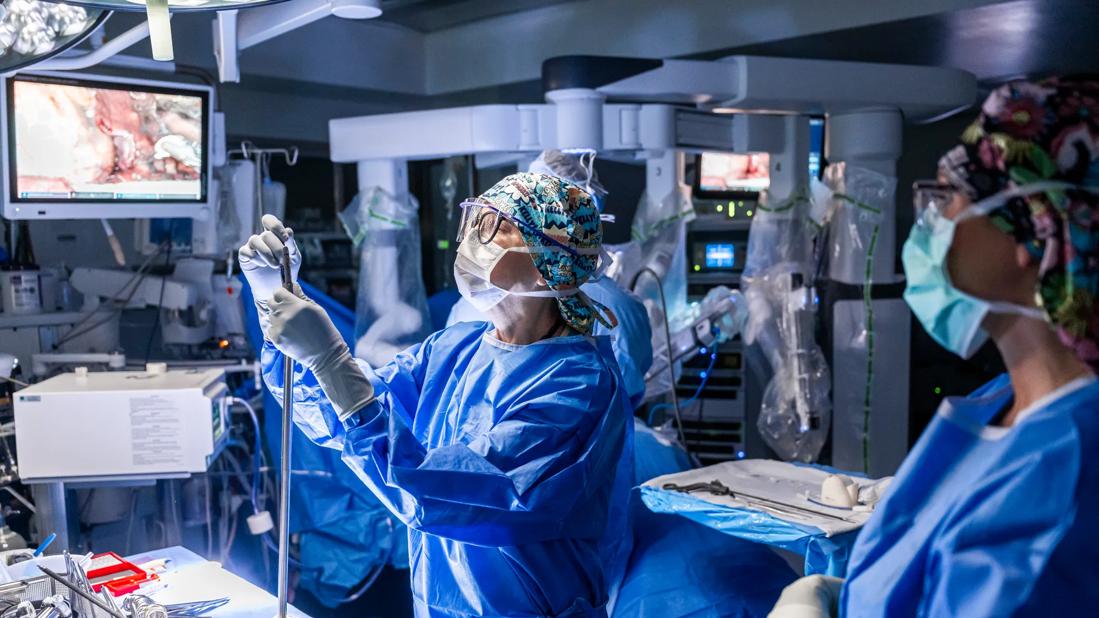
This November will mark 20 years since the FDA approved a robotic surgical system for use in mitral valve surgery. Today just over 100 centers in the United States offer robotic-assisted mitral valve repair, and only half perform 20 or more per year.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Despite two decades of accumulated experience with robotic mitral valve surgery, nationally only about 10% of these procedures are performed using robotics,” says cardiothoracic surgeon José Luis Navia, MD, Florida Regional Director of the Heart, Vascular, and Thoracic Institute for Cleveland Clinic. “That reflects the high degree of training and experience needed to offer this advanced approach.”
Earlier this year Dr. Navia performed the first robotic-assisted mitral valve repair at Cleveland Clinic Weston Hospital, a milestone that heralded the launch of southeast Florida’s first Robotic-Assisted Mitral Valve Surgery Program and the third such program for the state.
Studies have demonstrated that mitral valve repair for posterior leaflet prolapse, the most common cause of chronic primary mitral regurgitation, is a low-risk, durable surgical procedure. “Now we can offer all three major surgical approaches – robotic, minimally invasive, and open – based on what is most appropriate for each patient,” says Dr. Navia.
Traditional open-chested mitral valve surgery involves creating a 6- to 8-inch incision through the sternum and spreading the ribs to view the heart. Endoscopic mitral surgery with handheld instruments decreased the size of the incision to about 3 to 4 inches and may be performed with or without rib-spreading.
The robotically-assisted technique uses even smaller incisions, often less than 2 inches. With the robotic arms deployed in the right thorax, the procedure typically entails peripheral perfusion and aortic occlusion.
Advertisement
“During robotic mitral valve surgery, we can perform annuloplasty, leaflet resection, and artificial chordae tendineae implantation to repair the valve,” Dr. Navia explains. “In select cases, we can also perform robotically assisted tricuspid valve repair during the same surgery for patients who require multivalve repair.”
For patients, the benefits of less invasive surgery include lower risk of infection, less bleeding and trauma, a shorter hospital stay, faster recovery, and better cosmesis.
The Weston-based surgical team, under Dr. Navia’s leadership, received its robotic surgical training at Cleveland Clinic’s main campus in Ohio, home to the nation’s largest valve treatment program. Dr. Navia joined Cleveland Clinic Florida in 2019, after 20 years with the Cleveland Clinic Heart, Vascular & Thoracic Institute in Ohio, where he specialized in adult-acquired heart disease and minimally invasive cardiac surgery.
“I came with the intention of establishing a robotic-assisted mitral valve program in Florida, though COVID-19 impacted the timeline,” notes Dr. Navia, who first trained in robotic heart surgery in 2002.
Cleveland Clinic cardiothoracic surgeons have performed more than 2,000 robotic mitral valve repairs, demonstrating a high likelihood of valve repair and low operative mortality and morbidity. An analysis of Cleveland Clinic’s first 1000 cases, which was published in the January 2018 issue of the Journal of Thoracic and Cardiovascular Surgery, confirmed a repair rate of 99.5%, with an operative mortality rate of 0.1% and a stroke rate of 1.4%.
Advertisement
“The analysis was particularly compelling because it showed that a combination of algorithm-driven patient selection and increased experience improved outcomes,” Dr. Navia observes. He points out that the addition of routine CT scanning to detect peripheral artery disease or atherosclerosis, which would contraindicate femoral perfusion, reduced the stroke rate from 2% to just 0.8% in the second 500 patients.
According to Cleveland Clinic’s patient selection criteria, other contraindications for robotic-assisted surgery include aortic insufficiency, severe pulmonary hypertension, annular calcification, and poor ventricular function.
After coronary artery bypass, valve surgery is the second-most common heart surgery in the United States. Over 100,000 people had heart valve repair or replacement surgery in 2018, and the mitral valve is the most commonly repaired valve.
American College of Cardiology/American Heart Association Practice Guidelines for Management of Patients with Valvular Heart Disease recommend early surgery for patients with degenerative mitral valve disease if there is a high chance of successful repair and mortality risk is low. Yet, research reported on by the Society for Thoracic Surgeons indicates that many patients with mitral valve disease may have reached a chronic stage prior to referral for surgery.
“We know surgery works best when symptoms have not advanced too far,” asserts Dr. Navia. “In the case of mitral regurgitation, it can be curative if performed early enough to avoid irreversible heart and lung changes.”
Advertisement
Advertisement

Nonthermal technique reduces bleeding and perforation risk

Standardizing a minimally invasive approach for Barrett’s Esophagus and Esophageal Cancer

PSMA-targeted therapy for metastatic prostate cancer now offered at Cleveland Clinic Weston Hospital

Nationally recognized urologic oncologist offers vision for growth, innovation, and excellence

Noninvasive modality gains ground in United States for patients with early-to-moderate disease

Cleveland Clinic Weston Hospital’s collaborative model elevates care for complex lung diseases

Interventional pulmonologists at Cleveland Clinic Indian River Hospital use robotic technology to reach small peripheral lung nodules

Trained in the use of multiple focal therapies for prostate cancer, Dr. Jamil Syed recommends HIFU for certain patients with intermediate-risk prostate cancer, especially individuals with small, well-defined tumors localized to the lateral and posterior regions of the gland.