Young man saved multiple times by rapid collaborative response
A 36-year-old man with no remarkable medical history was transferred from an outside hospital to Cleveland Clinic with pulseless electrical activity, fulminant biventricular dysfunction (Figure) and severe malperfusion to multiple organs. Kidney and liver function were poor. The patient was immediately intubated and placed in the cardiac intensive care unit (ICU).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“This patient was about as sick as possible at presentation,’” says Aaron Weiss, MD, PhD, the Cleveland Clinic cardiothoracic surgeon who saw the patient that day and was on his care team throughout his stay. “Fortunately, we have an extremely effective cardiogenic shock team that can be activated at once.”
The Cleveland Clinic shock team consists of a multidisciplinary group of experts who can be assembled rapidly for a conference call to consult on a patient to develop a lifesaving management strategy. Among those included on the call, often with others, are a heart failure cardiologist, a heart failure cardiac surgeon and an ICU physician. A senior member of the nursing staff also listens on the line to immediately organize room placement and care preparations as needed.
The shock team can also be accessed from outside the hospital to consult on patients not in the Cleveland Clinic system. This provides expertise to colleagues and facilitates transfer to Cleveland Clinic if appropriate.
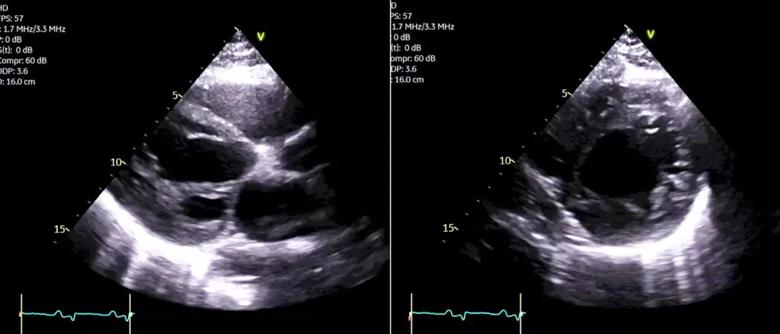
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d7da35c6-1f78-423f-b2b6-7b486637c808/23-HVI-3766948-CQD-Inset1-1024x438_jpg)
Figure. Echocardiograms at presentation revealing severe biventricular dysfunction and severe mitral regurgitation.
The shock team determined that the patient needed aggressive acute lifesaving circulatory support to buy time and help salvage his organs. He was immediately placed on the following:
The patient improved, and after two days, he was taken off ECMO. He was extubated a few days later. Although he made progress and his liver function improved, he remained on dialysis and stayed in the ICU with his heart fully dependent on the Impella 5.5 without evidence of heart recovery.
Advertisement
Soon after, the patient developed what was suspected to be heparin-induced thrombocytopenia (HIT). Initial testing was positive for HIT and he was empirically transitioned to bivalirudin therapy. The mechanical support kept the patient stable enough to wait for confirmatory testing, which was negative for HIT.
After a few weeks for further stabilization, the transplant team agreed to list him for heart and kidney transplantation due to end-stage cardiomyopathy with Impella dependence and continued renal failure. He was determined to be status 2 (hospitalized and on mechanical support).
Subsequently, the Impella device — which is not designed for use beyond more than a few weeks — failed, causing a stroke. In an emergency procedure, it was exchanged for a new one via the left axillary artery, and the patient recovered from his stroke within a few days.
Because of this complication, his transplant priority classification was upgraded to status 1 (critically ill and on mechanical support). “If the Impella failed again, it would have been much more difficult to place another device, putting his life in imminent danger without a good solution,” Dr. Weiss explains.
Ten weeks after the patient initially presented, organs became available, and he underwent a heart transplant with successful removal of the Impella 5.5. He was returned to the ICU and then underwent a kidney transplant the following day.
“Heart-kidney transplant is an unusual combination, and we probably have just a handful or so of them every year at Cleveland Clinic,” says Ventakesh Krishnamurthi, MD, who performed the renal transplant in this case. “While the surgery itself was standard, the behind-the-scenes coordination for such a complex transplantation was anything but.”
Advertisement
The patient had an uneventful recovery and was discharged a few weeks later with excellent function in both transplanted organs. Three months after transplant he was doing well at home, undergoing physical therapy and expected to be able to resume full normal activities.
“This young man went from not knowing he was sick to being the sickest patient in the hospital, to walking out the door three months later with a new heart and kidney as well as a new lease on life,” says Dr. Weiss. “This amazing trajectory could only have happened at a large tertiary center like Cleveland Clinic that emphasizes collaborative, multidisciplinary care.”
The care team highlight the following pivotal points in his care:
Advertisement
That collaborative culture also promoted an additional key to success in this case: continuity of care. “The same team that placed this patient on mechanical support also performed his heart transplant and was involved with the kidney transplant by Dr. Krishnamurthi,” says Dr. Weiss. “That type of continuity can be invaluable in a complex case like this.”
Advertisement
Advertisement

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world

Consensus statement aims to increase use of the perfusion technology and raise transplant volumes

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

AHA recommendations for pretransplant evaluation, peritransplant and long-term management

First-ever procedure restores patient’s health

The agent-based model aims to improve prediction accuracy
New guidelines expand on psychosocial, sexual health, cognitive and other issues