Cutaneous complications common post-transplant
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As lung transplant becomes more common, pulmonologists should be aware of post-transplant dermatologic complications. Early treatment for suspicious lesions is crucial, especially in this population. Patients with higher risk should be screened regularly and educated about the importance and of skin surveillance and proper application of UV protection. I urge any transplant pulmonologist to incorporate counseling, treatment, education and referral to dermatology into their post-transplant visits.
Here’s a roundup of our recent work on the pathogenesis, epidemiological characteristics and clinical manifestations of dermatologic complications found in lung transplant recipients.
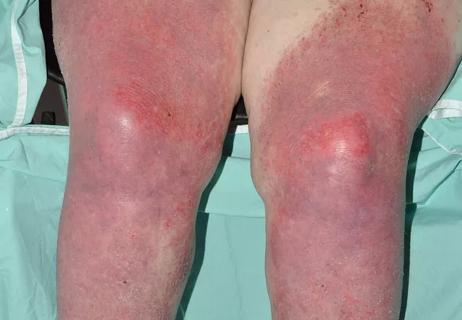
Actinic keratosis is caused by the abnormal proliferation of keratinocytes due to UV radiation. This premalignant skin lesion can potentially become squamous cell carcinoma (SCC). Classic actinic keratosis appears as large, scaly, thin, erythematous papules; hypertrophic actinic keratosis is thicker and sometimes manifests with cutaneous horns.
To see a cases of actinic keratosis in lung transplant patients, click here.
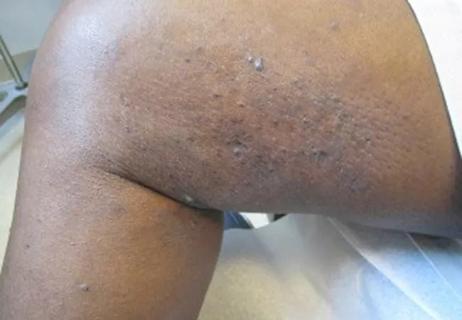
Because herpes viruses are lymphotrophic, they disseminate readily in immunocompromised patients. Other risk factors include seropositive transplant into a seronegative host, absence of or resistance to antiviral prophylaxis, reactivation of latent infection and confection of two herpes viruses.
To see cases of herpes virus in lung transplant patients, click here.
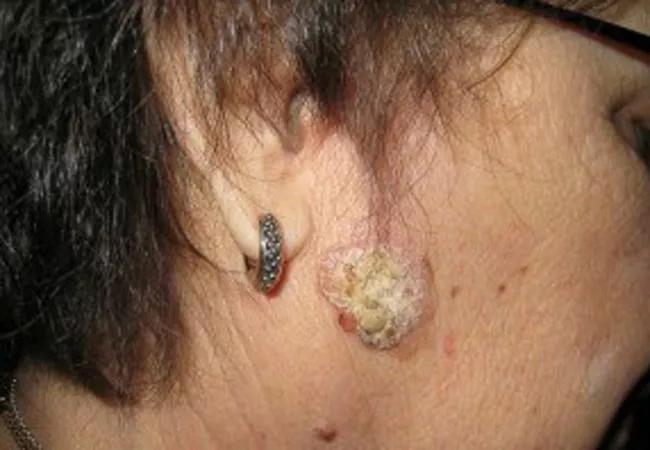
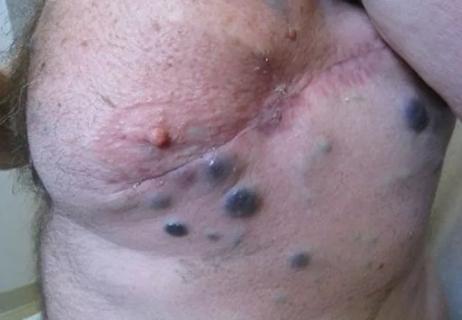
Kaposi sarcomas are endothelial cell tumors often but not always associated with human herpes virus (HHV)-8. Upon immunosuppression, especially with calcineurin inhibitors, HHV-8 can reactivate, proliferate and produce kaposi sarcoma. Viral transmission can also occur during transplant. KS can be disfiguring and cause lymphedema, pain and secondary infection.
Advertisement
To see a case of kaposi sarcoma in a lung transplant patient, click here.
Transplant recipients are at increased risk of developing malignant melanoma, and that risk increases with longer and more intense immunosuppression as well as male sex, age and azathioprine use. Melanoma can be transmitted from donor to recipient even after curative resection.
To see cases of malignant melanoma in lung transplant patients, click here.
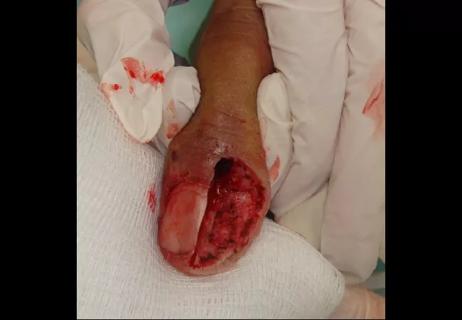
The incidence of SCC in solid organ transplant recipients is approximately 3.6 percent at 36 months and increases to 26.5 percent at 10 years post-transplant. The risk increases with age, time from transplant, prior skin cancer diagnosis and male sex. The use of immunosuppressants in transplant recipients increases the proliferation of oncogenic viruses and tumor promotion. There are several types of SCC, including Bowen disease, or SCC in situ, invasive SCCs (like the image above) and keratoacanthomas.
To see cases of SCC in lung transplant patients, click here.
Dr. Mehta is staff in the Department of Pulmonary Medicine.
Image republished with permission from CHEST.
Advertisement
Advertisement
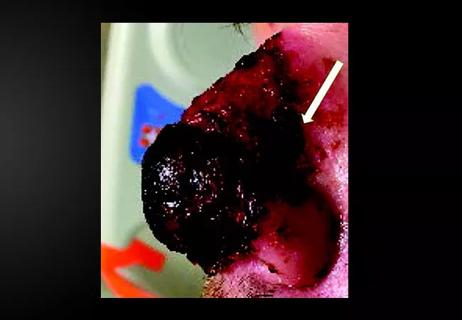
Stress and immunosuppression can trigger reactivation of latent virus
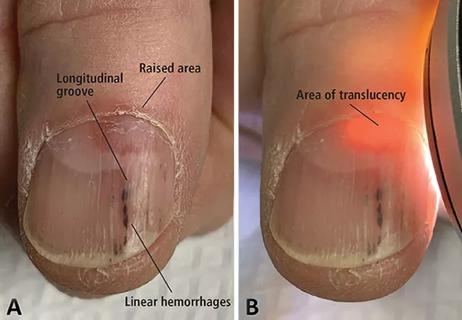
A case report of a thumbnail deformity
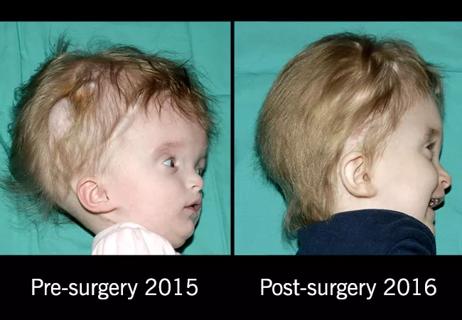
Multidisciplinary team of plastic surgeons and neurosurgeons correct severe, complex head deformity
Trials evaluate safety and efficacy of new treatments

Cutaneous complications common post-transplant
Cutaneous complications common post-transplant
Cutaneous complications common post-transplant
Two cases of a rare cancer of the sweat glands