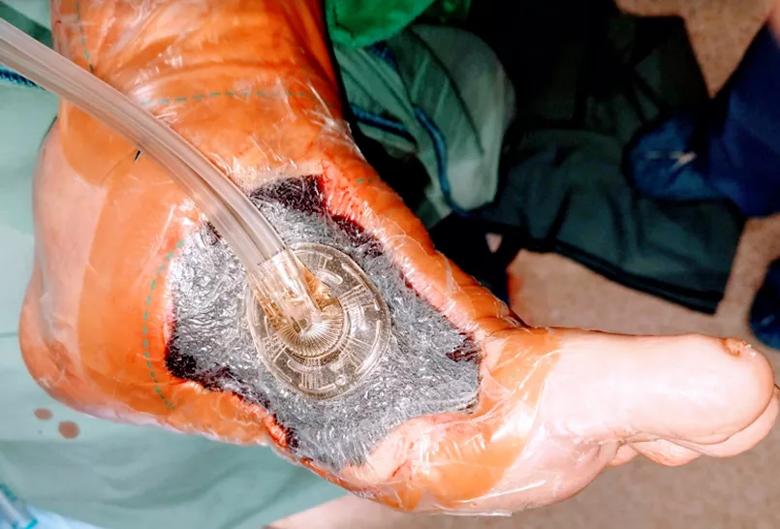
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/77b1b0f5-b0f2-47f8-bf6b-24b1dba64336/21-ORI-2415309-FIGURE-4_jpg)
Figure 4. Negative-pressure wound therapy after first foot debridement.
After 72 hours, the first dressing change was performed, and the remaining foot appeared viable. At that point, the podiatric surgical team proceeded with the definitive amputation level. The patient’s remaining midfoot and forefoot osseous structures were removed. Then a lateral plantar artery flap was brought from the lateral side of the foot to the medial side and was remodeled to fit the area (Figure 5).
Advertisement
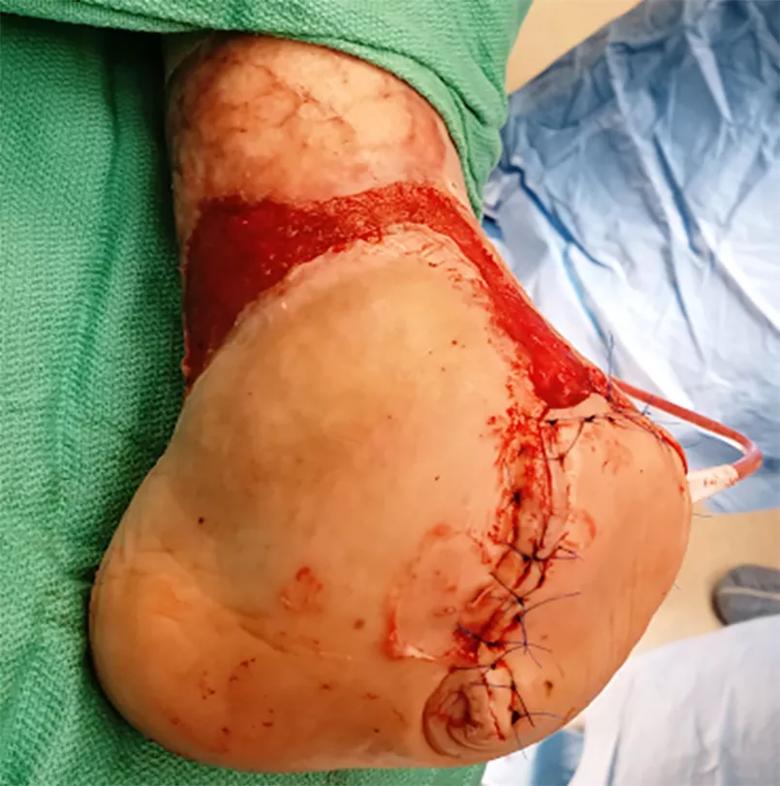
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/66676769-da7c-4161-a8ec-d187a6a25099/21-ORI-2415309-FIGURE-5_jpg)
Figure 5. Immediate post-op Chopart amputation.
Tendon balancing was performed in order to prevent an equinovarus deformity. Prior to closure, antibiotic beads with gentamicin and vancomycin were inserted. A drain was left in place for 48 hours in order to prevent hematoma or seroma.
A successful outcome ensued over the course of several months, with eradication of infection and primary closure of both the foot and prior ankle wounds. Advanced amniotic biologics were employed under the negative-pressure wound device at the time of the patient’s second surgical procedure. The patient is now three years post-op (Figure 6).
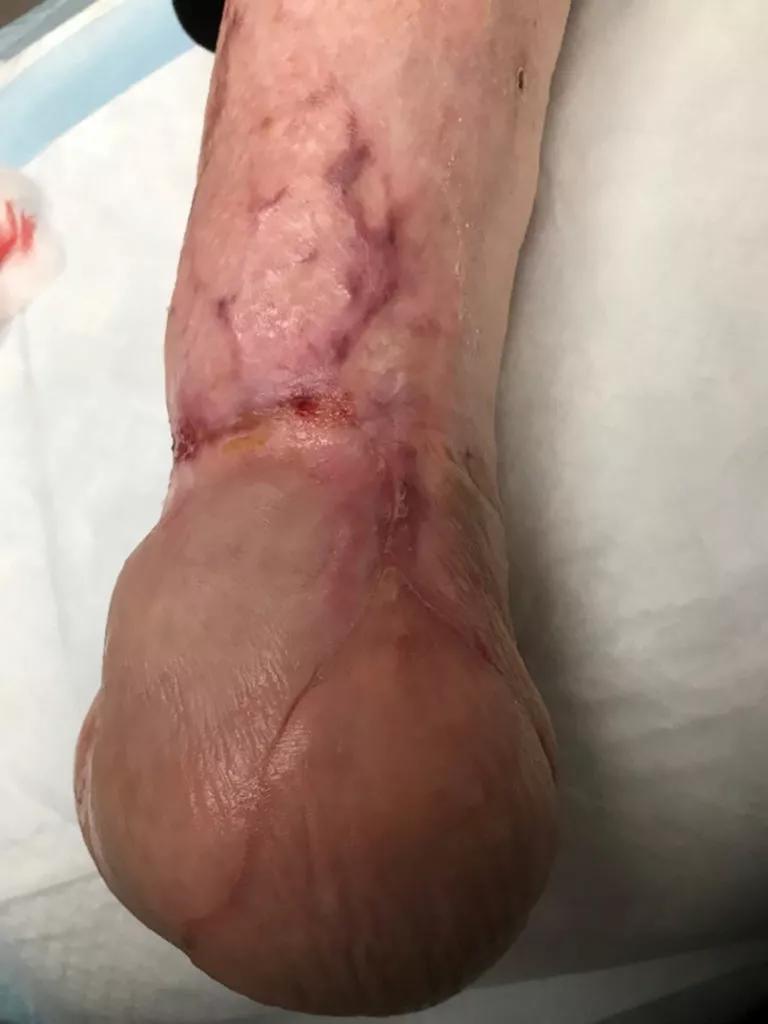
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c80dd1a8-625b-4b87-85cb-91081fc566ac/21-ORI-2415309-FIGURE-6-768x1024_jpg)
Figure 6. Status post-Chopart amputation with amniotic graft of ankle wounds.
For a functional, mobile extremity and to prevent future ulceration, multidisciplinary care is required. Patients are referred to physical therapy for gait training, and to orthotics for a custom brace or appropriate footwear.
Patients with a history of neuropathic or neuroischemic ulcerations are patients for life for the podiatrist and vascular specialist, respectively. To reduce the risk of re-ulceration and the potential for subsequent infection of the affected limb or the contralateral extremity, regular preventive visits are recommended.
With the diagnosis of diabetes mellitus at epidemic proportions, a functional limb preservation team is crucial to performing all roles necessary in caring for patients at high risk of foot ulceration and amputation.
Dr. Botek is Head of Podiatry within the Foot & Ankle Center and a founding member of Cleveland Clinic’s Functional Limb Preservation Council, a multidisciplinary group devoted to education, research and best practices involving the diabetic foot.
Advertisement
Dr. Hild is a podiatric surgeon specializing in limb salvage and general foot surgery in Cleveland Clinic’s Foot & Ankle Center.
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment