After four decades, refinements to the gold standard of bypass continue as new insights emerge
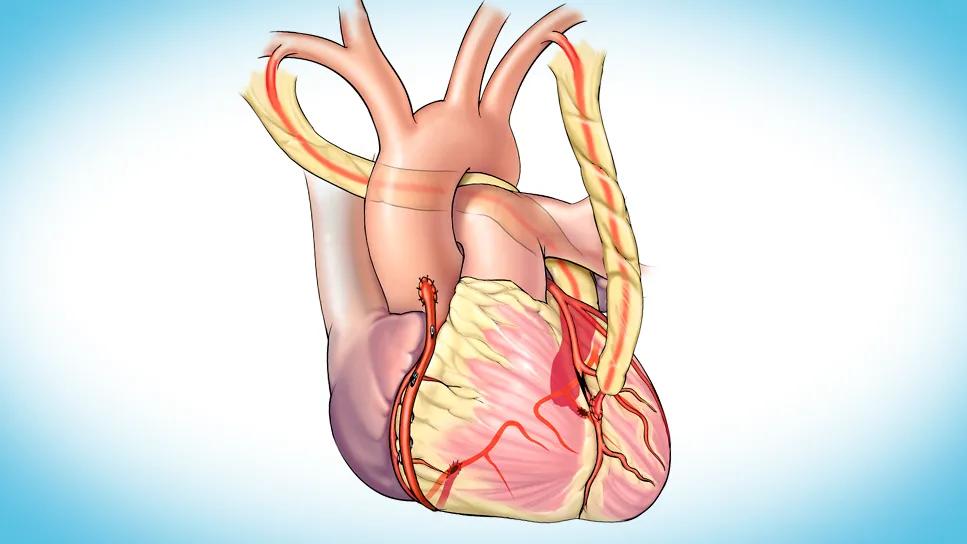
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/86a87828-b25f-4cd9-9be5-611c7a04c3ae/26-HVI-7629460-ima-grafting)
illustration of heart showing arterial grafts
Forty years after the landmark New England Journal of Medicine (NEJM) study by Loop and colleagues established IMA-to-LAD bypass as the gold standard for coronary artery bypass graft surgery (CABG), this grafting method remains the most robust and lasting method for coronary revascularization available to patients.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
So contends a team of Cleveland Clinic authors led by Faisal Bakaeen, MD, in a new “viewpoint” review in JAMA Surgery that traces the evolution of CABG before and after the seminal NEJM paper and details still-emerging insights about the procedure’s broad benefits.
“The internal mammary artery [IMA]-to-left anterior descending artery [LAD] graft provides not only superior long-term survival and graft patency but also unique prophylactic protection against future atherosclerotic events that alternative therapies cannot match,” says Dr. Bakaeen, Director of Cleveland Clinic’s Coronary Artery Bypass Surgery Center.
The journey toward establishing the IMA as the preferred CABG conduit spanned several decades of innovation. Early attempts at direct myocardial implantation by Arthur Vineberg in 1950 paved the way for more sophisticated connections. By the 1960s, pioneers like Goetz and Kolesov were performing direct IMA-to-coronary anastomoses, paving the way for Cleveland Clinic’s Rene Favaloro, MD, to popularize CABG using various arterial and venous grafts by the late 1960s.
However, the definitive evidence required to change global practice arrived in 1986 with the NEJM study by Loop and colleagues, also at Cleveland Clinic. Prior to this, many surgeons avoided the IMA due to the meticulous tissue handling and technical skill needed for harvesting and anastomosis, which were more daunting than what was required by simpler saphenous vein grafts. The 1986 study provided the conclusive verdict that transformed anecdotal observations of IMA durability into a standard quality metric for cardiac surgery.
Advertisement
The 1986 investigation was an observational study involving a massive cohort of 5,931 CABG patients at Cleveland Clinic. The researchers compared 2,306 patients who received an IMA-to-LAD graft (sometimes supplemented by vein grafts) with 3,625 patients who received only vein grafts. The results were stark and statistically significant across all levels of disease complexity:
Additionally, patients relying solely on vein grafts faced a 1.6 times higher risk of mortality and a 1.4 times greater risk of suffering a late myocardial infarction. Angiographic data provided mechanistic confirmation, as IMA grafts demonstrated a 96.0% patency rate while vein grafts to the LAD showed only 81.1% patency over the same period.
