No differences in patient-reported physical functioning at one year
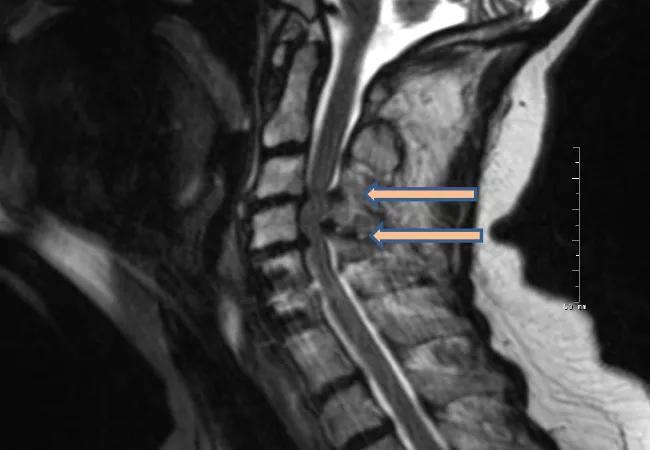
One year after surgery for cervical spondylotic myelopathy, patients report similar improvement in physical and general health measures regardless of whether they underwent a ventral or dorsal surgical approach. That’s the primary finding of the multicenter randomized Cervical Spondylotic Myelopathy Surgical (CSM-S) trial, believed to be the first randomized study to compare alternative surgical approaches for this common condition. Results of the trial were published in the Journal of the American Medical Association (2021;325:942-951).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Recent attention has focused on patient-reported quality of life for assessing surgical outcomes,” says the study’s senior author, Edward Benzel, MD, a neurosurgeon with Cleveland Clinic’s Center for Spine Health. “Ascertaining such information is especially important for cervical spondylotic myelopathy, given how often surgery is performed for this condition and the considerable practice variation in approaches.”
Cervical spondylotic myelopathy, the most common cause of spinal cord dysfunction, is frequently treated surgically in severe or progressive cases to decompress the spinal cord. In the U.S., ventral and dorsal decompression/fusion are the most common surgical interventions, but operations result in unsatisfactory outcomes in 30% of patients and frequently entail complications.
Evidence to date has failed to consistently show either the ventral or dorsal surgical approach to be superior to the other. The CSM-S trial was undertaken to compare the two strategies in terms of patient-reported physical functioning at one year.
The trial included patients with multilevel cervical spondylotic myelopathy from 14 large hospitals in the U.S. and one in Canada from April 2014 to March 2018. Patients were followed for up to two years.
The study’s 163 patients (mean age, 62 years; 49% women) were randomized to either ventral surgery (n = 63) or dorsal surgery (n = 100). Ventral surgery consisted of anterior cervical disk removal with instrumented fusion. Dorsal surgery consisted of either laminectomy with instrumented fusion or open-door laminoplasty, with the choice left to the surgeon’s discretion. Because of this variability in dorsal approaches, randomization followed a 2:3 scheme with more patients assigned to dorsal surgery.
Advertisement
One-year follow-up was conducted in 95% of study participants, and 80% completed two-year follow-up.
The primary outcome was one-year change in the physical component summary score of the Short Form 36 Survey (SF-36 PCS), which assesses patient-reported physical functioning, limitations in work and activities due to pain, and physical and general health. Scores range from 0 to 100, with a change of 5 points or more considered clinically meaningful.
Mean improvements in one-year SF-36 PCS scores were not significantly different between the ventral surgery cohort (5.9 points) and the dorsal surgery group (6.2 points) (P = 0.86).
When the cohorts were compared across seven prespecified secondary outcomes, there were no significant differences between the groups on six of the outcomes — specifically, the modified Japanese Orthopaedic Association scale score, the Neck Disability Index, the EuroQol 5 Dimensions score, sagittal vertical axis, work status and heath resource utilization. The one exception was risk of any complications, which was significantly higher in the ventral surgery group than in the dorsal surgery group (48% vs. 24%; P = 0.002), driven largely by an excess of dysphagia with ventral surgery. There was no significant difference in incidence of major complications.
Dr. Benzel emphasizes two major points from this trial:
Advertisement
The authors note that laminoplasty is preferred over ventral or dorsal fusion more often in Asia and Europe than in North America. Because of the small number of centers using laminoplasty in this study (five) and the nonrandomized protocol within the dorsal approach group, laminoplasty could not be adequately compared with the fusion procedures.
However, in nonrandomized analysis by treatment type, laminoplasty was associated with significantly better patient-reported functioning, fewer complications and less health resource utilization. The authors also note that reimbursement for laminoplasty is lower than for fusion in the U.S.
“Our findings on laminoplasty should be interpreted with caution,” Dr. Benzel concludes. “A more extensive evaluation — encompassing clinical and economic considerations — is needed to compare these three alternative surgical approaches. At the same time, the results associated with laminoplasty are very promising.”
Advertisement
Advertisement

An argument for clarifying the nomenclature

An expert talks through the benefits, limits and unresolved questions of an evolving technology

Recommendations on identifying and managing neurodevelopmental and related challenges

Phase 2 trials investigate sitagliptin and methimazole as adjuvant therapies

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits