Innovative procedure reduces scarring, recovery time and nipple sensation
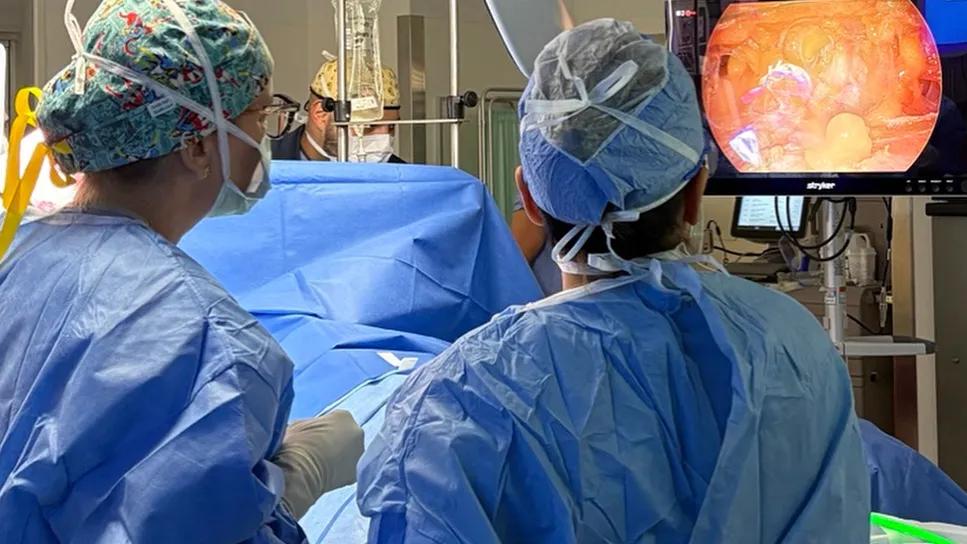
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/761362ed-3950-4a4f-8809-e44c62490dcf/surgery-endoscopic-nipple-sparing)
Endoscopic nipple-sparing mastectomy
A 46-year-old patient who was at high risk of developing breast cancer was among the first in the U.S. to undergo an endoscopic nipple-sparing procedure. This procedure helps to preserve the nipple, areola and skin. This prophylactic bilateral surgery benefited both the patient and surgeon, allowing for better visualization during the procedure as well as faster healing and less scarring.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The patient had a significant family history of breast cancer as well as dense breasts, which can be difficult to accurately image. After finding a lump in her breast, she was seen at a high-risk breast cancer clinic. Fortunately, they confirmed that the lump was benign.
However, given her family history of breast cancer, as well as subsequent tests revealing that she had the BRCA mutation, the clinic recommended taking tamoxifen as a preventative measure. The patient did not want to take medication, and she sought a second opinion at Cleveland Clinic Cancer Institute.
Paula Escobar, MD, a breast surgical oncologist at Cleveland Clinic, examined the patient and felt she was a good candidate for endoscopic nipple-sparing mastectomy. The procedure has been broadly used in Europe and Asia but is new to the U.S.
This procedure is not appropriate for all patients. Those with very large breasts, breast ptosis and/or a tumor near the nipple cannot undergo this surgery. For those patients who do meet the surgical criteria, this procedure can have several advantages, including faster healing time and, in some cases, more remaining sensation in the skin and nipple.
Dr. Escobar discussed the benefits and risks with the patient, who agreed it was the right choice for her. She underwent a prophylactic bilateral endoscopic nipple-sparing procedure, immediately followed by breast reconstruction.
With an endoscopic nipple-sparing mastectomy, no special instrumentation is needed. The surgeon extends the use of proven technology and instruments that are employed in other laparoscopic surgeries. The surgeon uses a mini access point device that can accommodate multiple devices via a single port.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/502e68a6-a5e0-408f-a1d2-2bba85182965/medical-illustration-endoscopic-nipple-sparing-inset)
For this case, Dr. Escobar made a 3 cm incision on the inframammary fold so it was completely hidden. Since the incision was much smaller than with open surgery, which is typically 10cm, the risk of scarring, infection, flap issues or skin necrosis was much lower.
Dr. Escobar then folded up the access point device and inserted the device through the incision, attaching it to the trocar. The breast was then inflated using low-pressure CO2 for better visualization. “Since the area is inflated, we can see the vessels so there’s less trauma to the skin and to the nipple. We can also feel the flap while performing surgery, enabling us to work more efficiently. If there were to be a tear or a leak, I could address it immediately,” says Dr. Escobar. The surgery to remove the breasts went smoothly.
Risal Djohan, MD, a plastic surgeon with Cleveland Clinic, then performed the breast reconstruction the same day. Healing time was faster with this procedure because, unlike in open surgery, the implants weren’t putting pressure on the incision.
Both procedures had a positive outcome. The patient had drains placed briefly and was discharged within 24 hours of the surgery. She was able to return to work two weeks later. In addition, the scar is much less visible than it would have been with open surgery. The patient reported being pleased with the results.
Looking back on one of the first cases of endoscopic nipple-sparing mastectomy in the U.S., Dr. Escobar shared several takeaways:
Select oncologically-appropriate patients. Not all patients are suitable for this technique. If there’s a tumor with skin involvement or in close proximity to the nipple, this procedure would not be the right choice. This may be an option for patients seeking preventative or therapeutic mastectomy depending on their health status, body mass index, comorbidities as well as tumor size and location.
Advertisement
Work closely with your plastic surgeon. “Plastic surgeons are accustomed to performing reconstructions with ten-centimeter incisions,” explains Dr. Escobar. “Now we’re challenging them to do so with a three-centimeter incision. For this procedure, Dr. Djohan and I had discussions together to come up with a surgical plan.”
Involve the whole team. Education and collaboration are necessary. Time and experience have shown that minimally-invasive surgeries are superior for procedures involving the appendix and gall bladder. This approach has been used for breast surgeries for years in other countries but is relatively new to the U.S.
“There are a lot of people involved in these cases, from the genetic counselor to the medical oncologist to the surgeon,” says Dr. Escobar. “It’s essential that everyone involved understands the reason for minimally-invasive surgery and is well aligned on the approach and expectations. Teamwork is crucial for implementing this procedure in the clinic.”
This technique is expanding beyond nipple-sparing mastectomies and in the future will also be used to perform sentinel node biopsies.
Advertisement
Advertisement
Research underscores the importance of access to timely diagnosis and treatment in this patient population.
A Cleveland Clinic model combining clinical staging, genomics and AI predicts survival with 18% greater accuracy — and could help match patients to more effective treatments.
Study serves as ‘cautionary tale’ for physicians tempted to rely on liquid biopsy results alone
Direct delivery of viral-based vector KB707 to the lungs may boost anti-tumor response and help overcome immune checkpoint inhibitor resistance
Evidence-based recommendations for managing pain, nausea and other treatment reactions
Emerging data and practice changes reduce toxicity burden of treatment
Understanding supports for adolescent and young adult patients
Reframing cancer survivorship