“For cardiovascular clinicians, understanding why the IMA succeeds where other vessels may fail is critical for patient counseling,” notes Cleveland Clinic interventional cardiologist Laura Young, MD, a co-author of the new JAMA Surgery paper. “Unlike saphenous veins or other arteries, the IMA possesses inherent histologic properties that grant it a relative immunity to atherosclerosis. Also, the IMA maintains a continuous basal production of nitric oxide, which serves to reduce endothelial dysfunction and promote vascular health.”
Advertisement
This biological resilience means that, barring a rare technical error during surgery, blood flow is typically compromised only by progressive disease in the native vessel distal to the anastomosis. “The result is that the IMA-to-LAD graft provides a ‘lifetime warranty’ of sorts for the most critical territory of the heart,” Dr. Bakaeen observes.
A key distinction for clinicians to consider when choosing between CABG and percutaneous coronary intervention (PCI) is the scope of protection. The authors note that PCI is essentially a segmental therapy focused on the specific area of stent deployment, whereas IMA-to-LAD bypass can offer broader prophylactic benefits.
By placing the IMA at a mid-to-distal position on the LAD, surgeons bypass not only the current flow-limiting lesions but also any potential “culprit” lesions that may develop upstream in the future. “This protective reach can extend even further,” Dr. Bakaeen adds. “Through the development of arterial collateralization over time, a single IMA-to-LAD graft can become the primary life-sustaining source of blood for the entire myocardium in patients with totally occluded native circulation.”
Building on the success of the single IMA, the Cleveland Clinic authors of the 1986 study soon explored the merits of bilateral internal mammary artery (BIMA) grafting. By the late 1990s they demonstrated in a retrospective study (J Thorac Cardiovasc Surg. 1999;117:855-872) that using two IMAs can further reduce the need for reoperation and improve survival, particularly when all major coronary vessels are bypassed with arterial conduits.
Advertisement
However, adoption has been slowed by the Arterial Revascularization Trial, which did not show a clear advantage for BIMA over single IMA at 10 years. Many experts argue that these results were confounded by high rates of treatment arm crossover and the use of radial artery grafts in the single-IMA group. To mitigate the risk of sternal wound complications — a common concern with BIMA — surgeons increasingly use skeletonized harvesting, which preserves collateral blood flow to the sternum.
For patients seeking less-invasive options, interest is mounting in a hybrid approach that combines a minimally invasive IMA-to-LAD bypass (sometimes with robotic assistance) with stenting to treat non-LAD lesions. While this avoids a full sternotomy, wider adoption requires more robust evidence, the authors of the JAMA Surgery review note.
The appeal of hybrid approaches reflects a shift beyond what the review authors call “the simplistic view” that PCI and CABG are competing alternatives for revascularization. “It’s increasingly appreciated that these modalities are often complementary to each other,” notes Dr. Young. “PCI is particularly valuable in the acute setting and in cases of symptomatic atherosclerosis with low- and moderate-complexity lesions. CABG is particularly valuable for extensive, complex coronary artery disease involving multiple vessels in patients who can tolerate surgery.”
“While the IMA-to-LAD bypass has reigned as the most effective intervention for severe coronary disease for four decades now, the most enduring legacy of the study that established it may be the endorsement of a data-driven, heart-team-based approach to revascularization care,” Dr. Bakaeen concludes.
Advertisement
Advertisement
BITA grafts themselves are rarely to blame, and outcomes can be good
Two cardiac surgeons explain Cleveland Clinic’s philosophy of maximizing arterial graft use
Cleveland Clinic-pioneered repair technique restores a 61-year-old to energetic activity
Study indicates lower in-hospital mortality and better long-term survival
How Cleveland Clinic supported an alliance hospital to improve early extubation practices
Why and how we’re using robotic assistance for qualifying CABG candidates
Findings undercut perceptions of radial artery as second conduit of choice
The case for a thoughtful approach to CTO and minimally invasive options for CABG