Compression device augments the carpal arch space
A radioulnar wrist compression device significantly relieved symptoms of carpal tunnel syndrome in a pilot study, according to an article in the Journal of Orthopaedic Translation. Patients showed significantly increased median nerve mobility, decreased distal motor latency and improved median nerve cross-sectional area after using the device for only two weeks.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“I like to refer to this intervention as aggressively conservative,” says William Seitz, MD, a hand and upper extremity surgeon and co-author on the paper. “It could revolutionize carpal tunnel treatment by eliminating the need for surgery in many cases.”
The intervention device is noninvasive, and applies compressive forces (140 mmHg or 10 N) via a medical balloon attached to a thermoplastic wrist brace. For this pilot study, patients wore the splint for three, 15-minute intervals each day, for a total of 45 minutes per day over the four-week intervention period.
Outcomes were evaluated at baseline, mid-intervention (two weeks) and at the end of the intervention (four weeks). These outcomes included measurements of median nerve mobility, median nerve conduction (distal motor latency and sensory nerve latency) and median nerve cross-sectional area, factors commonly impacted in carpal tunnel syndrome.
Median nerve mobility was significantly affected by the radioulnar wrist compression intervention. At two weeks, median nerve mobility was 1.73 times baseline measurements (p < 0.01). This improvement was sustained through week four, though no further significant improvements were observed.
After two weeks, distal motor latency improved by 10.2% to 6.27 ± 2.05 msec from 6.98 ± 2.74 msec at baseline (p < 0.05). Median nerve cross-sectional area also improved after two weeks, decreasing 19.4% to 15.2 ± 9.0 mm2 from the baseline of 18.9 ± 8.7 mm2 (p < 0.001).
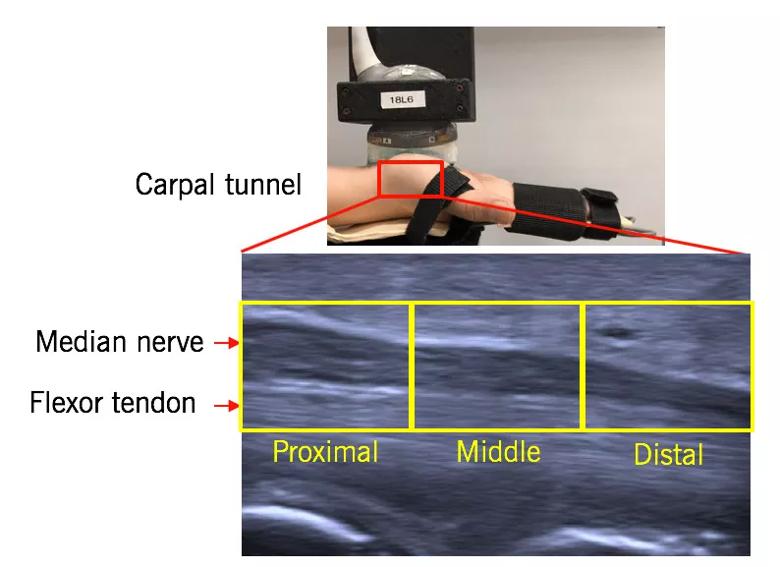
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/86ca14eb-c9a0-4cf4-8169-8ad4e525848b/19-ORT-1132-Nerve-Mobility-CQD-Inset_jpg)
“Carpal tunnel syndrome is a pressure syndrome of the nerve and wrist,” Dr. Seitz notes. “Dr. Li recognizes that if you compress the canal, putting intermittent pressure on the wrist, you can open up the volume of the carpal tunnel and give the nerve some breathing room. Night splinting gives the nerve a break, but this intervention dynamically changes the size and shape of the carpal canal to alleviate pressure on the nerve itself.”
Advertisement
“The findings support our approach of the carpal arch space augmentation (CASA) as a noninvasive option for the treatment of carpal tunnel syndrome,” states senior author Zong-Ming Li, PhD, a principal investigator in Cleveland Clinic’s Lerner Research Institute who studies orthopaedic biomechanics and rehabilitation of the hand and upper extremity.
“While we continue to investigate many aspects of CASA mechanisms, our next step is to translate our innovative CASA concept and laboratory research findings into a clinical treatment for patients with carpal tunnel syndrome. We plan to carry out a multi-site clinical trial to demonstrate the intervention’s efficacy in relieving patient symptoms and compare the CASA outcomes with other existing treatment options.”
Advertisement
Advertisement

First full characterization of kidney microbiome unlocks potential to prevent kidney stones

Researchers identify potential path to retaining chemo sensitivity

Large-scale joint study links elevated TMAO blood levels and chronic kidney disease risk over time

Investigators are developing a deep learning model to predict health outcomes in ICUs.

Preclinical work promises large-scale data with minimal bias to inform development of clinical tests

Cleveland Clinic researchers pursue answers on basic science and clinical fronts

Study suggests sex-specific pathways show potential for sex-specific therapeutic approaches

Cleveland Clinic launches Quantum Innovation Catalyzer Program to help start-up companies access advanced research technology