Growth modulation procedures are effective if the condition is diagnosed before the patient reaches skeletal maturity
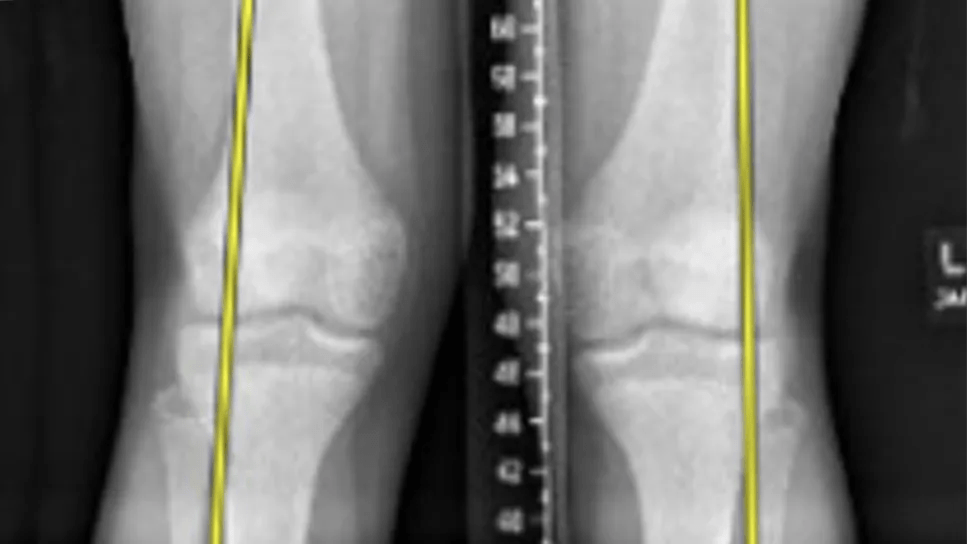
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3edf1c5b-0f1e-440e-b0dc-6b216f1a5557/Genu-valgum-feature)
X-ray of patient with knock knees
By Conner Paez, MD, and David Gurd, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Genu valgum (knock knees) represents one of the most common angular deformities encountered by pediatric orthopaedic specialists. In patients ages 2-7, genu valgum is typically physiologic, with a peak valgus angulation around ages 3-4. After age 7, genu valgum is considered abnormal.
Underlying causes of the pathologic form of genu valgum include:
However, the vast majority of cases are idiopathic.
Genu valgum is a concern for all orthopaedic specialists, not just pediatric specialists. The condition and its treatment outcomes can impact other orthopaedic conditions, such as medial collateral ligament injury, patellar instability and accelerated degenerative joint disease.
Genu valgum is diagnosed based on standing full-length radiographs of the bilateral lower extremities. The mechanical axis is drawn from the center of the femoral head to the center of the tibiotalar joint. Genu valgum is diagnosed when the mechanical axis falls lateral to the center of the knee.
The magnitude of the deformity can be assessed by tibiofemoral angle (the angle of the anatomical axes of the femur and tibia) as well as intermalleolar distance (the distance between the medial malleoli when medial femoral condyles are touching).
The mechanical lateral distal femoral angle (mLDFA) and medial proximal tibial angle (MPTA) — the angles formed by the mechanical axes and articular surfaces of the femur and tibia, respectively — can help assess an underlying femoral or tibial cause of the deformity.
Advertisement
Treatment is generally considered when the tibiofemoral angle is greater than 15 degrees or the intermalleolar distance is greater than 8 cm.
The method of treating idiopathic genu valgum depends on both the timing of presentation and the severity of the deformity. Ideally, the condition is diagnosed before the child approaches skeletal maturity, allowing for simple growth modulation procedures as opposed to the more significant osteotomies required after physeal closure.
Transient hemiepiphysiodesis is the most common of these growth modulation procedures. Techniques typically involve tension-band plating, staples or transphyseal screws. These techniques all rely on the Hueter-Volkmann principle, which states that increased mechanical stress on a physis leads to decreased bone growth.
In the case of genu valgum, by applying hardware to the medial distal femoral and/or medial proximal tibial physes, growth is slowed medially but allowed to progress in the lateral physes. Therefore, coronal angulation is corrected over time.
Patients must be followed closely (every three to four months) to ensure appropriate deformity correction and avoid overcorrection. Once the patient reaches a neutral mechanical axis or is slightly overcorrected to mild genu varum, the hardware is removed. Slight overcorrection is sometimes helpful because a small percentage of patients have rebound phenomenon and redevelop some degree of genu valgum after hardware removal.
A 14-year-old male presented with complaints of progression of genu valgum, with his left knee more pronounced than his right. The mechanical axes passed through the lateral knee bilaterally.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/af0b86f8-8811-45d1-aed4-9faead38bc30/Genu-valgum-inset1)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3dba9efd-06bc-4a3b-99d3-3a62808de806/Genu-valgum-inset2)
Measurements were as follows:
| Left | Right | |
|---|---|---|
| Tibiofemoral angle | 15 degrees | 13 degrees |
| mLDFA | 82 degrees | 84 degrees |
| MPTA | 89 degrees | 89 degrees |
| Tibiofemoral angle | ||
| Left | ||
| 15 degrees | ||
| Right | ||
| 13 degrees | ||
| mLDFA | ||
| Left | ||
| 82 degrees | ||
| Right | ||
| 84 degrees | ||
| MPTA | ||
| Left | ||
| 89 degrees | ||
| Right | ||
| 89 degrees |
Due to the predominantly femoral-induced genu valgum, as well as more significant deformity on the left side with questionable growth potential remaining, the decision was made to proceed with bilateral medial distal femur and left medial proximal tibia transient hemiepiphysiodesis with tension-band plating.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/37dc36a0-c994-42d9-bbe9-5a3731219e71/Genu-valgum-inset3)
The patient was followed postoperatively every four months with full-length bilateral lower extremity radiographs to assess for correction and timing of plate removal. After approximately one year of growth, the patient achieved a neutral mechanical axis, and plates were removed.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/03c824cb-992d-443e-8705-8fbe3c52dbad/Genu-valgum-inset4)
Dr. Gurd is a pediatric orthopaedic surgeon at Cleveland Clinic. Dr. Paez is a resident in Cleveland Clinic’s Department of Orthopaedic Surgery.
Advertisement
Advertisement
Computer simulation identifies causes of instability
Youth and open physes are two factors that increase risk of recurrence
Step counts suggest recovery is more variable and individualized than commonly believed
Largest cohorts to date reveal low rates of major complications
Study reports zero infections in nearly 300 patients
Cleveland Clinic’s Global Peak Performance Center and PGA TOUR partnership pair advanced assessment with longitudinal follow-up to enhance clinical decision-making
Study highlights the need for objective functional measures as value-based care expands
Reduces likelihood of achieving CMS-defined substantial clinical benefit at one year