Early projects include predicting cardiac arrest, kidney injury and low cardiac output syndrome after surgery
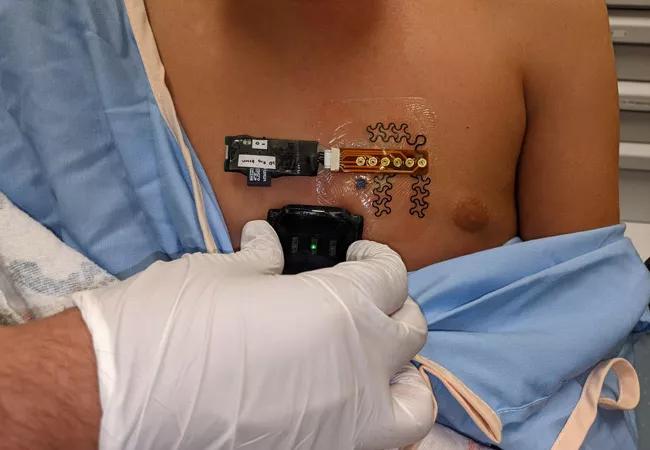
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/842d4444-3682-44ad-9c98-670f76b1522f/CQD-4408475-C4AI-650x450-1_jpg)
CQD-4408475-C4AI-650×450
A group of Cleveland Clinic physicians and researchers have launched Cleveland Clinic Children’s Center for Artificial Intelligence (C4AI) to develop innovative technology and algorithms for managing congenital heart disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“There are new technologies that are being developed in the healthcare space, but very few for children and adults with congenital heart disease,” says Animesh (Aashoo) Tandon, MD, MS, Director of Cardiovascular Innovation at Cleveland Clinic Children’s. “Our goal is to bring these new technologies to our patients as well.”
Although machine learning, also known as artificial intelligence (AI), is a broad tool, Dr. Tandon believes its greatest advantage is that it doesn’t have to follow specific rules to pinpoint relationships within data. This could be especially beneficial for patients with congenital heart disease because they have such complex life histories.
“Some of our patients have surgery within one week of being born, and we’re trying to figure out what’s going to happen to them 30 or 40 years later,” says Dr. Tandon. “That requires tools that are outside our conventional statistical toolbox.”
C4AI has existed in its present form for more than two years, with faculty members including Dr. Tandon; Tara Karamlou, MD; Orkun Baloglu, MD; Samir Latifi, MD; and Bradley Marino, MD, MBA. Dr. Tandon says the team is currently working to accelerate C4AI’s growth by hiring people to help curate, organize and analyze data.
Meanwhile, the center has two ongoing projects — one focused on predictive analytics and the other on detecting low cardiac output syndrome (LCOS) after surgery for congenital heart disease.
Research led by Dr. Baloglu uses mathematical modeling and machine learning techniques to predict and potentially prevent adverse events such as cardiac arrest in intensive care unit patients. More recently, the team developed a machine learning model that predicts acute kidney injury after cardiac surgery in children.
Advertisement
“It gathers all information from the pre-operative, intra-operative and immediate postoperative periods and predicts if the patient will have kidney injury two days after the surgery,” says Dr. Baloglu.
The subsequent retrospective study, published in Pediatric Nephrology, found promising results in AI’s ability to predict moderate to severe cardiac surgery-associated acute kidney injury. Dr. Baloglu says the next goal is to use this kidney model in real life to see if it’s as adept at predicting prospective data as it is with retrospective data.
“I don’t see any reason why it wouldn’t be,” he says. “And then maybe even a step further: Can we change patient care based on this model’s prediction? For example, can we change our ICU care to prevent kidney injury if the model says this patient is going to have kidney injury two days later?”
The research team also has tested their novel situational awareness scoring system (an algorithm that evaluates patients’ risk of cardiac arrest in the ICU) in adult patients. They found positive results similar to those found in children.
“What we’re developing for pediatric cardiology patients looks like it’s also very promising for adult patients,” Dr. Baloglu says.
Drs. Tandon and Baloglu have been leading a project for more than one year on LCOS detection using wearable biosensor technologies.
“We now have the bedside data aggregation platform set up, so every minute of every patient’s data from our ICU gets stored in a computer,” Dr. Tandon says.
Advertisement
There has also been progress in getting noninvasive sensors approved for use at Cleveland Clinic.
“Not only do we have a way to collect certain kinds of data, but we also have novel sensing mechanisms that will give us different physiologic insights than are available at other centers,” explains Dr. Tandon.
In terms of data infrastructure, Dr. Karamlou has acquired substantial national and surgical databases that will allow them to identify patterns between large numbers of patients, as well as large amounts of data from the same patient.
“We’re trying both of these strategies — breadth and depth — to get enough data to draw these inferences from AI techniques and really dig into the physiology for our patients,” Dr. Tandon says. “I think this approach is going to help us find the sweet spots where we can greatly push the field forward.”
“We’re really at a crossroads for pediatric cardiology and congenital heart disease,” says Dr. Tandon. While AI techniques exist and have been developed at scale for adults, “with kids and smaller populations like congenital heart disease, we don’t have enough data to just throw algorithms at them.”
C4AI will continue to create technology to curate new kinds of data and develop algorithms. However, because this particular patient population is so small, the next challenge lies in driving innovation on a national scale.
“We as a field need to figure out how we are going to share data effectively and how we are going to put multiple centers together to get enough scale,” Dr. Tandon explains. “We have to develop these technologies in a way that will be scalable outside the doors of Cleveland Clinic Children’s and change the management of patients across the country. All our projects are designed with that scope in mind.”
Advertisement
Advertisement
A new CME opportunity in Chicago, May 15-16
Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner
Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve
Reproducible technique uses native recipient tissue, avoiding risks of complex baffles
A reliable and reproducible alternative to conventional reimplantation and coronary unroofing
Program will support family-centered congenital heart disease care and staff educational opportunities
Case provides proof of concept, prevents need for future heart transplant
Pre and post-surgical CEEG in infants undergoing congenital heart surgery offers the potential for minimizing long-term neurodevelopmental injury