Head & neck surgeon and neurosurgeon perform complex endonasal procedure
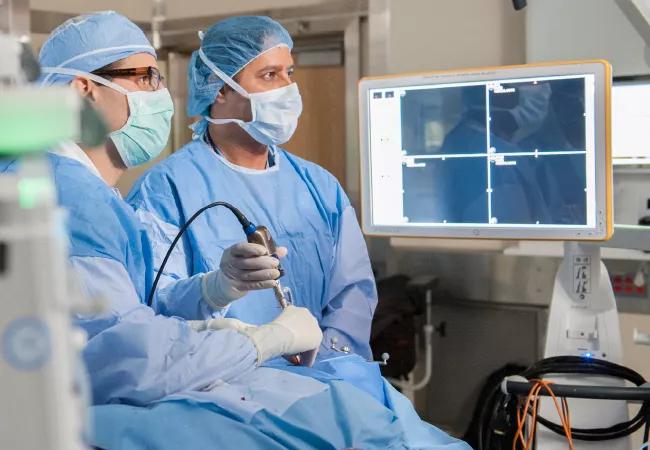
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0b1b0ecb-dc72-44b3-a830-521f24010bed/17-ENT-4469-Recinos-Hero-Image-650x450pxl_jpg)
17-ENT-4469-Recinos-Hero-Image-650x450pxl
Endoscopic sinus and skull base surgeon Raj Sindwani, MD, and neurosurgeon Pablo Recinos, MD, partner on complex endoscopic skull base surgeries that rely on a “two surgeons, four hands” simultaneous approach rather than the tag-team approach of traditional endonasal pituitary surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
These procedures have proliferated greatly since 2014 with the launch of Cleveland Clinic’s Minimally Invasive Cranial Base and Pituitary Surgery Program, a multidisciplinary collaboration between Cleveland Clinic’s Head & Neck Institute and the Neurological Institute’s Rose Ella Burkhardt Brain Tumor and Neuro-Oncology Center.
Given the success of the two-surgeon approach, the team now routinely employs its expertise for the management of other complex pathologies located in hard to reach areas of the head. Dr. Sindwani and Dr. Recinos recently used an endoscopic, endonasal approach for resection of an intraorbital/orbital apex l hemangioma for a patient who was having severe progressive vision loss due to the mass. This was a challenging procedure due to the deep location of the tumor within the intraconal space of the eye, and because of its close proximity to the optic nerve. They selected the safest endoscopic corridor to approach the tumor (between the inferior and medial rectus muscles) and removed the mass without any cuts or bruises. The patient’s vision was restored to normal.
See how the tumor was removed and learn more about the patient’s amazing outcome in this video showing step by step how the procedure was done.
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/q4RD0Dhm4L8?feature=oembed)
Advertisement
Advertisement
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits