Clinical features that should make clinicians suspect vasculopathy
by Carol A. Langford, MD, MHS, FACP
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You are asked to see a 55-year-old male who presented to the emergency room with acute abdominal pain. He was previously well prior to the onset of the pain and had no significant past medical or surgical history. Computed tomography angiography revealed evidence of hemoperitoneum from a ruptured splenic artery aneurysm with evidence of dissections involving the superior mesenteric artery and left renal artery. He was taken to surgery and his team consults you for the question of whether these vascular abnormalities are due to vasculitis.
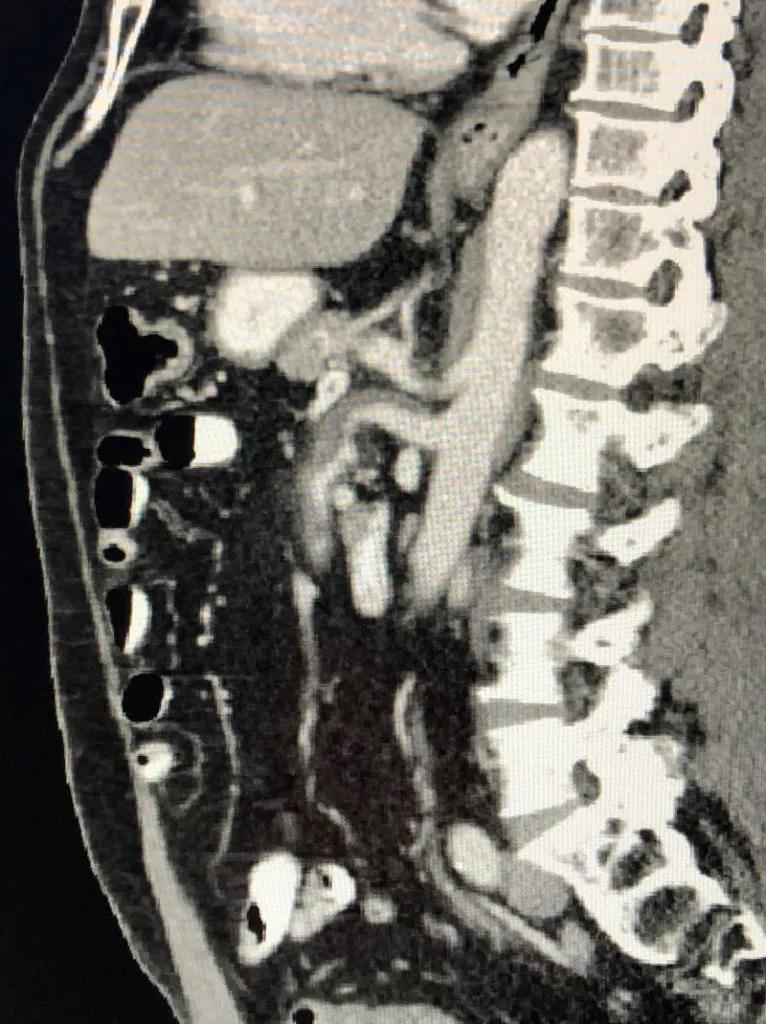
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d8e8be7e-a74a-4a14-b247-90c9fd3b83a8/21-RHE-2109968-Langford_vasculopathy-CQD-Inset_800x1070-766x1024_jpg)
CT abdomen – sagittal view demonstrating dissection of the superior mesenteric artery
In considering the cause of aneurysms, dissections, stenoses or occlusions in the large- or medium-sized vessels, it is appropriate to include vasculitis in the differential diagnosis. However, in addition to atherosclerosis, there are a range of less common vasculopathic disease entities that should also be considered, particularly if features atypical for vasculitis are present. The importance in identifying a vasculopathy is that these would not be treated with systemic immunosuppression and may have their own approach to management.
| Atherosclerosis |
|---|
| Heritable vascular disorders |
| Vascular Ehlers-Danlos syndrome |
| Marfan syndrome |
| Loeys-Dietz syndrome |
| Grange syndrome |
| Neurofibromatosis |
| Pseudoxanthoma elasticum |
| Arterial tortuosity syndrome |
| Erdheim-Chester disease |
| Fibromuscular dysplasia |
| Segmental arterial mediolysis (SAM) |
| Atherosclerosis |
| Heritable vascular disorders |
| Vascular Ehlers-Danlos syndrome |
| Marfan syndrome |
| Loeys-Dietz syndrome |
| Grange syndrome |
| Neurofibromatosis |
| Pseudoxanthoma elasticum |
| Arterial tortuosity syndrome |
| Erdheim-Chester disease |
| Fibromuscular dysplasia |
| Segmental arterial mediolysis (SAM) |
Causes of vasculopathy that can affect the medium- to large-sized vessels
In reviewing the key elements in our patient, he was well until he experienced the severe onset of abdominal pain. There were no prodromal features or prior vascular events. His ESR and CRP were elevated on first measurement but rapidly returned to normal. Review of the vascular lesions were notable for vessel dissections involving more than one vessel, predominantly in the visceral circulation. Multiple tissue sections were reviewed from his emergency surgery, which revealed areas of medial breakdown in the muscular arteries with associated aneurysm formation and adjacent areas of organizing granulation tissue. Collectively, these features argued against a vasculitis and supported a diagnosis of segmental arterial mediolysis (SAM).
Advertisement
SAM is a rare non-inflammatory vascular disorder of unknown cause that manifests as an arterial dissection, aneurysm, stenosis or occlusion involving muscular arteries. This most commonly involves the visceral arteries and less often the renal, coronary or cerebral circulation.1,2,3 In adults, SAM may present at any age and has a slightly higher frequency in men. Presentations are typically acute and can be severe with visceral organ infarction, vascular dissection or intra-abdominal hemorrhage. The diagnosis of SAM is based on histology where it is defined by the presence of vacuolar degeneration of the vessel media with subsequent mediolysis. This can lead to “gap aneurysms” that are at risk of rupture as well as mural hemorrhage or dissecting hematomas of the artery wall. In the reparative phase, fibrous granulation tissue replaces areas of medial loss. Treatment is based on management of the acute event, cautious application of treatment principles for dissection when present, and optimization of vascular risk factors such as blood pressure and atherosclerosis.
SAM presents a significant diagnostic challenge as it is rare, it can present in a similar manner to other more common disease entities, and as obtaining tissue for histology is frequently not possible.4 The diagnosis of SAM as well as other complex medium- and large-vessel vascular disorders requires a multidisciplinary approach involving rheumatology, vascular medicine, vascular and cardiothoracic surgery, radiology and genetics. Particularly in the setting of acute presentation, such collaboration is essential in establishing the most likely diagnosis and optimizing patient management.
Advertisement
Advertisement
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis