
An update on the technology from the busiest Gamma Knife center in the Americas
Improvements enable targeting of brain tumors with single-session, fractionated or neoadjuvant approaches
New review published in Cancers suggests a synergistic benefit
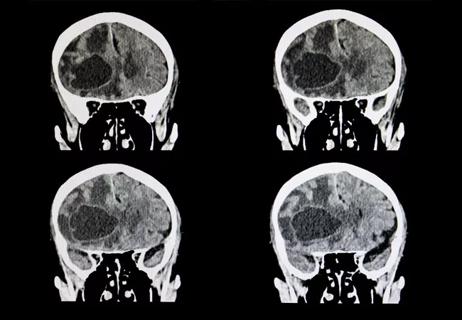
This approach led to local control for patients with brain metastases more than 2 cm in diameter
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
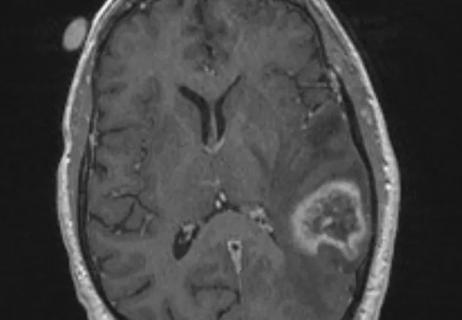
We now have an expanded toolbox to extend survival and lessen treatment toxicity
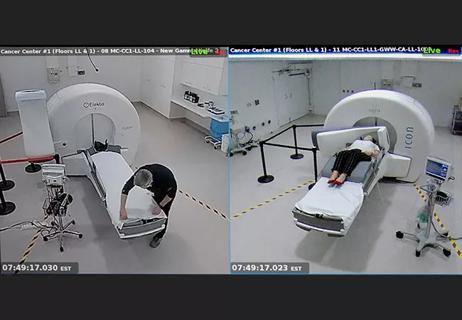
Two stereotactic radiosurgery experts take stock after Cleveland Clinic’s 10,000th case
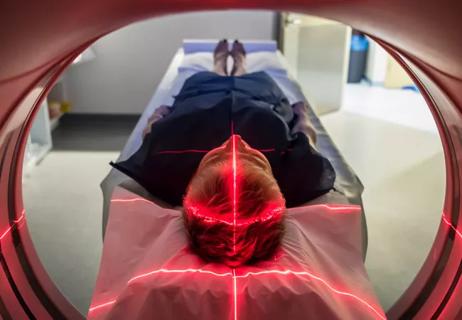
Study presented at ASTRO 2021 shows promise in patients treated with stereotactic radiosurgery

Why it remains the mainstay for newly diagnosed metastases and tumors

Number of brain metastases doesn’t matter for ALK/EGFR+ patients
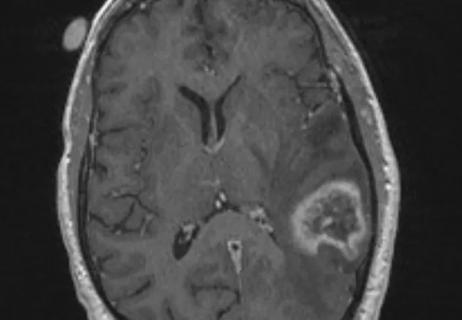
Dose-escalation trial shows local control with low toxicity, low leptomeningeal recurrence
Advertisement
Advertisement